New Part 4 (765-865) (765-1019) NR 7

Comprehensive Medical Knowledge Quiz
Test your medical knowledge with our in-depth quiz featuring 59 thoughtfully crafted questions. Designed for healthcare professionals and students alike, this quiz covers a broad spectrum of medical topics including diabetes management, endocrinology, and patient care.
Challenge yourself and see how well you understand important medical concepts. Enhance your learning experience by:
- Exploring diverse medical scenarios
- Improving your clinical reasoning skills
- Preparing for exams or certifications
A 30-year-old Caucasian female comes to the physician's office because of polyuria and polydipsia of recent onset. She has no other medical problems. She does not use tobacco, alcohol or drugs. She has no known drug allergies. Her mother has diabetes. Her temperature is 36.7°C (98°F), pulse is 75/min, blood pressure is 110/70 mmHg, and respirations are 15/min. The initial lab results are: Hb 12.7 g/dl, WBC 5,000 /cmm, Platelets 380,000/cmm, Blood glucose 90 mg/dl, Serum sodium 142 mEq/L, Serum potassium 4.0 mEq/L, Bicarbonate 26 mEq/L, BUN 15 mg/dl, Serum creatinine 0.9 mg/dl, Serum uric acid 9 mg/dl, Serum osmolality 295 mOsm/kg, Urine osmolality 160 mOsm/kg. After 12 hours of water deprivation, lab testing reveals:Serum sodium 151 mEq/L, Serum potassium 4.2 mEq/L, Bicarbonate 26 mEq/L, Serum osmolality 300 mOsm/kg, Urine osmolality 186 mOsm/kg. One hour after the subcutaneous administration of arginine vasopressin, the urine osmolality is 400mosm/kg. Which of the following is the most appropriate treatment for this patient?
Intranasal desmopressin acetate
Psychotherapy
Indomethacin
Hydrochlorothiazide
Demeclocycline
A 42-year-old woman with no significant past medical history presents for a routine health maintenance visit. On physical examination a solitary nodule is palpated in the thyroid. She denies pain, dysphagia, or hoarseness. She also denies fatigue, weight change, heat or cold intolerance, diarrhea, or constipation. There is no family history of thyroid cancer. Her serum thyroid-stimulating hormone level is normal. Which of the following is the most appropriate next step in evaluation?
Fine-needle aspiration
MRI
Radionuclide scan
Thyroid lobectomy
Ultrasonography
A patient comes to your office for a new-patient visit. He has moved recently to your city due to a job promotion. His last annual examination was 1 month prior to his move. He received a letter from his primary physician stating that laboratory workup had revealed an elevated alkaline phosphatase and that he needed to have this evaluated by a physician in his new location. On questioning, his only complaint is pain below the knee that has not improved with over-the-counter medications. The pain increases with standing. He denies trauma to the area. On examination you note slight warmth just below the knee, no deformity or effusion of the knee joint, and full ROM of the knee without pain. You order an x-ray, which shows cortical thickening of the superior fibula and sclerotic changes. Laboratory evaluation shows an elevated alkaline phosphatase of 297 mg/dL with an otherwise normal metabolic panel. Which of the following is the treatment of choice for this patient?
A bisphosphonate
Observation
Nonsteroidal anti-inflammatory
Melphalan and prednisone
Ursodeoxycholic acid (UDCA)
Your patient is a 48-year-old Hispanic male with a 4-year history of diabetes mellitus type 2. He is currently utilizing NPH insulin/Regular insulin 40/20 units prior to breakfast and 20/10 units prior to supper. His supper time has become variable due to a new job and ranges from 5 to 8 PM. In reviewing his glucose diary, you note some very low readings (40-60 mg/dL) during the past few weeks at 3 AM. When he awakens to urinate, he feels sweaty or jittery so has been checking a fingerstick blood glucose. Morning glucose levels following these episodes are always higher (200-250) than his average fasting glucose level (120-150). Which change in his insulin regimen is most likely to resolve this patient’s early AM hypoglycemic episodes?
Change regimen to glargine at bedtime with lispro prior to each meal
Increase morning NPH and decrease evening NPH
Decrease morning NPH and decrease evening regular insulin
Change regimen to glargine at bedtime and continue morning and evening regular insulin
Discontinue both NPH and regular insulin; implement sliding scale regular insulin with meals
A 32-year-old G2P1 woman at 16 weeks gestation presents to her obstetrician complaining of fatigue, anxiety, and palpitations. She says she has been feeling warm, even in her air-conditioned home, and has been having three or four loose stools per day, as compared to one or two prior to her pregnancy. She has a temperature of 37.1°C (98.9°F), heart rate of 105/min, and blood pressure of 128/76 mmHg. Neck examination reveals mild diffuse enlargement of the thyroid gland with no lymphadenopathy. Relevant laboratory findings include a total triiodothyronine level of 400 ng/dL, free thyroxine of 6.8 ng/dL, and thyroid-stimulating hormone of 0.01 μU/mL (normal: 0.4–4 μU/L). Results of a thyroid- stimulating hormone-receptor antibody test are positive. Which of the following is the most appropriate therapy for this patient?
Propylthiouracil
High-dose iodine therapy
Methimazole
Radioiodine ablation
Surgical resection
A 50-year-old female is 5 ft 7 in tall and weighs 185 lb. There is a family history of diabetes mellitus. Fasting blood glucose (FBG) is 160 mg/dL and 155 mg/dL on two occasions. HgA1c is 7.8%. You educate the patient on medical nutrition therapy. She returns for reevaluation in 8 weeks. She states she has followed diet and exercise recommendations but her FBG remains between 130 and 140 and HgA1C is 7.3%. She is asymptomatic, and physical examination shows no abnormalities. Which of the following is the treatment of choice?
Metformin
Insulin
Encourage compliance with medical nutrition therapy
Observation with repeat HgA1C in 6 weeks.
Thiazolidinediones
A 49-year-old woman presents to her physician’s office with a long-standing history of polydipsia, polyuria, central obesity, and hyperlipidemia. She is currently taking metformin, a sulfonylurea, and an angiotensin-converting enzyme (ACE) inhibitor. ACE inhibitors are most beneficial in preventing or slowing the progression of which of the following diabetic complications?
Diabetic nephropathy
Diabetic ketoacidosis
Diabetic neuropathy
Diabetic retinopathy
Peripheral vascular disease
A 42-year-old woman presents to her physician with complaints of fever (38.2°C [100.8°F]) and mild-to-moderate anterior neck pain. On examination the physician finds her to be tachycardic and sweating, and to have an exquisitely tender thyroid gland. Her blood work shows a depressed thyroid-stimulating hormone level and increased free thyroxine. Which of the following is the most appropriate treatment at this time?
Ibuprofen
Acetaminophen
Levothyroxine
Prednisone
Radioactive iodine
A 53-year-old woman suffers from long-standing obesity complicated by DJD of the knees, making it difficult for her to exercise. Recently her fasting blood glucose values have been 148 mg/dL and 155 mg/dL; you tell her that she has developed type 2 diabetes. She wonders if diet will allow her to avoid medications. In addition, her daughter also suffers from obesity and has impaired fasting glucose, and the patient wonders about the management of her prediabetes. Which of the following is a correct statement based on the American Diabetes Association 2008 guidelines regarding nutrition recommendations and interventions for diabetes?
Outcomes studies show that medical nutrition therapy (MNT) can produce a 1 to 2-point decrease in hemoglobin A1c in type 2 diabetics
Low-carbohydrate diets such as “South Beach” and “Atkins” should be avoided
Prediabetic patients should be instructed to lose weight and exercise but a referral to a medical nutritionist is not necessary until full-blown diabetes is diagnosed
Very low-calorie diets (< 800 cal/day) produce weight loss that is usually maintained after the diabetic patient returns to a self-selected diet
Bariatric surgery may be considered for patients with type 2 diabetes and a BMI of > 30 kg/m2
A 45-year-old G2P2 female presents for annual examination. She reports regular menstrual cycles lasting 3 to 5 days. She exercises 5 times per week and reports no difficulty sleeping. Her weight is stable 140 lbs and she is 5 ft 8 in tall. Physical examination is unremarkable. Laboratory studies are normal with the exception of a TSH value of 6.6 mU/L (normal 0.4-4.0 mU/L). Which of the following represents the best option for management of this patient’s elevated TSH?
Repeat TSH in 3 months and reassess for signs of hypothyroidism
Begin low dose levothyroxine (25-50 μg/d)
Recommend dietary iodide supplementation
Order thyroid uptake scan
Measure thyroid peroxidase antibodies (TPOAb)
A 28-year-old patient with known Addison’s disease presents with abdominal pain and is hypotensive to a systolic pressure of 88 mmHg. He has a 2-week history of progressively worse nonproductive dry cough, sore throat, malaise, and headache. He has not checked his temperature at home but complains of constant chills. Which of the following is the best initial management?
Intravenous fluids
Azithromycin
Check serum glucose
X-ray of the chest
Hydrocortisone
A generally healthy 74-year-old woman who recently moved into the area visits the physician’s office for her first well-visit. She states that her previous doctor had been treating her with propylthiouracil (PTU) for subclinical hyperthyroidism, but that her prescription ran out several months ago. Laboratory studies reveal that her free thyroxine and triiodothyronine levels are normal, but her thyroid-stimulating hormone is depressed. PTU therapy is most important in this patient to prevent the development of which disorder?
Cardiac dysrhythmias
Hypothyroidism
Pretibial myxedema
Thyroid cancer
Thyroid storm
You recently evaluated a 28-year-old woman who presented with complaints of shakiness and heat intolerance. The patient plans to have children and is currently using no contraception. On examination you noted tachycardia with an HR of 102, a fine tremor, a diffuse goiter, and proptosis. You now have the laboratory results and note a TSH < 0.001, elevated total T4 of 17.8, and increased T3 uptake. Radionuclide uptake by the thyroid gland is elevated. You tell her that she has Graves’ disease. What is the best treatment plan for this patient?
Propylthiouracil
Radioactive iodine
Propranolol
Thyroid surgery
Oral corticosteroids
A 61-year-old obese man with a history of chronic alcohol abuse is diagnosed with type 2 DM. In addition to diet modification and exercise, his physician recommends he begin therapy with a hyperglycemic agent. Several days after starting therapy, his wife comes home from work and finds him sitting on the couch staring into space and breathing rapidly. When she speaks to him, she finds he is quite confused, and immediately takes him to the emergency department. Arterial blood gas analysis shows: pH: 7.2, HCO −: 19 mEq/L. Partial carbon dioxide pressure: 32 mmHg Partial oxygen pressure: 80 mmHg Lactate: 6 mmol/L. Which of the following drugs is most likely responsible for this patient’s symptoms?
Metformin
Acarbose
Glipizide
Insulin
Rosiglitazone
A 56-year-old woman presents to the outpatient clinic for a routine visit. On physical examination a 1-cm nodule is palpated in her thyroid. Her physical examination is otherwise unremarkable. Her heart rate is 70/min and regular, blood pressure is 126/82 mmHg, and temperature is 36.7°C (98.0°F). Which of the following is a poor prognostic indicator for the thyroid nodule?
Hoarseness
Female gender
Palpitations
Patient age of 56 years
Slow growth of nodule
A 55-year-old female presents to the office with a one-week history of left-sided ear pain and itchiness. The pain is especially bothersome at night, and is exacerbated by chewing. She denies any hearing loss. Her past medical history is significant for hypertension, type 2 diabetes mellitus, hyperlipidemia, and gout. Current medications include lisinopril, allopurinol, and metformin. She has missed her last two appointments with her primary care physician. Her temperature is 38.3°C (101°F), blood pressure is 140/90 mmHg, and pulse is 98/min. On examination, there is granulation tissue in the left ear canal with a scant amount of discharge. Which of the following is the best initial treatment for this patient?
Ciprofloxacin
Topical neomycin
Topical low-strength corticosteroids
Ampicillin/sulbactam
Surgical debridement
A 60-year-old man comes to your office complaining of difficulty hearing for the past few weeks. He has type 2 diabetes mellitus, which is well-controlled by diet alone. His past medical history is also significant for essential hypertension, congestive heart failure secondary to diastolic dysfunction, and chronic renal failure. Medications include aspirin, diuretics, an ACE inhibitor, and a beta-blocker. His pulse is 82/min, blood pressure is 140/90 mmHg, and respirations are 14/min. Examination reveals hearing loss in both ears. Which of the following medication is a potential cause of this patient's hearing problems?
Furosemide
Lisinopril
Aspirin
Metoprolol
Hydrochlorothiazide
A 7-year-old boy is brought to your office with a sore throat, decreased appetite, and nausea. His past medical history is insignificant. All of his vaccinations are up-to-date. He has no known allergies. His temperature is 39.0°C (102.5°F), blood pressure is 110/70 mmHg, pulse is 104/min, and respirations are 16/min. On examination, the pharynx and tonsils are red, swollen, and have white exudates on their surface. There is also bilateral tender cervical lymphadenopathy. The rapid diagnostic test for streptococcal antigen is positive. What is the most appropriate next step in management?
Oral penicillin V
Throat culture
Monospot test
Antistreptolysin O antibodies
Oral azithromycin
A 37-year-old woman presents to your office with severe vertigo, postural instability, and vomiting. She also complains of "a buzzing sound" in her right ear. She has had two similar episodes over the previous year that lasted several hours and resolved spontaneously. She has no other medical problems. Her mother died of breast cancer at 55 years of age and her father is currently suffering from colon cancer. Her heart rate is 90/min and blood pressure is 130/80 mmHg. Her BMI is 25.3 kg/m2. Examination reveals horizontal nystagmus. Which of the following could have prevented this patient's symptoms?
Low salt diet
Caloric restriction
Gluten-free diet
High complex carbohydrate diet
Calcium supplementation
A 30-year-old school teacher presents with a three-day history of fever, chills, and sore throat. He also complains of difficulty swallowing that started yesterday. He denies any cough, chest pain, or difficulty breathing. He is married and denies any new sexual encounters. His temperature is 39°C (102.2°F), blood pressure is 118/76 mmHg, pulse is 102/min, and respirations are 19/min. On examination, his voice is muffled. Enlarged, tender cervical lymph nodes are palpated on the left, and his uvula is deviated to the right. What is the most appropriate treatment for this patient?
Needle peritonsillar aspiration
Throat swabs and oral antibiotics
Monospot test and oral antibiotics
Emergency laryngoscopy
Cricothyroidotomy
A 73-year-old woman is transferred to the hospital from the nursing home because of diverticulitis. A prior CT scan showed inflamed sigmoid colon. Transferred records indicate a 2 day history of fever and abdominal pain. On admission, her white count is 22,000/cmm, and she is started on IV antibiotics and IV fluids. Over the ensuing few days, her white count starts to come down and she has no nausea, vomiting or fever; however, she suddenly develops a cough and increasing abdominal pain. Abdominal examination shows guarding and tenderness in the left lower quadrant. An upright x-ray film of the chest shows free air under the left diaphragm. Which of the following is the most appropriate next step in management?
Laparotomy
CT scan of the abdomen
Colonoscopy
Barium enema
Continue antibiotics and observe
A 35-year-old Hispanic male comes to the office because of excruciating pain during defecation for the past week. The pain is so severe that he avoids using the toilet. He also adds that he has noticed bright red blood in his stool. The caliber of his stool has not changed. His past medical history is significant for chronic constipation. Rectal examination shows a posterior mucosal tear of the anus. Which of the following is the most appropriate next step in management?
Local anesthetic and stool softeners
Colonoscopy
Lateral sphincterotomy
Antibiotics
Gradual dilatation of the sphincter
A 27-year-old man complains of episodic abdominal pain. The pain is concentrated in the epigastrium and is gnawing in quality. It wakes him up during the night and is promptly relieved by a glass of water and a piece of bread. He denies vomiting or diarrhea, but has experienced an occasional "dark stool." He has no significant past medical history and does not take any medications. His family history is significant for biliary disease in his mother and stomach cancer in his father. He smokes one pack of cigarettes a day and consumes a can of beer almost every day. His vital signs are with in normal limits. Physical examination shows mild epigastric discomfort on deep palpation. Which of the following is most likely to provide long-term symptom relief in this patient?
Antibiotics and pantoprazole
Four weeks of omepra zole
NSAIDs as needed
Smoking cessation
No alcohol consumption
A 55-year-old obese male presents to his physician for a routine annual physical examination. A review of systems is insignificant, except for constipation which has been present for several years. He does not have major medical problems and is not on any prescription or over-the-counter medications. He has smoked one and- a-half packs of cigarettes daily for 30 years. He drinks 4 oz of alcohol daily. Physical examination is unremarkable. As part of the routine screening, a colonoscopy is performed, which shows multiple diverticuli at the sigmoid colon. He is concerned about the diverticulosis. Which of the following is the most appropriate next step in the management of this patient's diverticulosis?
Increase dietary fiber intake
Advise him to stop smoking
Advise him to stop drinking alcohol
Explain his surgical options
Educate about prophylactic antibiotics
A 56-year-old woman with cirrhosis presents with a 2-week history of increasing abdominal distension. She has mild encephalopathy and esophageal varices without bleeding. Her cirrhosis is due to chronic hepatitis type B. She has a past history of ascites treated successfully with conservative management. She is currently on sodium, water and protein restriction, maximal doses of spironolactone and furosemide, and lactulose. Her temperature is 36.6°C (97.9°F), blood pressure is 120/70 mmHg, pulse is 80/min, and respirations are 30/min. She has a flapping tremor and labored breathing. Abdominal examination shows marked abdominal distension. An x-ray film of the chest is unremarkable. Abdominal ultrasound shows peritoneal fluid and splenomegaly, liver hyperechogenicity and nodularity, and portal vein width of 16 mm; no masses are evident. Which of the following is the most appropriate next step in the management of this patient's ascites?
Tapping of some amount of ascitic fluid
Intravenous furosemide therapy
Peritonea-jugular shunt
Distal spleno-renal shunt (selective shunt)
Side-to-side porto-caval shunt (non-selective shunt)
A 52-year-old woman with cirrhosis presents with increasing abdominal distension. Her treatment regimen was amended three days ago, when furosemide was added to spironolactone and sodium/water restriction. However, her distension persists, and today she is very somnolent and has passed very little urine. Her past medical history is remarkable for chronic hepatitis type B, cirrhosis, encephalopathy, and 2 bleeding episodes from esophageal varices; the bleeding was controlled with sclerotherapy. Her temperature is 36.5°C (97.6°F), blood pressure is 90/60 mm Hg, pulse is 80/min, and respirations are 18/min. Abdominal examination shows distension, shifting dullness, and no tenderness; bowel sounds are present. Laboratory studies show: Hemoglobin 11.0 g/L, Leukocyte count 3,500/mm3, Serum sodium 125 mEq/L, Serum potassium 5.5 mEq/L, Chloride 103 mEq/L, Blood urea nitrogen 60 mg/dL, Serum creatinine 1.8 mg/dL, Prothrombin time 18 sec, Partial thromboplastin time 35 sec. Urinalysis shows no abnormalities. Ultrasound of the kidney is unremarkable. Which of the following is the most appropriate next step in management?
Careful volume loading and discontinuation of furosemide and spironolactone
Increase the dose of furosemide to its maximum
Tapping of ascites
Renal biopsy
Intravenous pyelography
A 34-year-old Caucasian male presents to the office with a 4-week history of diarrhea. He just returned from a trip to South America, where he developed foul-smelling stools, abdominal cramps and bloating. A three-day course of ciprofloxacin did not relieve his symptoms. His vital signs are within normal limits. Physical examination shows no abnormalities. Which of the following is the most appropriate next step in management?
Prescribe oral metronidazole
Schedule colonoscopy
Obtain CT scan of the abdomen
Prescribe another course of ciprofloxacin
Prescribe oral ampicillin
A 65-year-old male complains of fatigue for the past one month. He has been living alone since the death of his wife one year ago. He does not like to cook, and his diet consists mostly of canned food, hot tea, and toast. He drinks one glass of white wine nightly with dinner. Examination shows pallor of the skin, nail beds and conjunctiva. Rectal exam is heme-negative. His physical examination is otherwise unremarkable. Administration of which of the following would be most helpful in treating his condition?
Folic acid
Vitamin B12
Vitamin C
Vitamin D
Vitamin E
A 33-year-old male is admitted to the hospital after an episode of tonic-clonic seizures. He is a known IV drug abuser. He admits 'shooting' cocaine and heroin prior to the seizure. He has never had seizures before. Fallowing the seizure, he complains of muscle pain but otherwise feels normal. His temperature is 37.2°C (98.9°F) and his blood pressure is 156/90 mm Hg. Laboratory analyses reveal the following: CPK 11,200 U/ml, AST 545 U/L, ALT 560U/L, Troponin T normal, Anti-HAV antibodies negative, HBsAg negative, Anti-HBsAg negative, Anti-HCV antibodies positive. He reports that a recent HIV test was negative. Which of the following is the best management for this patient?
Hepatitis B vaccination
Fluid restriction
Metoprolol
Life-long phenytoin therapy
No intervention
A 40-year-old man with a recent history of exploratory laparotomy for a stabbing injury presents to the emergency department with diffuse cramping abdominal pain for 1 day, accompanied by nausea, multiple episodes of brown colored vomitus, and lack of stool, but he reports some flatulence. He denies any fever. On physical examination, the patient has stable vital signs, and there is diffuse distention in the abdomen with guarding and tenderness but no rebound, as well as high-pitched bowel sounds. Rectal examination reveals no fecal impaction in the rectal vault, and the stool was guaiac- negative. Complete blood cell count reveals no significant abnormalities and serum chemistry shows a mild metabolic alkalosis. CT demonstrates a noticeable difference in the diameter of proximal and distal small bowel. Which of the following is the most appropriate management?
Give the patient nothing by mouth, insert a nasogastric tube, and perform intravenous correction of electrolyte abnormalities
Broad-spectrum antibiotics
Colonoscopy
Exploratory laparotomy with lysis of adhesions
Serial abdominal examinations
A 52-year-old woman is experiencing abdominal discomfort after meals as well as early in the morning. There is no weight loss or constitutional symptoms, and she has tried antacids but experienced minimal relief. Upper endoscopy reveals a duodenal ulcer and the biopsy is negative for malignancy. Which of the following is the most appropriate next step in management?
Antibiotic therapy with omeprazole
6–8 weeks of omeprazole or ranitidine
Long-term acid suppression with omeprazole
Antibiotic therapy
Bismuth citrate therapy
A 36-year-old man presents for a well-patient examination. He gives a history that, over the past 20 years, he has had three episodes of abdominal pain and hematemesis, the most recent of which occurred several years ago. He was told that an ulcer was seen on a barium upper GI radiograph. You obtain a serum assay for H pylori IgG, which is positive. What is the most effective regimen to eradicate this organism?
Omeprazole 20 mg twice daily, amoxicillin 1000 mg twice daily, and clarithromycin 500 mg twice daily for 14 days
Omeprazole 20 mg orally once daily for 6 weeks
Ranitidine 300 mg orally once daily at bedtime for 6 weeks
Pepto-Bismol and metronidazole twice daily for 7 days
Benzathine penicillin, 1.2 million units intramuscularly weekly for three doses
An otherwise healthy 40-year-old woman sees you because of recurrent abdominal pain. In the past month she has had four episodes of colicky epigastric pain. Each of these episodes has lasted about 30 minutes and has occurred within an hour of eating. Two of the episodes have been associated with sweating and vomiting. None of the episodes have been associated with fever or shortness of breath. She has not lost weight. She does not drink alcohol or take any prescription or over-the-counter medications. Other than three previous uneventful vaginal deliveries, she has never been hospitalized. Her examination is negative except for mild obesity (BMI = 32). A complete blood count and multichannel chemistry profile that includes liver function test is normal. A gallbladder sonogram reveals multiple gallstones. What is the next best step in the treatment of this patient?
Laparoscopic cholecystectomy
Omeprazole, 20 mg daily for eight weeks
Ursodeoxycholic acid
Observation without specific therapy
Weight reduction
A 56-year-old chronic alcoholic has a 1-year history of ascites. He is admitted with a 2-day history of diffuse abdominal pain and fever. Examination reveals scleral icterus, spider angiomas, a distended abdomen with shifting dullness, and diffuse abdominal tenderness. Paracentesis reveals slightly cloudy ascitic fluid with an ascitic fluid PMN cell count of 1000/μL. Which of the following statements about treatment is true?
The addition of albumin to antibiotic therapy improves survival
Antibiotic therapy is unnecessary if the ascitic fluid culture is negative for bacteria
Repeated paracenteses are required to assess the response to antibiotic treatment
After treatment of this acute episode, a recurrent episode of spontaneous bacterial peritonitis would be unlikely
Treatment with multiple antibiotics is required because polymicrobial infection is common
A 60-year-old man with known hepatitis C and a previous liver biopsy showing cirrhosis requests evaluation for possible liver transplantation. He has never received treatment for hepatitis C. Though previously a heavy user of alcohol, he has been abstinent for over 2 years. He has had 2 episodes of bleeding esophageal varices. He was hospitalized 6 months ago with acute hepatic encephalopathy. He has a 1 year history of ascites that has required repeated paracentesis despite treatment with diuretics. Medications are aldactone 100 mg daily and lactulose 30 cc 3 times daily. On examination he appears thin, with obvious scleral icterus, spider angiomas, palmar erythema, gynecomastia, a large amount ascites, and small testicles. There is no asterixis. Recent laboratory testing revealed the following: hemoglobin = 12.0 mg/dL (normal 13.5-15.0), MCV = 103 fL (normal 80-100), creatinine = 2.0 mg/dL (normal 0.7-1.2), bilirubin = 6.5 mg/dL (normal 0.1-1.2), AST = 25 U/L (normal < 40), ALT= 45 U/L (normal < 40), INR = 3.0 (normal 0.8-1.2). What is the next best step?
Refer the patient to a liver transplantation center
Repeat liver biopsy
Start treatment with interferon and ribavirin
Refer the patient for hospice care
Continue to optimize medical treatment for his ascites and hepatic encephalopathy and tell the patient he is not eligible for liver transplantation because of his previous history of alcohol abuse
A 32-year-old white woman complains of abdominal pain off and on since the age of 17. She notices abdominal bloating relieved by defecation as well as alternating diarrhea and constipation. She has no weight loss, GI bleeding, or nocturnal diarrhea. On examination, she has slight LLQ tenderness and gaseous abdominal distension. Laboratory studies, including CBC, are normal. Which of the following is the most appropriate initial approach?
Recommend increased dietary fiber, antispasmodics as needed, and follow-up examination in 2 months
Refer to gastroenterologist for colonoscopy
Obtain antiendomysial antibodies
Order UGI series with small bowel follow-through
Order small bowel biopsy
A 27-year-old female is found to have a positive hepatitis C antibody at the time of plasma donation. Physical examination is normal. Liver enzymes reveal ALT of 62 U/L (normal < 40), AST 65 U/L (normal < 40), bilirubin 1.2 mg/dL (normal), and alkaline phosphatase normal. Hepatitis C viral RNA is 100,000copies/mL. Hepatitis B surface antigen and HIV antibody are negative. Which of the following statements is true?
Patients with hepatitis C genotype 2 or 3 are more likely to have a favourable response to treatment with interferon and ribavirin
Liver biopsy is necessary to confirm the diagnosis of hepatitis C
Most patients with hepatitis C eventually resolve their infection without permanent sequelae
This patient should not receive vaccinations against other viral forms of hepatitis
Serum ALT levels are a good predictor of prognosis
A 45-year-old woman presents to the ED with 1 day of painful rectal bleeding. Review of systems is negative for weight loss, abdominal pain, nausea, and vomiting. On physical examination, you note an exquisitely tender swelling with engorgement and a bluish discoloration distal to the anal verge. Her vital signs are HR 105 beats per minute, BP 140/70 mm Hg, RR 18 breaths per minute, and temperature 99°F. Which of the following is the next best step in management?
Excision under local anesthesia followed by sitz baths and analgesics
Recommend warm sitz baths, topical analgesics, stool softeners, a high-fiber diet, and arrange for surgical follow-up
Incision and drainage under local anesthesia or procedural sedation followed by packing and surgical follow-up
Obtain a complete blood cell (CBC) count, clotting studies, type and cross, and arrange for emergent colonoscopy
Surgical consult for immediate operative management
A 65-year-old man with a history of occasional painless rectal bleeding presents with 2 to 3 days of constant, dull RLQ pain. He also complains of fever, nausea, and decreased appetite. He had a colonoscopy 2 years ago that was significant for sigmoid and cecal diverticula but was otherwise normal. On physical examination he has RLQ tenderness with rebound and guarding. His vitals include HR of 95 beats per minute, BP of 130/85 mm Hg, and temperature of 101.3°F. The abdominal CT demonstrates the presence of sigmoid and cecal diverticula, inflammation of pericolic fat, thickening of the bowel wall, and a fluid-filled appendix. Which of the following is the most appropriate next step in management?
Begin IV hydration and broad-spectrum antibiotics, keep the patient npo (nothing by mouth), and admit the patient to the hospital
Discharge the patient with broad-spectrum oral antibiotics and surgical follow-up
Begin IV antibiotics and call a surgical consult for an emergent operative procedure
Arrange for an emergent barium enema to confirm the diagnosis
Begin sulfasalazine 3 to 4 g/d along with IV steroid therapy
A 49-year-old man presents to the ED with nausea, vomiting, and abdominal pain that began approximately 2 days ago. The patient states that he usually drinks a six pack of beer daily, but increased his drinking to 2 six packs daily over the last week because of pressures at work. He notes decreased appetite over the last 3 days and states he has not had anything to eat in 2 days. His BP is 125/75 mm Hg, HR is 105 beats per minute, and RR is 20 breaths per minute. You note generalized abdominal tenderness on examination. Laboratory results reveal the following: White blood cells (WBC) 9000/μL Sodium 131 mEq/L Hematocrit 48% Potassium 3.5 mEq/L Platelets 210/μL Chloride 101 mEq/L Aspartate transaminase (AST) 85 U/L Bicarbonate 10 mEq/L Alanine transaminase (ALT) 60 U/L Blood urea nitrogen (BUN) 9 mg/dL Alkaline phosphatase 75 U/L Creatinine 0.5 mg/dL Total bilirubin 0.5 mg/dL Glucose 190 mg/dL Lipase 40 IU Nitroprusside test weakly positive for ketones Which of the following is the mainstay of therapy for patients with thiscondition?
Solution containing both saline and glucose (D 5/NS or D 5 NS)
Normal saline (NS) solution
Half normal saline (NS)
Glucose solution (D5W)
The type of solution is irrelevant
A 31-year-old man from Florida presents to the ED complaining of severe pain that starts in his left flank and radiates to his testicle. The pain lasts for about 1 hour and then improves. He had similar pain last week that resolved spontaneously. He noted some blood in his urine this morning. His BP is 145/75 mm Hg, HR is 90 beats per minute, temperature is 98.9°F, and his RR is 24 breaths per minute. His abdomen is soft and nontender. As you examine the patient, he vomits and has trouble lying still in his stretcher. Which of the following is the most appropriate next step in management?
Start intravenous (IV) fluids and administer an IV nonsteroidal anti-inflammatory drug (NSAID) and antiemetic
Call surgery consult to evaluate the patient for appendicitis
Order an abdominal CT
Perform an ultrasound to evaluate for an abdominal aortic aneurysm (AAA)
Perform an ultrasound to evaluate for testicular torsion
A 22-year-old man presents to the ED complaining of dysuria for 3 days. He states that he has never had this feeling before. He is currently sexually active and uses a condom most of the time. He denies hematuria but notes a yellowish discharge from his urethra. His BP is 120/75 mm Hg, HR is 60 beats per minute, and temperature is 98.9°F. You send a clean catch urinalysis to the laboratory that returns positive for leukocyte esterase and 15 white blood cells per high power field (WBCs/hpf). Which of the following is the most appropriate next step in management?
Send a urethral swab for culture and administer 125 mg ceftriaxone intramuscularly and 1 g azithromycin orally
Send urine for culture and administer SMX/TMP orally
Discharge the patient with strict instructions to return if his symptoms worsen
Order a CT scan to evaluate for a kidney stone
Have him follow-up immediately with a urologist to evaluate for testicular cancer
An 18-year-old woman presents to the ED complaining of acute onset of RLQ abdominal pain. She also describes the loss of appetite over the last 12 hours, but denies nausea and vomiting. Her BP is 124/77 mm Hg, HR is 110 beats per minute, temperature is 102.1°F, RR is 16 breaths per minute, and oxygen saturation is 100% on room air. Abdominal examination reveals lower abdominal tenderness bilaterally. On pelvic examination you elicit cervical motion tenderness and note cervical exudates. Her WBC is 20,500/μL and β-hCG is negative. Which of the following is the most appropriate next step in management?
Begin antibiotic therapy
Bring her to the OR for an appendectomy
Perform a culdocentesis
Bring her to the OR for immediate laparoscopy
Order an abdominal plain film
A 30-year-old man presents to the ED complaining of sudden onset of abdominal bloating and back pain lasting for 2 days. The pain woke him up from sleep 2 nights ago. It radiates from his back to his abdomen and down toward his scrotum. He is in severe pain and is vomiting. His temperature is 101.2°F and HR is 107 beats per minute. A CT scan reveals a 9-mm obstructing stone of the left ureter with hydronephrosis. Urinalysis is positive for 2+ blood, 2+ leukocytes, 2+ nitrites, 40 to 50 WBCs, and many bacteria. You administer pain medicine, antiemetics, and antibiotics. Which of the following is the most appropriate next step in management?
Admit for IV antibiotics and possible surgical removal of stone
Observe in ED for another 6 hours to see if stone passes
Discharge with antibiotics and pain medicine
Discharge patient with instructions to consume large amounts of water
Discharge patient with antibiotics, pain medicine, and instructions to drink large amounts of water and cranberry juice
A 24-year-old woman presents to the ED after being sexually assaulted. She is a college student with no past medical history. Her BP is 130/75 mm Hg, HR is 91 beats per minute, temperature is 98.6°F, and RR is 16 breaths per minute. On physical examination you observe vaginal trauma and scattered bruising and abrasions. Which of the following medications should be offered to the patient in this scenario?
Ceftriaxone, azithromycin, tetanus, metronidazole, antiretrovirals, emergency contraception
Ceftriaxone, azithromycin, metronidazole, antiretrovirals, emergency contraception
Ceftriaxone, tetanus, metronidazole, antiretrovirals, emergency contraception
Ceftriaxone, azithromycin, tetanus, metronidazole, emergency contraception
Ceftriaxone, azithromycin, tetanus, antiretrovirals, emergency contraception
A 43-year-old man presents to the ED complaining of progressively worsening abdominal pain over the past 2 days. The pain is constant and radiates to his back. He also describes nausea and vomiting and states he usually drinks six pack of beer daily, but has not had a drink for 2 days. His BP is 144/75 mm Hg, HR is 101 beats per minute, temperature is 99.8°F, and RR is 14 breaths per minute. He is lying on his side with his knees flexed. Examination shows voluntary guarding and tenderness to palpation of his epigastrium. Laboratory results reveal WBC 10,500/μL, hematocrit 51%, platelets 225/μL, and lipase 620 IU. An abdominal radiograph reveals a nonspecific bowel gas pattern. There is no free air under the diaphragm. Which of the following is the most appropriate next step in management?
Admit to the hospital for medical management and supportive care
Observe in the ED
Send home with antibiotic therapy
Admit to the hospital for endoscopy
Admit to the hospital for exploratory laparotomy
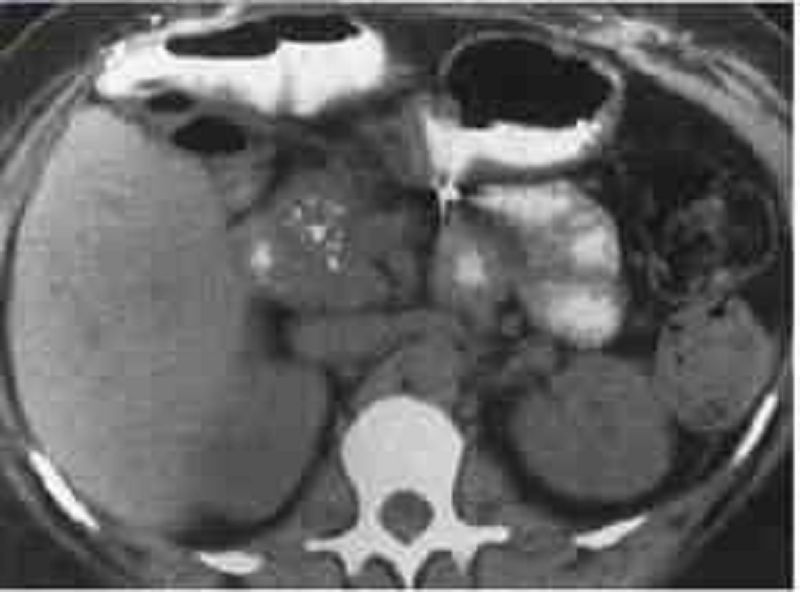
A 76-year-old man who has had multiple episodes of pancreatitis presents to his physician’s office with mild epigastric pain and 9.1-kg (20.0-lb) weight loss over the past 6 months. The patient also describes daily foul-smelling stools that “float” in the toilet bowl. The physician pulls up his electronic medical record and finds that the patient presented to the emergency department last week for the same symptoms. During that visit he had a CT of the abdomen (see image). Which of the following is the most appropriate treatment?
Pancreatic enzyme replacement
Endoscopic retrograde cholangiopancreatography
Pancreaticogastrostomy
Surgical resection of pancreas
Whipple procedure
A 34-year-old man presents with substernal discomfort. The symptoms are worse after meals, particularly a heavy evening meal, and are sometimes associated with hot/sour fluid in the back of the throat and nocturnal awakening. The patient denies difficulty swallowing, pain on swallowing, or weight loss. The symptoms have been present for 6 weeks; the patient has gained 20 lb in the past 2 years. Which of the following is the most appropriate initial approach?
Therapeutic trial of ranitidine
Exercise test with thallium imaging
Esophagogastroduodenoscopy
CT scan of the chest
Coronary angiography
A 48-year-old man with a past medical history of hepatitis C and cirrhosis presents to the ED complaining of acute-onset abdominal pain and chills. His BP is 118/75 mm Hg, HR is 105 beats per minute, RR is 16 breaths per minute, temperature is 101.2°F rectally, and oxygen saturation is 97% on room air. His abdomen is distended, and diffusely tender. You decide to perform a paracentesis and retrieve 1 L of cloudy fluid. Laboratory analysis of the fluid shows a neutrophil count of 550 cells/mm 3. Which of the following is the most appropriate choice of treatment?
Cefotaxime
Metronidazole
Vancomycin
Sulfamethoxazole/trimethoprim (SMX/TMP)
Neomycin and lactulose
A 29-year-old woman complains of dysphagia with both solids and liquids, worse when she is eating quickly or is anxious. Manometry reveals normal basal esophageal sphincter pressure, with no relaxation of the sphincter on swallowing. Which of the following is the most appropriate next step in management?
Calcium channel blockers
Beta-blocker therapy
Partial esophagectomy
Anticholinergic drugs
Dietary modification
A 39-year-old Japanese-American woman with insulin-dependent diabetes and asthma presents to her primary care physician complaining of trouble swallowing for the past few months. She explains that it started with solids, and then progressed to liquids. She states it now is hard even to swallow water and that she is often very thirsty. She says she has lost about 3.2 kg (7 lb), but says she is working out frequently. Her blood pressure is 118/76 mm Hg, pulse is 86/min, respiratory rate is 16/min, and temperature is 37.2°C (98.9°F). Laboratory tests show: Na+: 144 mEq/L, K+: 4.0 mEq/L, Cl−: 100 mEq/L, Carbon dioxide: 22 mmol/L Blood urea nitrogen: 18 mg/dL Creatinine: 1.0 mg/dL, Glucose: 88 mg/dL. Her hemoglobin A1c level, measured 3 months earlier, was 6.1%. A barium swallow is performed, which reveals a dilated esophagus, especially distally, that flares out near the lower esophageal junction. Still not completely sure of the diagnosis, esophageal manometry is performed, which reveals abnormal peristalsis and increased lower sphincter pressure. Which of the following is the most appropriate management?
Pneumatic dilation
Cholinergic agents
Glucose pharmacotherapy
Instructions to elevate the bed, avoid fatty foods, and consider a histamine blocker
Surgery to remove diverticula
A 55-year-old man is brought to the ED by his family. They state that he has been vomiting large amounts of bright red blood. The patient is an alcoholic with cirrhotic liver disease and a history of portal hypertension and esophageal varices. His vitals on arrival are HR 110 beats per minute, BP 80/55 mm Hg, RR 22 breaths per minute, and temperature 99°F. The patient appears pale and is in moderate distress. Which of the following is an inappropriate option in the initial management of a hypotensive patient with a history of known esophageal varices presenting with hematemesis?
Sengstaken-Blakemore tube placement
Two large-bore IV lines and volume repletion with crystalloid solutions
Nasogastric (NG) lavage
IV octreotide
Gastrointestinal (GI) consult
A 59-year-old woman presents to the ED complaining of worsening lower abdominal pain over the previous 3 days. She describes feeling constipated recently and some burning when she urinates. Her BP is 135/75 mm Hg, HR is 89 beats per minute, temperature is 101.2°F, and her RR is 18 breaths per minute. Her abdomen is mildly distended, tender in the LLQ, and positive for rebound tenderness. CT scan is consistent with diverticulitis with a 7-cm abscess. Which of the following is the most appropriate management for this condition?
Start treatment with ciprofloxacin and metronidazole and plan for CT-guided draining of the abscess
Reserve the OR for emergent laparotomy
Give an IV dose of ciprofloxacin and have the patient follow up with her primary physician
Start treatment with ciprofloxacin and metronidazole and plan for an emergent barium enema
Start treatment with ciprofloxacin and metronidazole and prepare for an emergent colonoscopy
A 60-year-old man is brought to the ED complaining of generalized crampy abdominal pain that occurs in waves. He has been vomiting intermittently over the last 6 hours. His BP is 150/75 mm Hg, HR is 90 beats per minute, temperature is 99.8°F, and his RR is 16 breaths per minute. On abdominal examination you notice an old midline scar across the length of his abdomen that he states was from surgery after a gunshot wound as a teenager. The abdomen is distended with hyperactive bowel sounds and mild tenderness without rebound. An abdominal plain film confirms your diagnosis. Which of the following is the most appropriate next step in management?
Begin fluid resuscitation, bowel decompression with a nasogastric tube, and request a surgical consult
Begin fluid resuscitation, administer broad-spectrum antibiotics, and admit the patient to the medical service
Begin fluid resuscitation, give the patient stool softener, and administer a rectal enema
Begin fluid resuscitation, administer broad-spectrum antibiotics, and observe the patient for 24 hours
Order an abdominal ultrasound, administer antiemetics, and provide pain relief
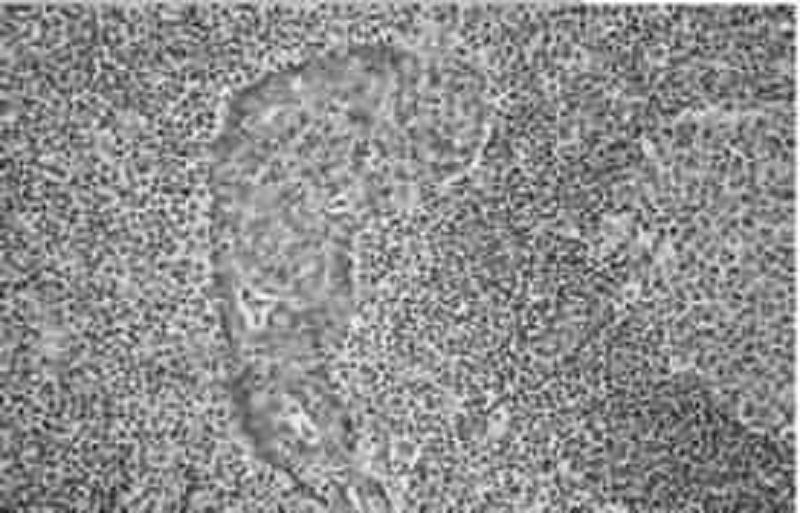
A 54-year-old man presents to his primary care provider with the complaint of upper abdominal fullness and pain. He states that he has lost 2.3-4.6 kg (5-10 lb), but denies other symptoms. Physical examination reveals a firm mass in the epigastric area. Ultrasonography reveals a mass in the gastric antrum. A salivary gland biopsy reveals the pathology shown in the image. Which of the following therapies is expected to be part of his treatment plan?
Antibiotic therapy
Bone marrow transplantation
Gene therapy
Liver transplantation
Multiagent chemotherapy
A 68-year-old African-American man presents to his primary care physician for a check-up. He has not been to the physician’s office in over 15 years. He reports that he is fine but that his wife keeps telling him that he has to “go see the doctor.” He says he has never been sick, despite smoking three packs of cigarettes per day for over 40 years. He also says that he drinks 2–3 beers a night but never had a problem with that either. He’s as healthy “as a bull,” he says. His wife is in the room and says that he recently has had some problems swallowing food and that he is losing weight. He laughs and says, “I just need to chew more and eat more.” His vital signs are normal, as are his laboratory values. The physician is concerned and orders an endoscopy, which reveals a biopsy positive for squamous cell carcinoma of the esophagus. Which of the following most likely could have prevented this condition?
Eliminating smoking and alcohol consumption
Avoiding fruits and vegetables
Eating more meats, especially smoked meats
Getting a colonoscopy every 5 years
Taking proton pump inhibitors regularly
A full-term 6-day-old boy presents to a physician’s office for routine care. He is tolerating breast milk well. He is urinating, defecating, and sleeping normally. Physical examination reveals an alert new-born with mild eczema, good skin turgor, normal reflexes, and a musty odor. His newborn laboratory screen is notable for phenylketones in the urine. What is the best advice to give his parents regarding the boy’s diet?
Increase tyrosine
Increase iron
Increase niacin
Increase phenylalanine
Increase vitamin D
A 34-year-old woman complains bitterly of heartburn. Physical examination reveals healing lesions of the fingertips that she says were small ulcers, and there are small areas of telangiectasias on her face. Esophageal manometry reveals a decrease in the expected amplitude of smooth muscle contraction. Lower esophageal sphincter tone is subnormal, but relaxes normally with swallowing. Which of the following statements regarding this condition is most likely correct?
Predominantly treated symptomatically
Characterized by systemic signs of inflammation
Characterized by a poor prognosis
Usually more frequent in men
Characterized by death secondary to a renal crisis
A 61-year-old man in previously excellent health presents to his physician with com- plaints of hematochezia tenesmus, and rectal pain. On work-up the physician discovers that he has a rectal tumor that is 5 cm (2.0 in) from the anal verge. Which of the following is the most appropriate treatment?
Abdominoperineal resection
Imatinib
Low anterior resection
Radiation alone
Radiation plus chemotherapy
{"name":"New Part 4 (765-865) (765-1019) NR 7", "url":"https://www.quiz-maker.com/QPREVIEW","txt":"Test your medical knowledge with our in-depth quiz featuring 59 thoughtfully crafted questions. Designed for healthcare professionals and students alike, this quiz covers a broad spectrum of medical topics including diabetes management, endocrinology, and patient care.Challenge yourself and see how well you understand important medical concepts. Enhance your learning experience by:Exploring diverse medical scenariosImproving your clinical reasoning skillsPreparing for exams or certifications","img":"https:/images/course5.png"}