Picture USMLE
A 43-year-old man presents to your office complaint of nagging left-side chest pain that increases on deep inspiration, plus two weeks of non-productive cough. He denies chills, fever or weight loss. His medical history is significant for Hodgkin's disease treated 20 years ago with chemotherapy and radiation therapy. On physical examination today, his blood pressure is 140/90 mmHg and his heart rate is 90/min.His chest x-ray is shown below.
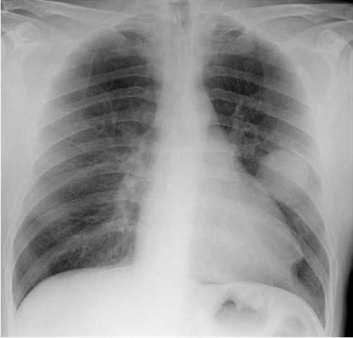
Which of the following is the most likely cause of his chest pain?
Radiation-induced fibrosis
Fungal pneumonia
Recurrence of Hodgkin's disease
Pulmonary tuberculosis
Secondary malignancy
A 56-year-old woman is brought to the hospital from a local restaurant after suddenly becoming short of breath. Her flow-volume loop is shown below.

Which of the following is the most likely cause of her symptoms?
Asthma attack
Pneumothorax
Pulmonary edema
Laryngeal edema
Panic attack
A 54-year-old black male from the southeast USA presents to you with complaints of generalized malaise, fever, and a cough. He claims that he has had intermittent hemoptysis for the past six months. He denies smoking and has never had tuberculosis. Examination is unremarkable and his chest x-ray is shown below.

On changing position, you notice that the part of the lesion seen on x-ray also moves. The most likely diagnosis is?
Lung abscess
Histoplasmosis
Pulmonary embolism
Bronchiectasis
Aspergilloma
A 65-year-old white male who has a history of chronic obstructive pulmonary disease, congestive heart failure, and coronary artery disease presented with a three-day history of worsening shortness of breath, cough with yellowish expectoration, and fever. He is not on steroids and does not use oxygen at home. He takes ipratropium, albuterol, aspirin, digoxin, furosemide, metoprolol, and lisinopril. He lives at home with his wife. His temperature is 39.4C (103F), blood pressure is 110/70 mmHg, pulse is 110/min, and respirations are 24/min. He is saturating 88% on room air. He was started on 3-liters of oxygen to keep the saturations above 92%. The chest x-ray of the patient is shown below.

What is the most appropriate next step in the management of this patient?
Admit the patient and give ampicillin
Admit the patient and start ciprofloxacin
Outpatient trimethoprim-sulfamethoxazole
Admit the patient and start vancomycin
Admit the patient and start levofloxacin
A 48-year-old male presents to the doctor with a history of persistent cough, tenacious mucopurulent sputum, and intermittent chills. He has been treated with several courses of antibiotics without resolution of his symptoms. On examination, he has an emaciated appearance and there is decreased air entry in the right lung base. His sputum has a foul smell. High resolution CT scan of the chest is shown below:

Which of the following is the most feared complication of this patient's condition?
Pneumonia
Respiratory failure
Hemoptysis
Pulmonary embolism
Pneumothorax
A 64-year-old African American male presents to you with complaints of a dry cough, weight loss and pain in his right arm. The symptoms started approximately 2 months ago. His past medical history is significant for type 2 diabetes mellitus and hypertension. He smokes 1 pack per day and drinks alcohol occasionally. He denies any drug allergies. Physical examination is unremarkable. ECG reveals normal sinus rhythm. An MRI of his chest is shown below.

Which of the following is most likely responsible for this patient's symptoms?
Aspergilloma
Cryptogenic organizing pneumonia
Bronchial carcinoid
Lung abscess
Superior sulcus tumor
A 61-year-old man is being evaluated for progressive exertional dyspnea and decreased exercise tolerance. He has also noticed some ankle swelling. The patient has a 40 pack-year smoking history but denies illicit drug use or occupational exposures. His chest x-ray is shown below.

The abnormal diaphragmatic contour seen here most likely results in which of the following?
Higher inspiratory flow
Increased thoracic wall recoil
Reduced expiratory effort
Decreased lung compliance
Increased work of breathing
A 65-year-old male comes to the emergency department with severe shortness of breath. The symptoms started one week ago with fever and a non-productive cough. His past medical history is significant for coronary artery disease with bypass surgery two years ago, hypertension and diabetes mellitus. His temperature is 38.9C (102 F), blood pressure is 160/70 mm Hg, pulse is 110/min, and respirations are 26/min. Physical examination reveals decreased breath sounds over the right lower lung base. His chest X-ray is shown on the slide below:

Which of the following is the most likely cause of this patient's current complaints?
Bronchopleural fistula
Pneumothorax
Lung abscess
Pulmonary infarction
Empyema
A 35-year-old man who recently emigrated from Mexico complains of persistent cough. He says that he coughs up yellowish sputum that is occasionally streaked with blood. He also notes occasional fevers and frequent nighttime awakenings with cough and choking. He has a 20 pack-year smoking history but does not use alcohol or drugs. CT of his chest is shown below. What is the most likely diagnosis?

Bronchiectasis
Bronchopulmonary aspergillosis
Pulmonary tuberculosis
Sarcoidosis
Lung cancer
A 67-year-old white male with a long history of bronchial asthma and chronic obstructive pulmonary disease (COPD) presents to the emergency room complaining of acute onset of shortness of breath for the last 30 minutes. He says that for the past 2 or 3 days he has been having some difficulty breathing and a productive cough with thick phlegm, but nothing as bad as the current episode. He also has a history of congestive heart failure after suffering a myocardial infarction for which he is taking furosemide and lisinopril. While talking to you in halting sentences, you note that he appears cyanotic, confused and are sweating profusely. He normally takes albuterol, ipratropium and budesonide inhalers for his breathing difficulties, but they have not relieved his current symptoms. On examination, he is found to be markedly dyspneic and his PaO2 is 55 mm Hg. A chest x-ray done in the ER is shown below.

Which of the following is the most appropriate next step in the management of this patient?
Start intravenous theophylline
Place central venous line
Urgent thoracocentesis
Increase furosemide and start digoxin
Urgent bronchoscopy
A 69-year -old Caucasian man presents with a two-day history of increasing shortness of breath and lower extremity edema. He is currently short of breath at rest and has an occasional cough. There is no past history of hypertension or ischemic heart disease. He reports drinking half a bottle of vodka daily and has smoked 1 pack of cigarettes per day for 45 years. His blood pressure is 160/90 mm Hg, pulse is 90/min, and oxygen saturation is 90% on room air. JVP is elevated and auscultation of his heart reveals faint heart sounds. The liver span is 18 cm and ascites is also present. No rales are heard in the lungs. There is 3+ lower extremity pitting edema up to the knees. The chest radiograph is shown below. Which of the following is the most likely diagnosis?

Alcoholic cirrhosis
Metastatic carcinoma of the liver
Coronary artery disease
Cor pulmonale
Cardiac tamponade
A 64-year-old male is admitted to the hospital with abdominal pain, abdominal distention, and confusion. Upon arrival his blood pressure is 90/60 mmHg and pulse is 120/min. On physical examination, his abdomen is tender, distended, and rigid with positive rebound tenderness. His past medical history is significant for rheumatic fever as a child, hypertension, coronary artery disease and atrial fibrillation. He receives a total of 6 liters of normal saline and undergoes emergent laparotomy. Postoperatively he complains of shortness of breath. His respiratory rate is 34/min. He is emergently intubated because of poor oxygenation. His chest x-ray is shown below:

This film is compared to a chest x-ray performed one week earlier, which was within normal limits. Currently, the pulmonary capillary wedge pressure is 8 mmHg. Which of the following is the most likely cause of his current condition?
Idiopathic pulmonary fibrosis
Left ventricular systolic dysfunction
Mitral stenosis
Iatrogenic fluid overload
Acute respiratory distress syndrome
A 45-year-old black female presents to you because of a dry cough and has not been feeling well for the past month. She did have some pain in her shins a few weeks ago. She denies any allergies, smoking, or other medical problems. Her ECG shows normal sinus rhythm. The chest x-ray is shown below.

What is the most likely pathophysiology in this patient?
Pulmonary venous congestion
Malignancy of the lung
Lupus pneumonitis
Interstitial lung disease
Inflammatory granulomas
A 38-year -old male is brought to the emergency room with high-grade fever, shaking chills, productive cough and shortness of breath that started two days ago. His medical history is significant for two hospital admissions for alcohol withdrawal seizures. He continues to drink alcohol every day. He has no other medical problems and does not take any medications. On admission, his temperature is 39.7°C (103.5.F), pulse is 110/min, blood pressure is 100/70 mmHg, and respirations are 20/min. His skin and mucous membranes are dry. Physical examination reveals crackles and bronchial breath sounds in the right lower lobe. Chest x-ray demonstrates right lower lobe consolidation. He is started on ceftriaxone, azithromycin and intravenous normal saline at 200 ml/hr. Six hours later the nurse calls you because he is breathing at 38/min and requiring 100% oxygen. Emergent intubation is performed. A repeat chest x-ray is shown below.

Which of the following is now most likely to be present in this patient?
Normal pulmonary capillary wedge pressure
Normal pulmonary arterial pressure
Increased lung compliance
Normal alveolar-arterial oxygen gradient
Increased left ventricular end diastolic pressure
A 32-year-old man is intubated and mechanically ventilated after an opioid drug overdose. The ventilator triggers 12 breaths per minute, each delivering 500 ml of tidal volume at a flow rate of 60 L/min. You perform an inspiratory hold for 2 seconds following delivery of the tidal volume, and the airway pressure is measured to be 30 cm H2O:

The measured pressure reflects which of the following?
Upper airway resistance
Expiratory muscle strength
Total airway resistance
End-expiratory pressure
Pulmonary compliance
A 35-year-old male from Arizona presents to the physician's office with a low-grade fever and cough of two months duration. He also reports malaise and a weight loss of 71bs over this same period. He has a history of HIV infection diagnosed two years ago. He received a pneumococcal vaccine at the time his HIV was diagnosed. He also receives an annual influenza vaccine. He is not on any antiretroviral therapy. His temperature is 37.7C (99.8F), pulse is 75/min, blood pressure is 130/80 mm Hg and respirations are 14/min. Examination shows clear lungs to auscultation. His current CD4 count is 450cells/microl. His chest radiograph is shown below:

Which of the following is the most likely cause of his cough?
Bronchial asthma
Postnasal drip
Gastroesophageal reflux disease
Coccidioidomycosis
Mycobacterial infection
A 65-year-old female presents with 6 months of worsening dyspnea and dry cough. Whereas she had previously enjoyed an active lifestyle, she now becomes breathless after walking just a few steps. The patient denies fever or chest pain and does not use tobacco, alcohol or illicit drugs. Her only medicine is hydrochlorothiazide for hypertension. She is retired and lives with her husband. She has never travelled abroad and denies any history of exposure to pets. On physical examination, her temperature is 37.2°C (98.9.F), blood pressure is 140/86 mm Hg, pulse is 84/min and respirations are 18/min. Examination shows dry, late inspiratory crackles and finger clubbing. Her chest x-ray is shown below:

Which of the following abnormalities is most likely to be present in this patient?
Increased diffusing capacity of carbon monoxide
Increased residual volume
Decreased FEV1/FVC ratio
Increased PaCO2
Increased A-a gradient
A 34-year-old woman presents with one week of low-grade fever, diarrhea, and lethargy plus two days of hemoptysis and severe pleuritic-type chest pain. In the past she abused heroin but is currently in a methadone program. She has a 20 pack-year cigarette smoking history. Her medical history is significant for HIV and hepatitis C infections. Her last CD4 count was 350/μl two months ago. PPD testing revealed 2 mm of induration at the same time. On physical examination today, her blood pressure is 130/80 mmHg, heart rate is 100/min, and temperature 38.1°C (100.6.F). Breath sounds are diminished at the base of the right lung. Chest CT is shown below.

Which of the following is the most likely diagnosis?
Pulmonary tuberculosis
Bacterial pneumonia
Pulmonary thromboembolism
Lung cancer
Pneumocystis pneumonia
A 60-year-old Caucasian female comes to the physician because of progressive shortness of breath for the past month. She has had a 13.6 kg (30 lb) weight loss during this period. She has a history of hypertension and hypothyroidism and takes metoprolol and levothyroxine. She has smoked two packs of cigarettes daily for 35 years. Her temperature is 36.7 C (98 F), blood pressure is 130/70 mmHg, pulse is 80/min, and respirations are 20/min. On examination, decreased breath sounds and dullness to percussion are noted on the right, middle and lower lobes of the lung. Her chest x-ray is shown below.

Which of the following is the most appropriate next step in the management?
Bronchoscopy
Video-assisted thoracoscopy
Mediastinoscopy
Open pleural biopsy
Thoracentesis
A 3-year-old boy presents to the emergency department with a fever and difficulty breathing. He is the product of a normal pregnancy and has been healthy since birth. His immunizations are up to date. This morning he appeared to be in his usual state of health and was dropped off at day care by his father. Later on, his teacher noticed that he had suddenly become fussy and flushed and could not be consoled with toys, rocking, or hearing a story. He also felt warm to the touch and was drooling more than usual. When she took his temperature, it was 39°C (102.2°F). His parents were contacted immediately, and the patient was brought to the emergency department. He appears toxic and anxious, and has loud labored breathing. He is sitting upright, bracing himself on his arms, with his neck hyperextended and mouth open. His temperature is 40°C (104°F), respiratory rate is 50/min, pulse is 140/min, blood pressure is 102/62 mm Hg, and oxygen saturation is 100% on room air. Lateral x-ray of the neck is shown in the image. Laryngoscopy reveals a large cherryred epiglottitis. What is the most appropriate next step in management?

Antibiotic therapy
Observation
Corticosteroids
Tracheostomy
Nasotracheal intubation
A 21-year-old nonsmoking college student comes to the local emergency department because pf cough, weight loss, and low-grade fever. Occasionally his sputum is tinged with blood. X-ray of the chest is shown in the image. He reports traveling to Haiti on a “medical mission” trip several years ago. Which of the following is the most likely diagnosis?

Aspergillosis
Sarcoidosis
Klebsiella infection
Tuberculosis
Lung cancer
A 25-year-old man is recovering in the hospital from an open repair of his broken femur, which he suffered during an automobile accident. On postoperative day 3 he develops sudden onset shortness of breath and vague chest discomfort. His temperature is 37.6°C (99.6°F), heart rate is 108/min, blood pressure is 95/62 mm Hg, respiratory rate is 42/min, and oxygen saturation is 89% on room air. Physical examination is significant for jugular venous distention to 9 cm and an accentuated pulmonic component of S2. A pulmonary angiogram is shown in the image. Which of the following is most likely to be decreased?

Airway resistance
Pulmonary compliance
Alveolar dead space
Pulmonary vascular resistance
Alveolar ventilation
A 24-year-old African American woman presents with mild dyspnea on exertion, fever, and a rash on her legs. Her symptoms have come on gradually and she reports no pleuritic chest pain, hemoptysis or sputum production. She has no significant past medical history, smokes 10 cigarettes/day and is not taking any medications. Physical examination reveals generalized lymphadenopathy and tender erythematous nodules on her legs. CXR shows bilateral symmetric hilar adenopathy and reticulonodular changes in both lungs. She has a restrictive lung disease pattern on pulmonary function testing. Which of the following is the most likely diagnosis?

Hodgkin’s disease
Sarcoidosis
Tuberculosis
Rheumatoid arthritis (RA)
Rheumatic fever
A 30-year-old man presents with coughing up blood and sputum. There is no associated dyspnea, fever, or pleuritic chest pain. His past medical history is significant for recurrent pneumonias and a chronic cough productive of foul-smelling purulent sputum. The sputum production is usually worse when lying down and in the morning. He quit smoking 5 years ago and started when he was 18 years old. On physical examination, he appears chronically ill with clubbing of the fingers. Wet inspiratory crackles are heard at the lung bases posteriorly. CXR shows scaring in the right lower lobe, which on chest CT scan is identified as airway dilatation, bronchial wall thickening, and grapelike cysts. Which of the following is the most likely diagnosis?

Bronchiectasis
Pulmonary neoplasm
Chronic bronchitis
Chronic obstructive emphysema
Disseminated pulmonary tuberculosis
A 58-year-old steam pipe worker presents with a vague ache in the left chest and mild dyspnea of several months’ duration. There is dullness on percussion of the left chest associated with diminished breath sounds. His CXR is shown in Fig. Which of the following is the most likely diagnosis?

Pleural metastases
Mesothelioma and asbestosis
Paget’s disease
Pleural effusion
Multiple myeloma
A 27-year-old man presents with chest pain and feeling unwell. He describes cough with blood-tinged sputum, chills, and fever of 2 days’ duration. Physical findings reveal dullness and moist rales in the left lower chest. His CXR is shown in Fig. Which of the following is the most likely diagnosis?

Pneumonia, left lower lobe
Tuberculosis
Atelectasis, left lower lobe
Sarcoidosis
PE
A 40-year-old man is seen for an insurance assessment. He has no past medical history and feels well. His compete physical examination is normal. His biochemistry, complete blood count (CBC), ECG, and urinalysis are also normal. His CXR is abnormal and presented in Fig. Which of the following is the most likely diagnosis?

Hamartoma of the lung
Bronchogenic carcinoma
Tuberculous granuloma of the left apex
Pulmonary metastases
Osteochondroma of the left 4th rib
A 21-year-old man has a nonproductive cough, shortness of breath, and chest pain, which changes with breathing. He also has pain in the left arm. On examination, there is tenderness over the left shoulder, heart sounds are normal, and the lungs are clear. CXR reveals a lytic lesion in the left humerus and reticulonodular opacities in the upper and middles lobes. The eosinophil count is normal. Which of the following is the most appropriate initial diagnostic test?

Lung biopsy
Bronchoscopy
Humerus bone biopsy
Pulmonary function tests
CT scan of chest
The pulmonary function studies shown in Table 12–1 are of a 65-year-old man with severe dyspnea and cough. Which of the following is the most likely diagnosis?

Emphysema
Acute bronchitis
Lobar pneumonia
CHF
Chronic bronchitis
A 34-year-old male presents to the emergency department with a red eye. He says, "I just woke up this morning and saw that my right eye was red." He denies any itching, pain or discharge. He has no known drug or environmental allergies. He takes no medication. His vital signs are stable. The photo of his eye is shown below.

What is the best next step in his management?
Check intraocular pressure
Observation
Refer to ophthalmologist
Antibiotics
Check coagulation parameters
A 31-year-old nurse in your hospital has noticed a lesion in her left eye. She denies change in vision, pain, fevers, or discharge. A picture of her eye is shown below. Which of the following is the most likely diagnosis?

Hordeolum
Dacryocystitis
Chalazion
Pinguecula
Pterygium
A 21-year-old man presents to the ED with a red eye. The patient complains of rhinorrhea and a nonproductive cough but has no eye pain or discharge. He also has no associated ecchymosis, bony tenderness of the orbit, or pain on extraocular eye movement. His vision is normal, extraocular movements are intact, and intraocular pressure (IOP) is 12. A picture of his eye is shown below. What is the most appropriate management of this condition?

Call ophthalmology immediately.
Administer ophthalmic timolol
Administer 1% atropine
Reassurance only
Elevate patient’s head
A 65-year-old man with a history of diabetes, hypertension, coronary artery disease, and atrial fibrillation presents with loss of vision in his left eye since he awoke 6 hours ago. The patient denies fever, eye pain, or eye discharge. On physical examination of the left eye, vision is limited to counting fingers. His pupil is 3 mm and reactive. Extraocular movements are intact. Slit-lamp examination is also normal. The dilated funduscopic examination is shown below. Which of the following is the most likely diagnosis?

Retinal detachment
Vitreous hemorrhage
Central retinal artery occlusion
Acute angle-closure glaucoma
Central retinal vein occlusion
A 22-year-old female is referred to the dermatology clinic. Over the past few years, she has noticed small areas of depigmentation on her arms and legs. Some of these areas are well-circumscribed, as shown in the picture below.

She is otherwise well. Her only medication is the oral contraceptive pill. She is currently sexually active with more than one partner. Which of the following diseases is most likely to be associated with her skin condition?
Type-2 diabetes mellitus
Zollinger-EIIison syndrome
Hypoparathyroidism
HIV infectio
Pernicious anemia
A 28-year-old Caucasian woman comes to the office for a routine skin exam. On exam, you encounter a dark-colored lesion. The patient states that she has had a spot there her whole life. She does state that it has recently "been a little itchy and hurts sometimes." She gives a history of sunburns during childhood, and says that she is very "sun-sensitive." A picture of the mole is shown below.

Which of the following is the most likely diagnosis?
Keratoacanthoma
Melanocytic nevus
Blue nevus
Lentigo simplex
Melanoma
An 80-year-old woman comes to the office and appears very upset. She requests removal of a lesion on her neck because "it is greasy and unsightly." She is tired of people constantly staring at her neck. The lesion has been present "for quite a while," and has been gradually darkening. Aside from occasional itching, there are no other symptoms. A picture of the lesion is shown below.

What is the most likely diagnosis?
Basal cell carcinoma
Actinic keratosis
Melanoma
Acrochordon
Seborrheic keratosis
A 45-year-old man is brought to the office due a sudden onset of skin lesions and fever. He is unable to eat or drink due to the pain in his mouth and throat. His wife says that he was complaining of a headache, malaise, and joint pain prior to developing the skin lesions. Generally, he has been in good health, other than an episode of sinusitis, for which he was prescribed trimethoprim-sulfamethoxazole 5 days ago. His pulse is 92/min, blood pressure is 110/80 mmHg, respirations are 14/min, and temperature is 36.8C (98.4F). On examination, both conjunctivae are inflamed. There is erythema, blistering and ulceration over the oral mucosa. There is an erythematous rash over the trunk and cutaneous lesions over the hands, arms and feet. Some of the lesions are shown in the picture below.

What is the most likely diagnosis?
Stevens-Johnson syndrome
Toxic shock syndrome
Erythema multiforme minor
Impetigo.
Staphylococcal scalded skin syndrome
A 42-year-old woman presents with painful skin lesions. She is unable to eat or drink because the lesions have involved her mouth and throat. Her other complaints include malaise, headache, sore throat, cough, nausea and vomiting prior to the onset of the skin lesions. She was in perfect health in the past, other than an episode of urinary tract infection 3 days ago. She was prescribed trimethoprim-sulfamethoxazole combination for this infection. Her pulse is 92/min, respirations are 14/min, blood pressure is 140/90 mm Hg, and temperature is 38.3C (101 F). On examination, the skin is hot and tender with erythematous macules. The oral mucosa shows blistering and erosions. A picture of her back is shown below.

What is the most likely diagnosis?
Exfoliative dermatitis
Erythema multiforme minor
Staphylococcal scalded skin syndrome
Stevens Johnson's syndrome
Toxic epidermal necrolysis
A 20-year-old female comes to the office and complains of rough, dry and scaly skin. Her skin was normal at birth, but gradually became dry. The dryness increases during the winter months, despite regular application of body-moisturizing lotion. An image of the patient's skin lesions is shown below.

What is the most likely diagnosis?
Atopic dermatitis
Lmpetigo
Irritant contact dermatitis
Psoriasis
Ichthyosis vulgaris
A 35-year-old male presents to your office with red skin lesions on his back that were first noticed by his wife. His past medical history is not significant. Physical examination reveals the following findings (see the slide below).

Which of the following is the most likely diagnosis in this patient?
Strawberry (capillary) hemangioma
Cavernous hemangioma
Cherry hemangioma
Cystic hygroma
Spider angioma
A 65-year-old male comes to the office on a hot summer afternoon. He complains of blisters and intense itching all over his body for the past 2 days. He has been having "itchy red swelling all over" for the past 2 months, which he thinks is due to the summer heat. His pulse is 82/min, blood pressure is 140/80 mm Hg, respirations are 14/min, and temperature is 36.8C (98.4F). On examination, lesions are seen on both normal and erythematous skin over flexural areas of the groin, axilla and legs. An image of one of these lesions is shown below.

Which of the following is most likely seen with this patient's condition?
LgG and C3 deposits at the dermal-epidermal junction
C3 at the basement membrane zone
LgG deposits intercellularly in the epidermis
Intradermal edema with leukocyte infiltration
LgG deposits in a linear band at the dermal-epidermal junction
A 31-year-old male presents to your office with a velvety skin rash in his axilla as shown on the slide below.

Which of the following is the most likely cause of this patient's condition?
Vitamin D resistance
Insulin resistance
Calcitonin hypersecretion
Serotonin hypersecretion
Testosterone unresponsiveness
A 70-year-old Caucasian male presents to your office for evaluation of skin lesions on his forehead. On physical exam you find that these papules have a sandpaper texture by palpation. The lesions are illustrated in the slide below.

Which of the following is the most likely diagnosis in this patient?
Psoriasis
Atopic dermatitis
Seborrheic keratosis
Pityriasis rose a
Actinic keratosis
A 45-year-old male comes to you with complaints of throbbing pain over the pulp of his right index finger for the last two days. He has been feeling warm for the last three days. He denies ever having any sexually transmitted disease or cold sores in the past. On examination, he has a swollen, soft, and tender distal pulp space of the right index finger with some non-purulent vesicles. A picture of his hand is shown below.

Tzanck smear of the vesicles show multinucleated giant cells. Which of the following is most likely the occupation of this patient?
A dentist
A tailor
Commercial sex worker
A Pilot
A gardener
A 12-year-old boy notices a scaly, mildly pruritic rash on his arm (see image below). There is no associated fever, muscle pain, nausea, vomiting, diarrhea, or back pain. He recently started taking swimming classes.

The rash is most likely to clear with which of the following therapies?
Nafcillin
Terbinafine
Corticosteroids
Acyclovir
Retinoids
A 25-year-old male presents with skin lesions over his elbows, knees and neck. He complains of intense itching and burning sensation over these lesions for the past 10 days. He was advised to follow a gluten-free diet on his previous visit, but was not compliant. His vital signs are stable. On examination, there are flesh-colored to erythematous vesicles distributed over the extensor aspects of elbows, knees, posterior neck and shoulders. Some of these lesions are shown in the picture below.

Which of the following is the drug of choice for his skin condition?
High potency steroids
Azathioprine
Low dose acyclovir
Dapsone
1% lindane solution
A 22-year-old male presents with a 6-month history of a red, nonpruritic rash over the trunk, scalp, elbows, and knees. These eruptions are more likely to occur during stressful periods and have occurred at sites of skin injury. The patient has tried topical hydrocortisone without benefit. On examination, sharply demarcated plaques are seen with a thick scale. Pitting of the fingernails is present. There is no evidence of synovitis. What is the best first step in the therapy of this patient’s skin disease?

Photochemotherapy (PUVA)
Oral cyclosporine
Oral methotrexate
Topical fluticasone
Topical calcipotriene
A 35-year-old woman develops an itchy rash over her back, legs, and trunk several hours after swimming in a lake. Erythematous, edematous papules and plaques are noted. The wheals vary in size. There are no mucosal lesions and no swelling of the lips. What is the best first step in management of her symptomatic rash?

Subcutaneous epinephrine
Aspirin
Intravenous glucocorticoids
Oral doxycycline
Oral antihistamines (H1 blockers)
A 23-year-old, HIV-infected female presents with a five-day history of fever and productive cough. She is on antiretroviral therapy, and her CD4 count is 300/mm3. Her temperature is 39.0C (102.5F), pulse is 95/min, respirations are 22/min, and blood pressure is 115/76 mm Hg. Physical exam reveals dullness to percussion and bronchial breath sounds in the right lung base. Chest x-ray is shown below.

What is the most likely cause of this patient's symptoms?
Mycobacterium tuberculosis
Streptococcus pneumonia
Disseminated coccidioidomycosis
Pneumocystis jiroveci (P. jiroveclj
Pseudomonas aeruginosa
A 25-year-old man is admitted with fever and rust-colored sputum. He looks unwell, temperature 38.4°C, pulse 100/min, and blood pressure 115/80 mm Hg. On auscultation, there are bronchial breath sounds in the right axilla and inspiratory crackles. The CXR is shown in Fig. Which of the following is the most likely diagnosis?

Right middle lobe pneumonia
Loculated pleural effusion
Aspergilloma
Aspiration pneumonia
Right lower lobe pneumonia
The dental condition illustrated in Fig is usually associated with a congenital infectious disease. The teeth are characterized by centrally notched, widely spaced, peg-shaped upper central incisors and molars that have poorly developed cusps. Which of the following is the most likely diagnosis?

Congenital measles
Congenital rubella
Congenital syphilis
Congenital toxoplasmosis
Congenital HIV
A 22-year-old female presents to the office with a three-day history of rash, fever, and malaise. There is no burning or itching associated with the rash. Two weeks ago, she had been camping in northern Massachusetts, and noted a tick bite after walking through the woods. She is twelve weeks pregnant. The rash is shown below. The examination is otherwise unremarkable.

What is the most appropriate treatment for this patient?
Amoxicillin
Doxycycline
Azithromycin
Ceftriaxone
Penicillin G
A 40-year -old man who underwent a renal transplant six months ago comes to the clinic with fever, chills, and a productive cough. His temperature is 39.4C (103 F), pulse is 110/min, respirations are 22/min, and blood pressure is 110/65 mmHg. Chest x-ray shows a right lower lobe nodule with a cavity. Sputum gram stain is shown below. What is the most appropriate treatment of this patient's condition?

Trimethoprim-sulfamethoxazole
Penicillin
Vancomycin
Gentamycin
Metronidazole
A 29-year-old male, known intravenous drug user presents to the emergency department with a chief complaint of dyspnea. Over the last few days, he has become short of breath and he has very little exercise tolerance. His other symptoms are a persistent dry cough, low-grade fever for the past two days, watery diarrhea, abdominal cramps, and general malaise. He self-treated his fever with acetaminophen. He has a history of anaphylaxis with sulfonamides. Physical examination reveals an emaciated man with numerous needle marks on his hands. Arterial blood gas analysis reveals a PCO2 of 32 mm Hg and PO2 of 64 mm Hg on room air. The chest x-ray is shown below:

Which of the following is the most appropriate initial treatment regimen for this patient?
Acyclovir and azithromycin
Penicillin and acyclovir
Pentamidine and azithromycin
Tetracycline and azithromycin
Ganciclovir and azithromycin
A 27-year-old man presents with fever, malaise, anorexia, and fatigue for the last three days. He denies cough, chest pain, arthralgias, and diarrhea. He has history of rheumatic heart disease and recently underwent a dental cleaning. His temperature is 38.5C (101.3F), pulse is 90/min, respirations are 18/min, and blood pressure is 135/76 mm Hg. Examination of his fingernail is shown below.

Cardiovascular examination reveals an early diastolic murmur in the mitral area. The chest x-ray is negative. Urinalysis shows microscopic hematuria. What is the most appropriate next step in the management of this patient?
Do transthoracic echocardiography
Start antibiotics immediately and then obtain blood cultures
Start antibiotics after drawing blood for culture
Do transesophageal echocardiography
Give aspirin and start his penicillin prophvlaxis
A 50-year-old woman develops pink macules and papules on her hands and forearms in association with a sore throat. The lesions are target like, with the centers a dusky violet. What causes of this disorder are most likely in this patient?

Tampons and superficial skin infections
Anxiety and emotional stress
Drugs and herpesvirus infections
Harsh soaps and drying agents
Rickettsial and fungal infections
A 32-year-old homosexual male with HIV infection presented to his physician with skin lesions. He first noted these lesions last month, and has since observed a change in color from pink to violet. There is no associated pain, itching, or burning. He was diagnosed with HIV infection three years ago and has been noncompliant with his medications. His pulse is 80/min, blood pressure is 115/70 mm Hg, respirations are 14/min, and temperature is 37.1 C (98.8F). The appearance of his lesions is illustrated below:

His CD4 count is 30/microl, and viral load is 300,000copies/ml. Which of the following is the most likely cause of his current condition?
Human papillomavirus
Human herpesvirus 8 (HHV-8)
Pneumocystis jiroveci
Poxvirus
Herpes simplex type 2 (HSV-2)
A 25-year-old female with blonde hair and fair complexion complains of a mole on her upper back. The lesion is 8 mm in diameter, darkly pigmented, and asymmetric, with an irregular border (see illustration below). Which of the following is the best next step in management?

Tell the patient to avoid sunlight
Obtain full-thickness excisional biopsy
Follow the lesion for any evidence of growth
Obtain shave biopsy.
Obtain metastatic workup
A 46-year-old construction worker is brought to the clinic by his wife because she has noticed an unusual growth on his left ear for the past 8 months (see photo below). The patient explains that, except for occasional itching, the lesion does not bother him. On physical examination, you notice an 8-mm pearly papule with central ulceration and a few small dilated blood vessels on the border. What is the natural course of this lesion if left untreated?

This is a benign lesion and will not change
Local invasion of surrounding tissue and metastasis via lymphatic spread
Local invasion of surrounding tissue
Disseminated infection resulting in septicemia
Regression over time
A 50-year-old male comes to the office due to an ulcer in his right foot. He has type 2 diabetes, for which he takes glyburide. Laboratory investigations reveal an HbA1c of 9%, and random blood sugar of 180 mg/dl. X-ray of the leg/foot is normal. A picture of the foot ulcer is shown below.

Which of the following is the most appropriate management of this patient's foot ulcer?
Start aspirin and atorvastatin
Prescribe oral antibiotics and follow-up as an outpatient
Perform thorough debridement of the wound
Amputation
Prescribe tight-fitting shoes
A 46-year-old female complains of a "sandy" sensation in her eyes. Review of systems is notable for a 6-pound weight loss over the last month. A picture of her eyes is shown on the slide below.

Which of the following most likely underlies this finding?
High circulating thyroxine level
Increased intraocular pressure
Periorbital lymphocytic infiltration
Increased intracranial pressure
Bilateral facial nerve compression
A 25-year-old female comes to the office for a follow-up visit. She was just diagnosed with type 1 diabetes mellitus a few days ago, when she presented at the emergency department with ketoacidosis. After successful management of her diabetic ketoacidosis (DKA), she was sent home on an insulin regimen with the following dosage:
Before breakfast 10 units of NPH and 10 units of regular insulin
Before supper 10 units of NPH and 4 units of regular insulin
During this office visit, she shows the record of her fingerstick readings at home.
blood glucose levels were:
blood glucose levels were:

What is the most likely explanation for her 7:00 am blood glucose level?
Spikes of growth hormone release
Destruction of glucagon-secreting cells
Epinephrine, norepinephrine, & glucagon release
Decrease Insulin-secretor
Waning of insulin levels
A 19-year-old G1P0 woman at 32 weeks’ gestation presents for scheduled prenatal appointment. The pregnancy has been uncomplicated to date. However, she mentions that she recently noticed a hard lump on her neck. She denies pain or difficulty swallowing, speaking, or breathing. Physical examination reveals a firm, nontender, immobile, solitary nodule on the left hemithyroid. Ultrasound reveals a solid 2-cm mass. There is no cervical lymphadenopathy. Thyroid function tests reveal a thyroid-stimulating hormone level of 1.2 μU/mL and free thyroxine level of 0.9 ng/dL. Results of fine-needle aspiration biopsy are shown in the image. Which of the following is the best next step in management?

Left hemithyroidectomy
Start methimazole
Monitor until after delivery
Start propylthiouracil
Radioablation therapy
A 30-year-old female complains of palpitations, fatigue, and insomnia. On physical examination, her extremities are warm and she is tachycardia. There is diffuse thyroid gland enlargement and proptosis. There is thickening of the skin in the pretibial area. Mild clubbing of digits is present. Which of the following laboratory values would you expect in this patient?

Increased free thyroxine (free T4), increased TSH
Normal free thyroxine, elevated triiodothyronine (T3), normal TSH
Increased free thyroxine, decreased TSH
Normal free thyroxine, decreased TSH
Increased free thyroxine, normal TSH
A 17-year-old girl has never had a menstrual period. On physical examination, she has minimal breast development and no axillary or pubic hair. She is color blind and has had a diminished sense of smell since birth. Laboratory evaluation would most likely reveal which of the following?

A
D
B
E
C
A 6-year-old boy is brought to his pediatrician for a routine check-up. He has not been seen by a physician for the past 3 years. Recently, he has developed some patchy areas of hair loss on his scalp. The mother also notes he has had many colds over the past year. She says he has developed normally, although he started walking later than her other two children. On physical examination his wrists appear enlarged, and he has bowing of the forearms and legs. X-ray of the boy’s legs is shown in the image. Laboratory tests show a calcium level of 7.1 mg/dL, phosphate of 1.8 mg/dL, and intact parathyroid hormone of 130 pg/mL (normal: 10–65 pg/mL). Vitamin D level is normal. Treatment with vitamin D does not correct the patient’s hypocalcemia. Which of the following disorders best explains this patient’s findings?

Dietary vitamin D deficiency
Pseudohypoparathyroidism
Hypoalbuminemia
Vitamin D-resistant rickets
Primary hyperparathyroidism
A 14-year-old boy presents at the pediatric clinic for a routine check-up. The patient had developed end-stage renal disease over the previous 2 years, and was successfully treated with a renal transplant 6 months prior. Since his operation, he has developed purple striae on his back and arms, central obesity, and an increasingly round face. During the subsequent blood analysis, which of the following results would be most likely?

A
D
B
E
C
A 79-year-old woman presents to her primary care physician complaining of memory loss. She reports increasing difficulty balancing her check book and remembering the names of new acquaintances over the last several months. Her only other complaint is occasional urinary incontinence, which she attributes to old age. She denies headache, vision changes, rash, nausea, or vomiting. Her past medical history is significant for hypertension controlled with felodipine. On exam her vital signs are within normal limits. The heart and lung exams are also unremarkable. The cranial nerves are intact, fundoscopic exam is normal, and no tremor is observed. Her gait is slow and shuffling, there is no dysmetria, and her Folstein mini-mental status score is 24/30. CT scan of her brain is shown below:

Which of the following interventions is most likely to relieve her symptoms?
Ventriculoperitoneal shunt
Vitamin B12 replacement
Hematoma evacuation
High-dose penicillin
Levodopa/carbidopa
An 86-year -old known hypertensive woman is brought to the emergency department due to weakness of her left side, confusion, drowsiness and slurred speech for the last 2 hours. Her past medical history is significant for an inferior wall myocardial infarction 12 years ago, chronic atrial fibrillation, and severe backache secondary to osteoarthritis. She is currently on aspirin, warfarin, losartan, indomethacin, atenolol, and simvastatin. She doesn't go to anticoagulation clinic regularly. Her blood pressure is 180/110 mm Hg, temperature is 38C (100 F), respirations are 16/min, and pulse is 70/min, irregularly irregular. The pertinent physical findings are: carotid bruit on both sides, 2/5-muscle
strength in the left arm and leg, and slurred speech. Her deep tendon reflexes are exaggerated on the left side, and the Babinski sign is positive. EKG reveals atrial fibrillation. Her CT scan (performed in the ED) is shown below.
strength in the left arm and leg, and slurred speech. Her deep tendon reflexes are exaggerated on the left side, and the Babinski sign is positive. EKG reveals atrial fibrillation. Her CT scan (performed in the ED) is shown below.

What is the most likely diagnosis?
Cerebral haemorrhage
Lacunar infarction
Cerebellar hemorrhage
Subarachnoid haemorrhage
Cerebral infarction
A 74-year-old Caucasian woman is brought to the emergency department after a fall. Her husband is concerned since she is on "blood thinners." Her other medical problems include hypertension, hearing loss, congestive heart failure, coronary artery bypass graft, transient ischemic attack, and atrial fibrillation. She does not use tobacco, alcohol, or drugs. Her medications include aspirin, metoprolol, digoxin, furosemide, and warfarin. Her temperature is 37.2 C (99 F), blood pressure is 140/90 mmHg, pulse is 72/min, and respirations are 14/min. CT scan of the head without contrast is shown below.

Which of the following is the most likely cause of her condition?
Tearing of middle meningeal artery
Rupture of an aneurysm
Tearing of bridging veins
Tumor of the arachnoid granulation
Hypertensive hemorrhage
A 45-year-old white male presents with a 4-month history of headaches. The headache is generalized, dull, constant, and worsened by bending, coughing and sneezing. It is unresponsive to simple analgesics, and associated with nausea and vomiting. His wife says he has been acting strangely for the last few months, and she has noted a personality change. The neurological examination is non-focal. Fundoscopy reveals papilledema. His CT scan is shown below.

Which of the following is the most likely diagnosis?
Brain abscess
Low-grade astrocytoma
Metastatic brain tumor
Cerebral infarction
Glioblastoma multiforme
A 38-year-old female presents with one week of "shakiness" in her right arm, right leg weakness and unsteady gait. An MRI of her brain is shown below:

Which of the following is the best treatment for this patient?
Aspirin and simvastatin
Tissue plasminogen activator
Glatiramer acetate
Broad-spectrum antibiotics
Argatroban
A 64-year-old Caucasian female is rushed to the emergency department (ED) due to a sudden onset of severe headache and altered mental status. By the time she arrived at the ED, she had deteriorated to a stuporous state. She developed a fever and severe dry cough yesterday, but did not take any medicine nor consult her physician. Her medical problems include hypertension, coronary artery disease, atrial fibrillation, mitral valve regurgitation, and psoriasis. Her medications include aspirin, metoprolol, warfarin, amiodarone, and multivitamin tablets. Her blood pressure is 162/80 mm Hg, pulse is 80/min, respirations are 16/min and temperature is 37C (98F). Her lab results are:
Hb 13 g/dl
WBC 11,000/cmm
Platelets 180,000/cmm
Blood Glucose 118 mg/dl
Serum Na 138 mEq/L
Serum K 4.5 mEq/L
BUN 16 mg/dl
Serum Creatinine 1.0 mg/dl
PT 25.0sec
INR 4.0
WBC 11,000/cmm
Platelets 180,000/cmm
Blood Glucose 118 mg/dl
Serum Na 138 mEq/L
Serum K 4.5 mEq/L
BUN 16 mg/dl
Serum Creatinine 1.0 mg/dl
PT 25.0sec
INR 4.0

Which of the following is the most appropriate next step in management?
Give fresh frozen plasma
Stop warfarin and start heparin
IV infusion of vitamin K
Obtain liver function panel
Order t-PA
A 40-year-old Caucasian male comes to the emergency department because he is having "the worst headache" of his life. The headache is of sudden onset, and associated with nausea and vomiting. He denies any fever and trauma to head. He is not taking any medications. He has a history of migraine headaches. The neurological examination is non-focal. CT scan of the head without contrast is shown below.

Which of the following is the most likely cause of this patient's headache?
Hypertension
Extension of primary intracerebral hemorrhage
Rupture of saccular aneurysm
Amyloid angiopathy
Rupture of AV malformation
A 76-year-old man is brought to the emergency department by his son who found him confused in his apartment. The son also reports that his father has been limping for the past two days. The patient's past medical history is significant for hypertension, diabetes mellitus, and cataract surgery six months ago. His medications are metoprolol, enalapril, and glyburide. He has also been taking ibuprofen for recent headaches. A head CT scan is obtained and is shown below.

Which of the following is the most likely cause of this patient's condition?
Carotid artery atherosclerosis
Ruptured aneurysm
Small vessel hyalinosis
Recent eye surgery
Blunt head trauma
A 43-year-old male (Patient A) is being evaluated for an esophageal disorder. Esophageal manometry tracings after a single swallow of 5 ml of water are shown on the slide below.

UE: upper esophagus
ME: middle esophagus
LES: lower esophageal sphincter
Which of the following is the most likely diagnosis in this patient?
Cricopharyngeal dysfunction
Gastroesophageal reflux
Diffuse esophageal spasm
Mallory-Weiss syndrome
Achalasia
A 44-year-old white female presents with a 2-month history of low-grade fever, abdominal pain and bloody diarrhea. Over the past two days, her symptoms have increased. She does not use medications and she has no allergies. She has had a 10 lb (4.5 kg) weight loss over the past four weeks. Her temperature is 38.9C (102F), blood pressure is 102/70 mm Hg, pulse is 118/min, and respirations are 22/min. Examination shows pale and dry mucus membranes. Abdominal examination shows diffuse tenderness and distention.
Laboratory studies show:
Hb 9.5 g/dl
WBC 16,000/cmm
Serum Na 145 mEq/L
Serum K 3.0 mEq/L
An x-ray film of the abdomen is shown below
Laboratory studies show:
Hb 9.5 g/dl
WBC 16,000/cmm
Serum Na 145 mEq/L
Serum K 3.0 mEq/L
An x-ray film of the abdomen is shown below

Which of the following is the most likely diagnosis?
Crohn's disease
Pseudomembranous colitis
Toxic megacolon from ulcerative colitis
Obstructed colon cancer
S. Aureus gastroenteritis
A 54-year-old male presents to the emergency department with a 1-week history of abdominal pain. His other symptoms are nausea, vomiting, low-grade fever, and loss of appetite. He does not use alcohol. He has a seizure disorder, for which he takes a "prescription drug." X-ray films of his chest and abdomen show no abnormalities. His abdominal CT scan is shown below.

Which of the following is the most likely explanation for this patient's abdominal symptoms?
Gall bladder pathology
Air in the stomach
Kidney pathology
Liver pathology
Pancreas pathology
A 74-year-old man presents to the emergency department with abdominal pain. The pain is deep and aching and is localized to the left lower quadrant. The man reports multiple episodes of diarrhea over the preceding week. He also reports having multiple similar episodes of abdominal pain in the past. On physical examination he is febrile and has tenderness to palpation of the left lower quadrant. His WBC count is 23,000/mm³. Results of CT are shown in the image. Which of the following is the most likely diagnosis?

Angiodysplasia
Diverticulitis
Carcinoid syndrome
Infectious colitis
Carcinoma of the colon
A 47-year-old woman presents to the emergency department with an 8-day history of left lower quadrant pain and semi-formed stools. Starting this afternoon, she has noticed blood in her stool as well as dizziness when she gets up from sitting. She denies fever, nausea, vomiting, weight loss, and night sweats. Her temperature is 37°C (98.6°F), heart rate is 104/ min, blood pressure is 120/82 mm Hg supine and 103/63 mm Hg when she sits up, and respiratory rate is 18/min. Physical examination reveals no peritoneal signs and is remarkable only for fecal occult blood on rectal examination. Laboratory results reveal a WBC count of 13,000/mm³ and hematocrit of 29%. Results of an x-ray of the abdomen are shown in the image. What is the best next step in management?

Angiography with embolization
Nothing by mouth, nasogastric tube, and broad-spectrum antibiotics
Immediate surgery for partial colectomy
Place the patient on a high-fiber diet
Intravenous hydration and blood transfusion
A 75-year-old woman with a history of diabetes and coronary heart failure presents to the emergency department because of increasing abdominal girth. In recent months she has been feeling increasingly fatigued, and although she has had decreased appetite, she has gained weight. Her heart rate is 100/min and blood pressure is 112/70 mm Hg. She has scleral icterus; the skin over her face, neck, and lower legs is slightly bronze in color; she has palmar erythema; and she has numerous ecchymoses over her body. Her abdominal examination is significant for ascites. Laboratory tests show:
Aspartate transaminase: 102 U/L Alanine transaminase: 97 U/L Alkaline phosphatase: 300 U/L Total bilirubin: 1.9 mg/dL Albumin: 2.9 g/dL
Prothrombin time: 22 sec
Partial thromboplastin time: 42 sec
Prothrombin time: 22 sec
Partial thromboplastin time: 42 sec
An ultrasound of her abdomen shows a shrunken and nodular liver. A liver biopsy using Perls Prussian blue stain is shown in the image. Which of the following is the most likely complication of her disease?

Acute pancreatitis
Hepatocellular carcinoma
Amyloidosis
Splenomegaly
Bone marrow failure
A 45-year-old HIV-positive woman comes to her primary care physician complaining of a 2-day history of bloody diarrhea. She states that she has been feeling well until 2 days ago, when she developed abdominal pain. She denies fevers, chills, night sweats, nausea, or vomiting. She admits to feeling tired over the last couple of weeks and has had a 2.3-kg (5-lb) weight loss over the past 2 weeks. Her stool sample shows WBCs and RBCs. Her Gram stain is shown in the image. Her CD4+ cell count is 201/mm³. Which of the following is the most likely cause of this woman’s symptoms?

Escherichia coli
Mycobacterium avium complex
Kaposi’s sarcoma
Mycobacterium tuberculosis
Legionella
A 45-year-old man with a long history of alcohol intake comes into the emergency room with upper gastrointestinal (UGI) bleeding. Urgent endoscopy reveals the following findings. Which of the following is the most likely diagnosis?

Esophageal varices
Tertiary waves
Esophageal carcinoma
Barrett’s esophagus
Foreign body
A 35-year-old White man has a long past his- tory of diarrhea, rectal bleeding, crampy abdominal pain, and the passage of mucus. He now presents with a worsening of his symptoms despite taking his medications. A barium enema is performed and is shown in Fig. Which of the following is the most likely diagnosis of this new complication?

Toxic megacolon
Ischemic colitis
Amoebic colitis
Annular carcinoma
Appendicitis
A 55-year-old man presents to the ED complaining of mild diffuse abdominal pain. He states that he underwent a routine colonoscopy yesterday and was told “everything is fine.” The pain began upon waking up and is associated with some nausea. He denies fever, vomiting, diarrhea, and rectal bleeding. His BP is 143/71 mm Hg, HR is 87 beats per minute, temperature is 98.9°F, and RR is 16 breaths per minute. His abdomen is tense but only mildly tender. You order baseline laboratory tests. His chest radiograph is seen below. Which of the following is the most likely diagnosis?

Ascending cholangitis
Acute liver failure
Acute pulmonary edema
Pancreatitis
Pneumoperitoneum
A 3-year-old boy is brought to the pediatrician because his mother noticed a reddish-purple rash on his buttocks and thighs (see image). She notes that he has not seemed well since he had a mild cold 2 weeks earlier; he has been complaining of aches and pains in his legs and a stomach ache. Urinalysis shows 10–20 RBCs/ mm³ and 2+proteinuria. Which of the following is associated with this patient’s disease process?

Hemoptysis
Intussusception
High antistreptolysin O titer
Malar rash
Impaired glucose tolerance
A 65-year-old man presents to his physician complaining of difficulty swallowing, occasional chest pain, and regurgitation of food. Over the past 2 months he has lost about 7 kg (15 lb). Results of a barium swallow study are shown in the image. What test should be performed to look for possible causes of his condition?

24-hour pH monitoring
Upper endoscopy
Esophageal manometry
Urease breath test
Serum gastrin level measurement
A 58-year-old man comes to the emergency department complaining of colicky abdominal pain over the past 3 days that suddenly became more severe and constant over the past 6 hours. A contrast study is performed and results are shown in the image. What is the first-line treatment after fluid resuscitation and nasogastric tube placement?

Colonoscopy
Sigmoid colectomy
Hemicolectomy
Sigmoidoscopy
Proximal colostomy with delayed resection
A 54-year-old man presents to his primary care provider with the complaint of upper abdominal fullness and pain. He states that he has lost 2.3-4.6 kg (5-10 lb), but denies other symptoms. Physical examination reveals a firm mass in the epigastric area. Ultrasonography reveals a mass in the gastric antrum. A salivary gland biopsy reveals the pathology shown in the image. Which of the following therapies is expected to be part of his treatment plan?

Antibiotic therapy
Liver transplantation
Bone marrow transplantation
Multiagent chemotherapy
Gene therapy
A 22-year-old man with inflammatory bowel disease is noted to have a “string sign” in the ileal area on barium enema. In which of the following conditions is this sign most often seen?

In the stenotic or nonstenotic phase of the disease
With gastric involvement
In the stenotic phase only
With rectal involvement
As a rigid, nondistensible phenomenon
A 72-year-old woman notices progressive dysphagia to solids and liquids. There is no history of alcohol or tobacco use, and the patient takes no medications. She denies heartburn, but occasionally notices the regurgitation of undigested food from meals eaten several hours before. Her barium swallow is shown. Which of the following is the cause of this condition?

Growth of malignant squamous cells into the muscularis mucosa
Loss of intramural neurons in the esophagus
Scarring caused by silent gastroesophageal reflux
Psychiatric disease
Spasm of the lower esophageal sphincter
A 76-year-old man who has had multiple episodes of pancreatitis presents to his physician’s office with mild epigastric pain and 9.1-kg (20.0-lb) weight loss over the past 6 months. The patient also describes daily foul-smelling stools that “float” in the toilet bowl. The physician pulls up his electronic medical record and finds that the patient presented to the emergency department last week for the same symptoms. During that visit he had a CT of the abdomen (see image). Which of the following is the most appropriate treatment?

Endoscopic retrograde cholangiopancreatography
Surgical resection of pancreas
Pancreatic enzyme replacement
Whipple procedure
Pancreaticogastrostomy
A 58-year-old white man complains of intermittent rectal bleeding and, at the time of colonoscopy, is found to have internal hemorrhoids and the lesion shown at the splenic flexure. Pathology shows tubulovillous changes. Repeat colonoscopy should be recommended at what interval?

In 1 to 2 months
In 10 years
In 1 year
Repeat colonoscopy is not necessary
In 3 years
A male infant is delivered at 37 weeks’ gestation via cesarean section for breech presentation. The pregnancy was complicated by polyhydramnios. The 34-year-old mother is rubella immune and has blood type B. She is negative for Rh antibody, Group B streptococci, rapid plasma reagin, hepatitis B surface antigen, gonorrhea, and Chlamydia. At delivery there is no meconium. He has a birth weight of 2.7 kg (6 lb). The baby has a weak cry and is pale and frothing at the nose and mouth. He has nasal flaring and retractions, with a respiratory rate of 56/min. Heart rate is 140/min and he has a regular rhythm and a harsh 2/6 holosystolic murmur that is best heard at the left sternal border. On auscultation he has fine diffuse crackles in his lungs bilaterally. The infant is missing both thumbs and has fusion of the remaining digits of his upper extremities bilaterally. The pediatric resident is able to suction secretions from the patient’s nasopharynx and oropharynx; however, she is unable to pass a nasogastric or orogastric tube more than 10 cm down. X-ray of the chest is shown in the image. Which of the following is the most likely diagnosis?

Congenital diaphragmatic hernia
Tracheoesophageal fistula
Pyloric stenosis
Transient tachypnea of the new-born
Respiratory distress syndrome
A 2-year-old boy is brought to the emergency department. His mother reports that the patient had been well until 3 days ago, when he developed a fever and nasal congestion. He was diagnosed with otitis media in his right ear, and was started on amoxicillin with clavulanic acid by his pediatrician. He appeared to be improving until this morning, when he began to complain of abdominal pain. The pain has been intermittent, with episodes occurring every 20 minutes for several minutes each time. However, the episodes appear to be worsening and lasting longer with increasing pain. Thirty minutes ago he had an episode of nonbloody, nonbilious emesis that was followed by passage of blood- and mucus-stained stools. He is currently in no acute distress, and his vital signs are normal. A firm sausage-shaped mass is palpable in the RUQ of his abdomen. A rectal examination yields bloody mucus. He does not have any skin lesions or rashes. X-ray of the abdomen is shown in the image. Which of the following is the most likely diagnosis?

Cystic fibrosis
Henoch-Schönlein purpura
Enterocolitis
Meckel’s diverticulum
Idiopathic intussusception
A 63-year-old man is brought to the ED by EMS complaining of severe abdominal pain that began suddenly 6 hours ago. His BP is 145/75 mm Hg and HR is 105 beats per minute and irregular. On examination, you note mild abdominal distention and diffuse abdominal tenderness without guarding. Stool is heme positive. Laboratory results reveal WBC 12,500/μL, haematocrit 48%, and lactate 4.2 U/L. ECG shows atrial fibrillation at a rate of 110. A CT scan is shown below. Which of the following is the most likely diagnosis?

Abdominal aortic aneurysm
SBO
Mesenteric ischemia
Crohn disease
Diverticulitis
A 73-year-old man is seen in the ED for abdominal pain, nausea, and vomiting. His symptoms have progressively worsened over the past 2 to 3 days. The pain is diffuse and comes in waves. He denies fever or chills, but has a history of constipation. He reports no flatus for 24 hours. Physical examination is notable for diffuse tenderness and voluntary guarding. There is no rebound tenderness. An abdominal radiograph is seen below. Which of the following is the most likely diagnosis?

Constipation
Cholelithiasis
SBO
Large bowel obstruction
Inflammatory bowel disease
A 70-year-old male presents to the emergency room complaining of weakness, dizziness and back pain. He denies nausea, vomiting, diarrhea, chest pain, palpitations, shortness of breath, urinary symptoms, or black stools. His past medical history is significant for diabetes mellitus, diabetic nephropathy and retinopathy, hypertension, atrial fibrillation and chronic leg cellulitis. He takes warfarin for chronic anticoagulation. On physical examination, his blood pressure is 139/75 mmHg and his heart rate is 110 and irregular. His WBC count is 10,500/mm3, hemoglobin level is 7.0 mg/dl and platelet count is 170,000/mm3. An abdominal CT image is shown on the slide below.

Which of the following is the most likely diagnosis?
Renal cell carcinoma
Hydronephrosis
Vertebral fracture
Mesenteric ischemia
Retroperitoneal hematoma
A 24-year-old woman comes to the physician complaining of a skin rash and pain in her wrists, ankles and elbows over the past 4 days. She has also had a fever and sweats, but denies headache, nausea or vomiting. She has no significant past medical history and does not take any medications. She recently took a vacation with her new boyfriend. She denies any previous sexually transmitted diseases but acknowledges having unprotected sex with her new boyfriend. She does not use tobacco, alcohol or illicit drugs. Her temperature is 38.5°C (101.3F) and her pulse is 98/min. Her oropharynx is clear and there is no thrush or lymphadenopathy. Her abdomen is benign and the pelvic examination is within normal limits. She has pain along the tendon sheaths with active and passive hand movement. A photo of her skin rash is shown below.

Which of the following is the most likely cause of her symptoms?
Lyme disease
Syphilis
Gonococcemia
Meningococcemia
Acute HIV infection
A 33-year-old African-American woman presents with one week of painful skin lesions on her legs. She has no cough, shortness of breath or bowel symptoms, and denies any recent illness or travel. She has no other significant past medical history and does not take any medication. She smokes one pack of cigarettes and drinks one glass of wine daily. She denies a history of sexually transmitted diseases and has been married to a monogamous partner for the past eight years. Her mother was diagnosed with ovarian cancer at age 65. Her temperature is 37.2°C (98.9.F), and blood pressure is 126/76
mmHg. On examination, she has multiple tender pink to reddish nodules noted below the knee on the extensor surface, as shown below.
mmHg. On examination, she has multiple tender pink to reddish nodules noted below the knee on the extensor surface, as shown below.

Which of the following is the most appropriate next step in her management?
HIV testing
CT scan of the abdomen
Chest x-ray
Rectal swab for culture
Colonoscopy
A 71-year-old female is brought to your clinic by her daughter with a complaint of severe pain in her fingers. Her daughter says, "Mom has horrible problems with her joints and she has never tried to get help". The patient adds that her fingers have been swollen and painful for a few weeks. She claims that she had a similar condition in her foot last year. She was given a pain pill, but it was ineffective. She takes a water pill for her blood pressure.

What is the most likely diagnosis in this patient?
Gouty arthritis
Rheumatoid nodules
Severe osteoarthritis
Bone tumor
Severe psoriatic arthritis
A 52-year-old male presents with a long history of joint pain. He describes pain and stiffness of the small joints of his hand that is worse in the morning and can last several hours. He also complains of occasional digit swelling. A picture of the patient's hands is shown on the slide below.

Which of the following is the most likely diagnosis?
Crystalline arthritis
Enteropathic arthritis
Rheumatoid arthritis
Psoriatic arthritis
Sarcoidosis
Over the last six weeks a 45-year-old nurse has developed progressive difficulty getting out of chairs and climbing stairs. She can no longer get in and out of the bathtub. She has no muscle pain and takes no regular medications. She does not use alcohol and does not smoke cigarettes. On examination she has a purplish rash that involves both eyelids (see figure). There is weakness of the proximal leg muscles. What is the best next diagnostic test?

Chest x-ray
Vitamin B12 level
HLAB27
MRI scan of the lumbar spine
CPK
A 60-year-old Caucasian woman comes to the physician because of joint pains in both hands. Her other medical problems include obesity and gastroesophageal reflux disease. She does not use tobacco, alcohol, or drugs. Family history is not significant. Her medications include omeprazole and acetaminophen. Her vital signs are within limits. X-ray of the joints is shown below.

Which of the following is the most likely diagnosis?
Rheumatoid arthriti
Systemic lupus erythematosus
Osteoarthritis
Reactive arthritis
Gouty arthritis
A 72-year-old female is admitted to the ICU with severe chest pain. The initial set of cardiac enzymes is positive and her EKG reveals an anterior wall myocardial infarction. She receives treatment with aspirin clopidogrel, metoprolol nitroglycerine drip, and morphine. Two hours later, her telemetry monitor displays the following rhythm

Which of the following is the best next step in managing this patient?
Lidocaine
Defibrillation
Digoxin
Amiodarone
Immediate echocardiogram
A 67-year-old male presents to the ER with chest pain. His medical history is significant for stable angina for which he takes aspirin and isosorbide dinitrate, as well as hypertension and bronchial asthma. Occasionally, he uses an albuterol inhaler. He is admitted to the hospital and five hours later, he begins to feel lightheaded and weak. His blood pressure is 100/60 mmHg. An EKG is obtained and is shown below

Which of the following is the best next step in managing this patient?
Pacemaker insertion
Cardiac catheterization
Adenosine
Digoxin
Metoprolol
A 46-year-old man collapsed while getting out of his bed. He has been feeling weak over the last several days and has complained of vague chest discomfort. He ascribed the symptoms to a recent respiratory infection and did not visit a doctor. His mother died of a stroke and his father suffered from recurrent myocardial infarctions. He eats a balanced diet and takes a multivitamin daily. His most recent blood cholesterol level was 200 mg/dl. An ECG strip taken by EMS is shown below.

Which of the following is the best initial management of this patient?
Procainamide
Synchronized DC cardioversion
Thrombolytic therapy
Beta-blockers and aspirin
Pericardiocentesis
A 59-year-old male suffers a myocardial infarction. He is treated medically and is discharged home ten dayslater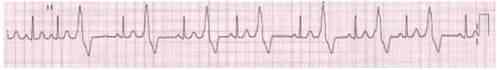 on aspirin, atorvastatin, metoprolol, lisinopril, and sublingual nitroglycerin. One month later, he presentsto your office for a follow-up visit. He denies chest pain, dyspnea or lightheadedness. His blood pressure is120/75 mmHg. His EKG is pictured below. Echocardiogram reveals an ejection fraction of 45%. What is the best next step in his management?
on aspirin, atorvastatin, metoprolol, lisinopril, and sublingual nitroglycerin. One month later, he presentsto your office for a follow-up visit. He denies chest pain, dyspnea or lightheadedness. His blood pressure is120/75 mmHg. His EKG is pictured below. Echocardiogram reveals an ejection fraction of 45%. What is the best next step in his management?
 on aspirin, atorvastatin, metoprolol, lisinopril, and sublingual nitroglycerin. One month later, he presentsto your office for a follow-up visit. He denies chest pain, dyspnea or lightheadedness. His blood pressure is120/75 mmHg. His EKG is pictured below. Echocardiogram reveals an ejection fraction of 45%. What is the best next step in his management?
on aspirin, atorvastatin, metoprolol, lisinopril, and sublingual nitroglycerin. One month later, he presentsto your office for a follow-up visit. He denies chest pain, dyspnea or lightheadedness. His blood pressure is120/75 mmHg. His EKG is pictured below. Echocardiogram reveals an ejection fraction of 45%. What is the best next step in his management?Observation
Amiodarone
Digoxin
DC cardioversion
Verapamil
A 22-year-old male presents to you with feelings of general malaise. He is always tired and has noticed that he has frequent headaches. Exam reveals an elevated arm blood pressure with a radial to femoral delay. ECG shows left ventricular hypertrophy and the chest-x ray is shown below. Close examination of the x-ray reveals a "3" sign.

What is the most likely diagnosis in this patient?
Coarctation of aorta
Tetralogy of F allot
Patent ductus arteriosus
Atrial septal defect
Aortic aneurysm
Diuretics, vasodilators and oxygen are standard inpatient therapy for patients hospitalized with left-sided heart failure. When patients are discharged, a different outpatient regimen is instituted. A team of researchers compares long-term cardiovascular mortality between patients treated with two different outpatient regimens. The study results are depicted below:

In comparison to the patients depicted by the dashed curve, those depicted by the solid line most likely received treatment with which of the following?
ACE inhibitor
Calcium channel blocker
Loop diuretic
Digoxin
Dobutamine
A 63-year-old female presents to your clinic complaining of palpitations. For the past 3 weeks, she has noticed pounding of her heart that comes and goes. Her symptoms are more frequent at night. Her only medicine is insulin for diabetes mellitus. On physical examination, she is alert and oriented, and in no distress. Her EKG is shown below.

Which of the following best accounts for this patient's symptoms?
Variable AV node conduction
Sinus arrhythmia
Irregularly irregular atrial activation
Atrial ectopy
Ventricular ectopy
A 47-year-old female, who is a chronic alcoholic, is admitted to the hospital with epigastric pain, nausea, and vomiting. Her serum amylase and lipase levels are significantly elevated and the diagnosis of acute pancreatitis is made. She is maintained nothing by mouth (NPO), and receives intravenous hydration and narcotic analgesics. On the second day of hospitalization she develops progressive shortness of breath. Her temperature is 37.2 C (98.9 F), blood pressure is 110/66 mm Hg, pulse is 110/min, and respirations are 24/min. Her oxygenation is measured at 84% on 100% non-rebreather mask and the decision is made to intubate. Since the time of admission, she has received 5 liters of normal saline and has produced 3 liters of urine output. On examination, there is no evidence of jugular venous distention. Chest auscultation reveals diffuse bilateral crackles. Auscultation of the heart reveals normal heart sounds with no murmurs. A chest x-ray from the time of admission and one from the time of intubation are shown below:

Based on these findings, what is the most likely diagnosis in this patient?
Hospital acquired pneumonia
Acute respiratory distress syndrome
Iatrogenic volume overload
Congestive heart failure from myocardial infarction
Alcoholic cardiomyopathy
A 69-year-old male undergoes coronary artery bypass and aortic valve replacement surgery. The procedure goes well, and he is extubated and discharged to the step-down unit on postoperative day 2. That night, he complains of weakness, chest tightness and shortness of breath. His blood pressure is 70/30 mmHg, respiratory rate is 26/min, and heart rate is 148 beats per minute. Lung auscultation reveals bibasilar crackles. An EKG rhythm strip is obtained:

Which of the following is the best next step in the management of this patient?
DC cardioversion
Amiodarone
Transcutaneous pacing
Lidocaine
Digoxin
An 18-year-old male complains of fever and transient pain in both knees and elbows. The right knee was red and swollen for 1 day during the week prior to presentation. On physical examination, the patient has a low-grade fever. He has a III/VI, high pitched, apical systolic murmur with radiation to the axilla, as well as a soft, mid-diastolic murmur heard at the base. A tender nodule is palpated over an extensor tendon of the hand. There are pink erythematous lesions over the abdomen, some with central clearing. The following laboratory values are obtained:
Hct: 42
WBC: 12,000/μL with 80% polymorphonuclear leukocytes, 20% lymphocytes
ESR: 60 mm/h
The patient’s ECG is shown below. Which of the following tests is most critical to diagnosis?
Hct: 42
WBC: 12,000/μL with 80% polymorphonuclear leukocytes, 20% lymphocytes
ESR: 60 mm/h
The patient’s ECG is shown below. Which of the following tests is most critical to diagnosis?

Antistreptolysin O antibody
Blood cultures
Echocardiogram
Antinuclear antibodies
Creatine kinase
You are performing medical screening of new military recruits when an 18-year-old male reports several episodes of palpitation and syncope over the past several years. Physical examination is unremarkable. An ECG is obtained with excerpts shown below. What is the most likely diagnosis?

Prior myocardial infarction secondary to coronary artery disease
Congenital prolonged QT syndrome
Hypertrophic obstructive cardiomyopathy (HOCM)
Preexcitation syndrome (Wolff-Parkinson-White)
Rheumatic mitral stenosis
A 66-year-old male is rushed to the emergency department because he feels dizzy and light-headed. He denies chest pain or palpitations. He has a history of hypertension and diabetes. His blood pressure is 116/62 mm Hg and his pulse is 35-40/min. He is alert, awake, and fully oriented. He is breathing comfortably and does not appear to be in any distress. His extremities are slightly cold and capillary refill is 3 seconds. His EKG is shown below.

Which of the following is the most appropriate next step in management?
Intravenous atropine
Intravenous adenosine push
Intravenous epinephrine
Intravenous amiodarone
Transcutaneous pacing
A 70-year-old Caucasian man comes to the emergency department because of the sudden onset of nausea, vomiting, diaphoresis, and chest pain. His other medical problems include hypertension, diabetes mellitus-type 2, and aortic stenosis. He has smoked one-and-a-half packs of cigarettes daily for 30 years and drinks 4 ounces of alcohol daily. His temperature is 37.2 C (99 F), blood pressure is 100/60 mmHg, pulse is 60/min, and respirations are 18/min. The patient's pulse oximetry showed 98% at room air. Examination shows normal first and second he sounds. Lungs are clear to auscultation. His EKG is shown below.

Which of the following is the most likely mechanism of this patient's condition?
Occlusion of the right coronary artery
Occlusion of the left circumflex artery
Occlusion of the left anterior descending artery
Inflammation of the pericardium
Vasospasm of the left circumflex artery
A 56-year-old diabetic female comes to the clinic with complaints of dizziness which has been going on for 3 weeks. She denies any dyspnea or diaphoresis. She says her blood glucose is well controlled and denies any allergy. Her BP is 155/90 mm Hg. Her chest-x ray is unremarkable and her blood work is normal. The ECG is recorded below.

What is the most likely diagnosis?
Mobitz type I heart block
Mobitz type II heart block
Complete heart block
Atrial fibrillation
First degree heart block
A 46-year-old man comes to the ER because of weakness and chest tightness. He has had these symptoms for the past one hour. He denies any past medical history. He does not smoke or drink alcohol. His father had a myocardial infarction at 68 years of age and his mother has myasthenia gravis. His EKG is shown on the slide below.

The patient should be evaluated for which of the following?
Cushing syndrome
Hyperthyroidism
Aortic dissection
High-frequency deafness
High-range proteinuria
A 46-year-old man presents to the emergency department with difficulty breathing and chest discomfort. His pain worsens with inspiration but does not radiate. He says that he has never had symptoms like this before. His past medical history is unremarkable. He works as a long-haul truck driver. On physical examination, his blood pressure is 110/70 mmHg, his heart rate is 110/min, his respiratory rate is 31/min, and his temperature is 36.7C (98.F). ECG reveals sinus tachycardia but no ischemic ST-segment or T-wave changes. His chest X-ray is shown below.

What is the most likely diagnosis in this patient?
Ascending aortic dissection
Myocardial infarction
Pneumothorax
Pulmonary embolism
Pleural effusion
A 48-year-old African American man presents to the emergency room with severe retrosternal chest pain. His temperature is 36.7C (98.F), blood pressure is 190/100 mm Hg, pulse is 100/min, and respirations are 16/min. On physical examination, his lungs are clear to auscultation and his heart sounds are normal. EKG shows evidence of left ventricular hypertrophy. A CT image of his chest is shown below.

Which of the following is the most appropriate immediate pharmacotherapy for this patient?
Labetalol
Nifedipine
Heparin
Hydrochlorothiazide
Hydralazine
A 72-year-old male is admitted to the hospital with chest pain. EKG and cardiac enzymes confirm a myocardial infarction and he is started on nitroglycerine, aspirin, simvastatin and low molecular weight heparin. Four days later, he complains of leg pain. Physical examination reveals a cold, pale leg. The angiogram is shown below.

What is the best next step in his management?
Intravenous streptokinase
Clopidogrel
Cilosta zol
Leg elevation and warm compress
Embolectomy
A 77-year-old woman comes to the emergency department because of feeling “light-headed and dizzy.” Except for the irregular pulse, her physical examination is normal. What is the rhythm in the lead tracing shown in Fig.?

First-degree heart block
Second-degree heart block
Third-degree heart block
Premature ventricular beats
Premature atrial beats
A 42-year-old woman has anterior chest pain of a somewhat atypical nature for many years. The patient’s pain has been present and relatively stable for a number of years, and the ECG shown in Fig. Is a stable one. What is the diagnosis?

Inferior wall infarction
Anterior wall infarction
Ventricular aneurysm
Nonspecific changes
Pericarditis
The ECG shown in Fig. Was obtained during the initial stages of an acute MI. The patient had just received thrombolytic therapy. What is the rhythm?

Atrial fibrillation
Atrial flutter
Second-degree heart block
Wenckebach phenomenon
Nonsustained ventricular tachycardia
A 78-year-old man with advanced renal disease has the ECG shown in Fig. (lead II). What is the diagnosis?

Hyperkalemia
Hypercalcemia
Hypernatremia
Pericarditis
Ventricular aneurysm
A 42-year -old male with a past medical history of bladder cancer and recurrent hematuria presents to the emergency room after "passing out" when he got out of bed this morning. The patient says that he was standing up to urinate shortly after waking when he began feeling dizzy. Fortunately, he was able to return to his bed before losing consciousness for 7-10 minutes. His EKG at the time of admission is shown below:

Which of the following most likely accounts for the observed EKG changes?
Ventricular preexcitation
Impaired SA node automaticity
Impaired AV node conduction
Atrial reentry
His bundle branch block
A 65-year -old Hispanic male is brought to the emergency room with severe substernal chest pain and diaphoresis that began suddenly 1 hour ago. He reports that his pain started while he was at rest and radiates to his left shoulder. The patient notes having vomited twice when the pain first began. Despite administration of 2 baby aspirins and 3 tablets of sublingual nitroglycerin, the pain persists. His initial EKG is shown below.

On physical examination, the patient's temperature is 36.9°C (98.4.F), blood pressure is 110/80 mmHg, pulse is 60/min, and respirations are 18/min. S1 and S2 are normal, and an S4 is heard. The lungs are clear to auscultation. There is no jugular venous distension or pedal edema. Interventions to achieve which of the following goals would most improve this patient's long-term prognosis?
Decrease myocardial oxygen demand
Decrease blood coagulability
Restore coronary blood flow
Prevent ischemia-induced arrhythmias
Prevent reperfusin myocardial injury
A 64-year -old male with a history of hypertension presents with general malaise and a 'funny' heart rhythm for the past 2 weeks. He had an echocardiogram done last year, which revealed mild left atrial dilatation and left ventricular hypertrophy. He has been taking hydrochlorothiazide for hypertension. His blood pressure at today's visit is 180/98 mm Hg. An EKG is obtained and is shown below.

Which of the following is the most appropriate treatment for this patient?
Immediate cardioversion
Lidocaine
Adenosine
Carotid massage
Diltizem
A 64-year-old male is admitted in ICU for acute myocardial infarction. He is on metoprolol, lisinopril, aspirin, furosemide, and potassium supplements. All of a sudden, the nurse mentions that the patient has a change in his tele monitoring. His blood pressure is 120/60 mm Hg. His potassium level is 4.2. He is alert, awake and oriented time, place and person. Examination shows scattered bilateral crackles, peripheral pedal edema and elevated JVI.

Which of the following is the next best step in the management of this patient?
IV amiodarone
IV digoxin
Cardioversion
IV diltiazem
Carotid massage
A 34-year-old female presents to the ER with difficulty breathing and dizziness. Blood pressure tracing from an arterial line placed in the ER is depicted below.

Which of the following best accounts for these findings?
Severe asthma
Lobar pneumonia
Mitral stenosis
Aortic regurgitation
Panic attack
43-year -old man complains of progressive weakness and shortness of breath over the last two weeks. He denies any chest or muscle pain, nausea, vomiting or weight loss. He had a recent upper respiratory tract infection. His heart rate is 90/min and blood pressure is 110/70 mmHg. Jugular venous pressure is normal. Lungs are clear to auscultation. His chest x-ray is shown below.

Which of the following is the most likely additional finding in this patient?
Audible fourth heart sound
Non-palpable point of maximal impulse
Pulsus bisferiens
Opening snap
Fixed splitting of the second heart sound
A 55-year-old male is admitted to the ICU after being involved in a motor vehicle accident. He requires exploratory laparotomy for suspected bowel perforation. Two days after the surgery he remains hypotensive and requires both aggressive intravenous fluids and vasopressors to maintain his blood pressure. On physical examination, you note the fingertip changes pictured below:

All four extremities feel cold to touch. Which of the following is most likely responsible?
Septic emboli
Raynaud's phenomenon
Norepinephrine-induced vasospasm
Cholesterol emboli
Superior vena cava syndrome
{"name":"Picture USMLE", "url":"https://www.quiz-maker.com/QPREVIEW","txt":"A 43-year-old man presents to your office complaint of nagging left-side chest pain that increases on deep inspiration, plus two weeks of non-productive cough. He denies chills, fever or weight loss. His medical history is significant for Hodgkin's disease treated 20 years ago with chemotherapy and radiation therapy. On physical examination today, his blood pressure is 140\/90 mmHg and his heart rate is 90\/min.His chest x-ray is shown below. Which of the following is the most likely cause of his chest pain?, A 56-year-old woman is brought to the hospital from a local restaurant after suddenly becoming short of breath. Her flow-volume loop is shown below. Which of the following is the most likely cause of her symptoms?, A 54-year-old black male from the southeast USA presents to you with complaints of generalized malaise, fever, and a cough. He claims that he has had intermittent hemoptysis for the past six months. He denies smoking and has never had tuberculosis. Examination is unremarkable and his chest x-ray is shown below. On changing position, you notice that the part of the lesion seen on x-ray also moves. The most likely diagnosis is?","img":"https://www.quiz-maker.com/3012/images/ogquiz.png"}
More Quizzes
Green Mindset quiz
20100
Are you alpha
6321
Glamour Shot Contest
100
Qual o nome da raça?
100
Which Blackpink Member Are You? to Find Your Soulmate
201027919
Free PEMDAS Worksheets & Practice
201022778
Free Healthcare Infection Control Knowledge Test
201023689
Free Eligibility and Knowledge Assessment
201021641
Free: Best Conclusion from Data?
201023131
Intellectual Property Topics
15824282
Ultimate California Golden Bears Football Trivia
201043352
Free Radio Communication Code
201030132