Part 4 (765-865) (765-1019) NR 6
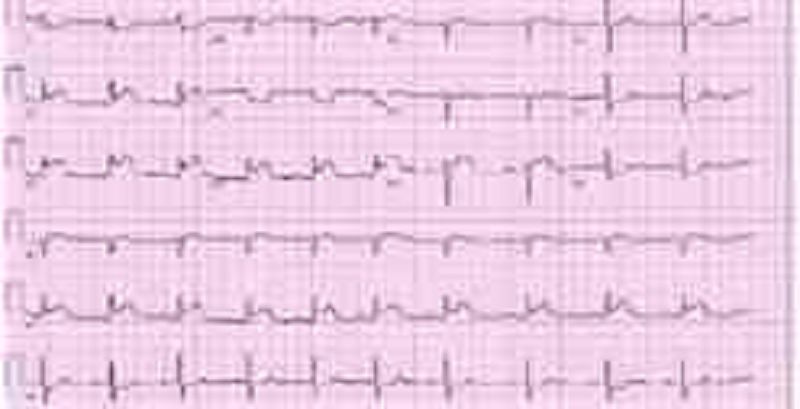
A 65-year -old Hispanic male is brought to the emergency room with severe substernal chest pain and diaphoresis that began suddenly 1 hour ago. He reports that his pain started while he was at rest and radiates to his left shoulder. The patient notes having vomited twice when the pain first began. Despite administration of 2 baby aspirins and 3 tablets of sublingual nitroglycerin, the pain persists. His initial EKG is shown below. On physical examination, the patient's temperature is 36.9°C (98.4°F), blood pressure is 110/80 mmHg, pulse is 60/min, and respirations are 18/min. S1 and S2 are normal, and an S4 is heard. The lungs are clear to auscultation. There is no jugular venous distension or pedal edema. Interventions to achieve which of the following goals would most improve this patient's long-term prognosis?
Restore coronary blood flow
Decrease myocardial oxygen demand
Decrease blood coagulability
Prevent ischemia-induced arrhythmias
Prevent reperfusin myocardial injury
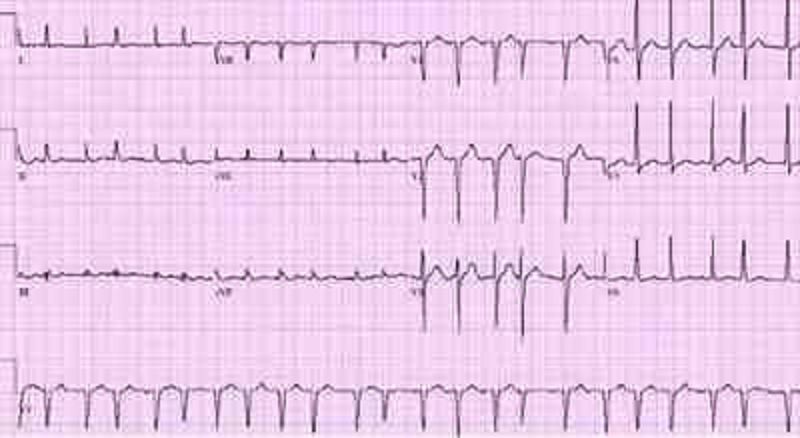
A 64-year -old male with a history of hypertension presents with general malaise and a 'funny' heart rhythm for the past 2 weeks. He had an echocardiogram done last year, which revealed mild left atrial dilatation and left ventricular hypertrophy. He has been taking hydrochlorothiazide for hypertension. His blood pressure at today's visit is 180/98 mmHg. An EKG is obtained and is shown below. Which of the following is the most appropriate treatment for this patient?
Diltizem
Immediate cardioversion
Lidocaine
Adenosine
Carotid massage
A 53-year-old Caucasian male is admitted to the hospital with a 2-week history of fatigue and decreased exercise tolerance. He says he can hardly climb two flights of stairs without getting dyspneic. He denies palpitations or chest pain. His past medical history is insignificant, and a routine check-up 6 months ago was normal. He admits two episodes of binge drinking during the last month, but says that he 'got it under control'. He is currently not taking any medications. His blood pressure is 150/90 mmHg and heart rate is 130/min, irregular. Lungs are clear on auscultation. ECG does not reveal P waves. Echocardiography shows significant left ventricular dilation with an ejection fraction of 35% and mitral regurgitation (1+). Which of the following intervention will most likely improve the left ventricular function in this patient?
Rate or rhythm control
Preload optimization
Decreasing afterload
Inotropic support
Valve surgery
A 47-year-old Caucasian female presents with occasional episodes of nocturnal substernal chest pain that wakes her up during sleep. The pain episodes last 15-20 minutes and resolve spontaneously. She denies any illicit drug use. She leads a sedentary lifestyle but states that she can climb two flights of stairs without any discomfort. She has no history of hypertension or diabetes. Her pulse is 75/min and regular, blood pressure is 134/70 mmHg and respirations are 14/min. Extended ambulatory ECG monitoring reveals transient ST segment elevation in leads I, aVL, and V4-V6 during the episodes. Which of the following is the best treatment for this patient?
Diltiazem
Propranolol
Aspirin
Heparin
Digoxin
A 55-year-old male presents to your office with a 6-month history of periodic substernal pressure. He experiences this pressure while walking uphill or climbing two flights of stairs. His past medical history is insignificant. He smokes 1 pack a day and consumes alcohol occasionally. His blood pressure is 160/90 mmHg and heart rate is 75/min. Resting ECG is normal. You suspect stable angina and order an ECG stress test that reveals horizontal ST segment depression in leads II, III, and aVF at submaximal heart rate. What is the best medication to treat this patient's condition?
Metoprolol
Thiazide
Verapamil
Amlodipine
Enalapril
A 56-year-old white male presents to his primary care physician for follow-up evaluation of high blood pressure noted on each of three prior visits over a period of 6 months (systolic blood pressure ranging 140-145, diastolic blood pressure ranging 90-96 mmHg). He has smoked a pack of cigarettes per day for the past 20 years and takes 5-6 drinks of alcohol daily. He has no other medical problems and takes no medications. There is no family history of diabetes mellitus, coronary artery disease, hyperlipidemia or hypertension. On physical examination today, his blood pressure is 146/97 mmHg and pulse is 80/min. The remainder of the exam is unremarkable. Which of the following nonpharmacologic interventions would be expected to have the greatest impact on his high blood pressure?
Decreased alcohol intake
Smoking cessation
Increased consumption of complex carbohydrates
Increased calcium consumption
. Decreased consumption of animal protein
A 63-year-old female presents to your office for a routine check-up. She has no present complaints. Her past medical history includes OM, type 2, and hypertension. Her current medications include glyburide and atenolol. She does not smoke. She drinks 2-3 glasses of wine 1-2 times a week. Three consecutive BP measurements were in the range of 138-142/87-90 mmHg. Physical examination is within normal limits. Her recent fasting glucose level was 250 mg/dl. ECG recorded 1 month ago showed left ventricular hypertrophy. Which statement about the BP control in this patient is the most accurate?
It is better to keep systolic pressure less than 130 mmHg to slow end-organ damage
BP is within acceptable range
BP is within optimal range
Diastolic BP is within acceptable range, but systolic is not
Systolic BP is within acceptable range, but diastolic is not
A 22-year-old white female is brought to your office by her mother because of the recurrent syncopal episodes. The first episode occurred about one year ago when her roommate committed suicide and then several similar episodes occurred usually provoked by a strong emotion. The episodes are preceded by light-headedness, weakness, and blurred vision and last about three minutes with rapid recovery of consciousness. Past medical history is insignificant. She is not taking any medications and denies drug abuse. Her blood pressure is 110/70 mmHg while supine and 108/70 mmHg while standing. Physical findings are within normal limits. EKG performed one month ago was normal. Which of the following is the next best step in the management of this patient?
Upright tilt table testing
Echocardiography
24-hour (Holter) monitoring
Electroencephalogram
Invasive electrophysiologic testing
A 59-year-old man presents to the emergency department (ED) complaining of new-onset chest pain that radiates to his left arm. He has a history of hypertension, hypercholesterolemia, and a 20-pack-year smoking history. His electrocardiogram (ECG) is remarkable for T-wave inversions in the lateral leads. Which of the following is the most appropriate next step in management?
Place the patient on a cardiac monitor, administer oxygen, and give aspirin
Give the patient two nitroglycerin tablets sublingually and observe if his chest pain resolves
Call the cardiac catheterization laboratory for immediate percutaneous coronary intervention (PCI)
Order a chest x-ray; administer aspirin, clopidogrel, and heparin
Start a β-blocker immediately
A 63-year-old insurance agent is brought to the ED by paramedics for shortness of breath and an RR of 31 breaths per minute. The patient denies chest pain, fever, vomiting, or diarrhea. His wife says he ran out of his “water pill” 1 week ago. His BP is 185/90 mmHg, HR is 101 beats per minute, oxygen saturation is 90% on room air, and temperature is 98.9°F. There are crackles midway up both lung fields and 2+ pitting edema midway up his legs. An ECG shows sinus tachycardia. The patient is sitting up and able to speak to you. After placing the patient on a monitor and inserting an IV, which of the following is the most appropriate next step in management?
Administer oxygen via non-rebreather, furosemide, nitroglycerin, and consider non-invasive respiratory therapy
Obtain blood cultures and complete blood cell (CBC) count, and begin empiric antibiotic therapy
Order a statim (STAT) portable chest x-ray
Administer oxygen via nasal cannula and have the patient chew an aspirin
Rapid sequence endotracheal intubation
You have been asked to evaluate a 42-year-old white male smoker who presented to the emergency department with sudden onset of crushing substernal chest pain, nausea, diaphoresis and shortness of breath. His initial ECG revealed ST segment elevation in the anterior-septal leads. Cardiac enzymes were normal. The patient underwent emergent cardiac catheterization, which revealed only a 25% stenosis of the left anterior descending (LAD) artery. No percutaneous intervention was performed. Which of the following interventions would most likely reduce his risk of similar episodes in the future?
Beginning therapy with a calcium-channel blocker
Placement of a percutaneous drug-eluting coronary artery stent
Placement of a percutaneous non-drug-eluting coronary artery stent
Beginning therapy with an ACE inhibitor
Beginning therapy with a beta-blocker
Two weeks after hospital discharge for documented myocardial infarction, a 65-year-old returns to your office concerned about low-grade fever and pleuritic chest pain. There is no associated shortness of breath. Lungs are clear to auscultation and the heart is free of murmur, gallop, or rub. ECG is unchanged from the last one in the hospital. Which therapy is most likely to be effective?
An anti-inflammatory agent
Antibiotics
Anticoagulation with warfarin (Coumadin)
An increase in antianginal medication
An anxiolytic agent
A 55-year-old patient presents to you after a 3-day hospital stay for gradually increasing shortness of breath and leg swelling while away on a business trip. He was told that he had congestive heart failure, but is asymptomatic now, with normal vital signs and physical examination. An echocardiogram shows an estimated ejection fraction of 38%. The patient likes to keep medications to a minimum. He is currently on aspirin and simvastatin. Which would be the most appropriate additional treatment?
Begin an ACE inhibitor and then add a beta-blocker on a scheduled basis
Begin digoxin plus furosemide on a scheduled basis
Begin spironolactone on a scheduled basis
Begin furosemide plus nitroglycerin
Given his preferences, no other medication is needed unless shortness of breath and swelling recur
An active 78-year-old female with history of hypertension presents with the new onset of left hemiparesis. Cardiac monitoring reveals atrial fibrillation. She had been in sinus rhythm on check-up 3 months earlier. Optimal management at discharge includes a review of antihypertensive therapy, a ventricular rate control agent, and which of the following?
Warfarin with a target INR of 2.0 to 3.0.
Automated implanted cardioverter-defibrillator (AICD)/permanent pacemaker to avoid the need for anticoagulation
Immediate direct-current cardioversion
Antiplatelet therapy such as aspirin, without warfarin
Antiplatelet therapy plus warfarin with a target INR of 1.5
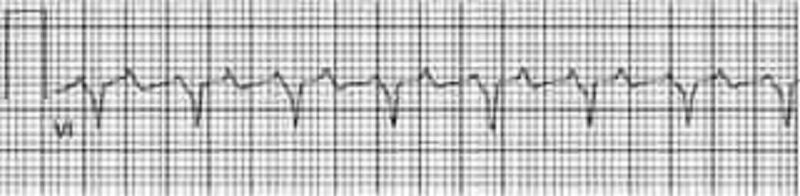
A 72-year-old male with a history of poorly controlled hypertension develops a viral upper respiratory infection. On his second day of symptoms he experiences palpitations and presents to the emergency room. His blood pressure is 118/78 mmHg. The following rhythm strip is obtained. What is the best next step in the management of this patient?
Administration of intravenous metoprolol
Administration of intravenous adenosine
Administration of intravenous amiodarone
Emergent electrical cardioversion
Initiation of chest compressions and preparation for semielective intubation
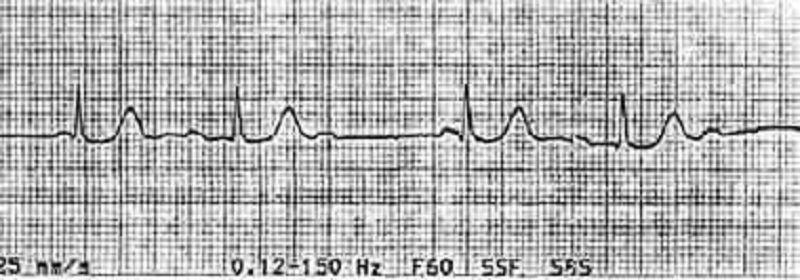
An otherwise asymptomatic 65-year-old man with diabetes presents to the ER with a sports-related right shoulder injury. His heart rate is noted to be irregular, and this ECG is obtained. Which of the following is the best immediate therapy?
Observation
Atropine
Isoproterenol
Pacemaker placement
Electrical cardioversion
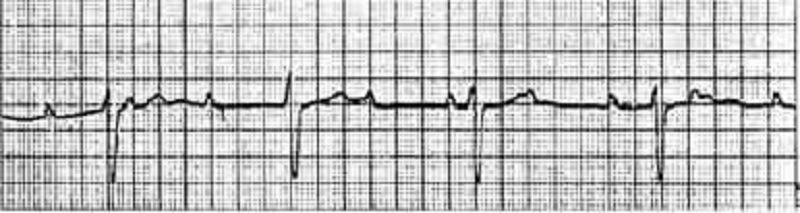
A patient has been in the coronary care unit for the past 24 hours with an acute anterior myocardial infarction. He develops the abnormal rhythm shown below, although blood pressure remains stable at 110/68 mmHg. Which of the following is the best next step in therapy?
Arrange for pacemaker placement
Perform cardioversion
Give digoxin
Give propranolol
Give lidocaine
A 70-year-old male with a history of coronary artery disease presents to the emergency department with 2 hours of substernal chest pressure, diaphoresis, and nausea. He reports difficulty “catching his breath.” An electrocardiogram shows septal T-wave inversion. The patient is given 325-mg aspirin and sublingual nitroglycerin while awaiting the results of his blood work. His troponin I is 0.65 ng/mL (normal < 0.04 ng/mL). The physician in the emergency department starts the patient on low-molecular-weight heparin. His pain is 3/10. Blood pressure is currently 154/78 mmHg and heart rate is 72. You are asked to assume care of this patient. What is the best next step in management?
Begin intravenous beta-blocker therapy
Arrange for emergent cardiac catheterization
Begin intravenous thrombolytic therapy
Admit the patient to a monitored cardiac bed and repeat cardiac enzymes and ECG in 6 hours
Begin clopidogrel 300 mg po each day
You are volunteering with a dental colleague in a community indigent clinic. A nurse has prepared a list of patients who are scheduled for a dental procedure and may need antibiotic prophylaxis beforehand. Of the patients listed below, who would be most likely to benefit from antibiotic prophylaxis to prevent infective endocarditis?
65-year-old male with prosthetic aortic valve
17-year-old male with coarctation of the aorta
26-year-old female with a ventricular septal defect repaired in childhood
42-year-old female with mitral valve prolapse
72-year-old female with aortic stenosis
An 80-year-old woman was admitted to your service for dizziness. Cardiac monitoring initially revealed atrial fibrillation with rapid ventricular response. Her ventricular rate was controlled with beta-blocker. An echocardiogram revealed an enlarged left atrium and an ejection fraction of 50%. No evidence of diastolic heart dysfunction was noted. She is now asymptomatic, with blood pressure 130/80 mmHg, heart rhythm irregularly irregular, and heart rate around 80/minute. Which of the following is the best management strategy of this patient’s arrhythmia?
Continued rate control plus prolonged anticoagulation
Electrical cardioversion plus prolonged anticoagulation
Electrical cardioversion without anticoagulation
Chemical cardioversion plus prolonged anticoagulation
Chemical cardioversion without anticoagulation
You are seeing a 45-year-old female patient of your partner for the first time in your clinic. A quick review of the patient’s medical record shows that her systolic blood pressure was greater than 140 mmHg at both of her last clinic appointments. Her medical history is otherwise significant only for diabetes mellitus. Her blood pressure today is 164/92 mmHg. What is the best next step in her blood pressure management?
Prescribe an ACE inhibitor in addition to heart healthy diet
Ask the patient to keep a written record of her blood pressure and bring with her to a return appointment
Advise the patient to begin a heart healthy, low sodium diet and refer to a nutritionist
Prescribe a dihydropyridine calcium-channel blocker in addition to a heart healthy diet
Arrange for echocardiogram to assess for end-organ damage
A 68-year-old male complains of pain in his calves while walking. He notes bilateral foot pain, which awakens him at night. His blood pressure is 117/68 mmHg. Physical examination reveals diminished bilateral lower extremity pulses. An ankle:brachial index measures 0.6. The patient’s current medications include aspirin and hydrochlorothiazide. Which of the following is the best initial management plan for this patient’s complaint?
Smoking cessation therapy, graduated exercise regimen, cilostazol
Smoking cessation therapy, warfarin
Smoking cessation therapy, schedule an arteriogram
Smoking cessation therapy, warfarin, peripherally acting calcium-channel blocker
Smoking cessation therapy, consultation with a vascular surgeon
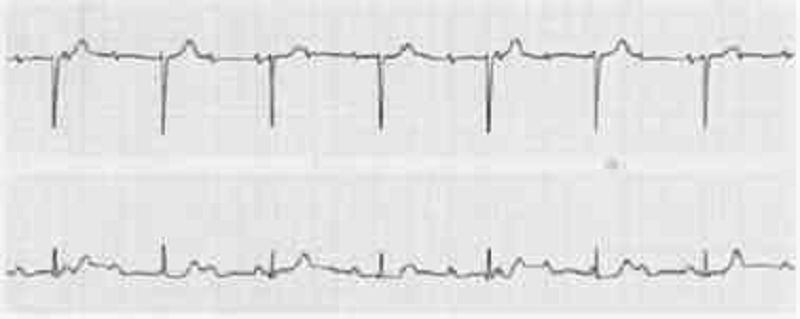
An 82-year-old woman is brought to the ED by her daughter for worsening fatigue, dizziness, and light-headedness. The patient denies chest pain or shortness of breath. She has not started any new medications. Her BP is 140/70 mmHg, HR is 37 beats per minute, and RR is 15 breaths per minute. An IV is started and blood is drawn. An ECG is seen below. Which of the following is the most appropriate next step in management?
Place on a cardiac monitor, place external pacing pads on the patient, and admit to the CCU
Bed rest for the next 48 hours and follow-up with her primary-care physician
Administer aspirin, order a set of cardiac enzymes, and admit to the cardiac care unit (CCU)
Place a magnet on her chest to turn off her pacemaker
Admit for Holter monitoring and echocardiogram
A 52-year-old man presents to his primary care physician’s office for routine care. He has hypertension, hypercholesterolemia, and type 2 diabetes mellitus, and has smoked one pack of cigarettes per day for the past 30 years. Medications include hydrochlorothiazide, atorvastatin, and glipizide. There is a family history of myocardial infarction in the maternal grandfather at age 60. The patient has undergone screening for colon and prostate cancer. Physical examination reveals a pleasant, obese man who is 175 cm (5′9″) tall and weighs 108 kg (238 lb). His blood pressure is 155/81 mmHg, heart rate is 78/min, respiratory rate is 14/min, and temperature is 36.8°C (98.3°F). What one action would most reduce the patient’s stroke risk?
Blood pressure reduction
Blood glucose reduction
Serum cholesterol reduction
Smoking cessation
Weight loss
A 29-year-old tall, thin man presents to the ED after feeling short of breath for 2 days. In the ED, he is in no acute distress. His BP is 115/70 mmHg, HR is 81 beats per minute, RR is 16 breaths per minute, and oxygen saturation is 98% on room air. Cardiac, lung, and abdominal examinations are normal. An ECG reveals sinus rhythm at a rate of 79. A chest radiograph shows a small right-sided (< 10% of the hemithorax) spontaneous pneumothorax. A repeat chest x-ray 6 hours later reveals a decreased pneumothorax. Which of the following is the most appropriate next step in management?
Discharge the patient with follow-up in 24 hours
Perform needle decompression in the second intercostal space, midclavicular line
Insert a 20F chest tube into right hemithorax
Observe for another 6 hours
Admit for pleurodesis
A 47-year-old man with a history of hypertension presents to the ED complaining of continuous left-sided chest pain that began while snorting cocaine 1 hour ago. The patient states he never experienced chest pain in the past when using cocaine. His BP is 170/90 mmHg, HR is 101 beats per minute, RR is 18 breaths per minute, and oxygen saturation is 98% on room air. The patient states that the only medication he takes is alprazolam to “calm his nerves.” Which of the following medications is contraindicated in this patient?
Metoprolol
Diltiazem
Aspirin
Lorazepam
Nitroglycerin
A 60-year-old man with coronary artery disease, peptic ulcer disease, and gout presents to the emergency department with a 24-hour history of abdominal pain. The pain, which is most intense in the upper abdomen, was sudden in onset and has become progressively more severe. Free air in the abdomen is detected on x-ray films. The patient is in an agitated state. His extremities are cool and capillary refill time is 3 seconds. His blood pressure is 80/40 mmHg and heart rate is 130/min. The neck veins are flat and the lungs are clear to auscultation. His hemoglobin is 13.8 g/dL. A urinary catheter is inserted and 10 mL of urine is drained. What is the most appropriate treatment for this patient at this time?
Infusion of isotonic fluid
Broad-spectrum antibiotics for presumed sepsis
Infusion of norepinephrine
Inotropic support with dopamine, vasopressin, or dobutamine
Transfuse with 1 unit packed RBCs
A 19-year-old man complains of chest pain while playing basketball on his high school team. Paramedics are called and he is rushed to the hospital. Physical examination reveals moderate mitral regurgitation and a crescendodecrescendo systolic ejection murmur that gets louder with Valsalva maneuver. Echocardiography reveals thickened left ventricular walls and dynamic left ventricular outflow tract obstruction. What is the best first step in management?
β-Blockers
Calcium channel blockers
Partial excision of the interventricular septum
Warfarin
Digoxin
A 57-year-old man presents to the emergency department with worsening substernal chest pain occurring over the past 20 minutes. He has a medical history significant for a 2-packper- day smoking history, gout, obesity, hypercholesterolemia, hypertension, osteoarthritis of both knees, inflammatory bowel disease, and recently diagnosed type 2 diabetes mellitus that is well controlled on oral antiglycemics (haemoglobin A1c of 7.8%). On physical examination he is in moderate distress, diaphoretic, and nauseous. His temperature is 37.5°C (99.5°F), pulse is 112/min, blood pressure is 142/85 mmHg, and respiratory rate is 22/min. He tests positive for MI by serial cardiac enzymes. He is started on the appropriate therapy and is ready for discharge the following evening. What is the number one preventive measure this patient can take to decrease his immediate risk for a second MI?
Quit smoking
Decrease the amount of cholesterol in his diet
Exercise three times a week
Lower his blood pressure to the 120/80 mm Hg range
Lower his blood sugar levels to achieve a hemoglobin A1c level <7%
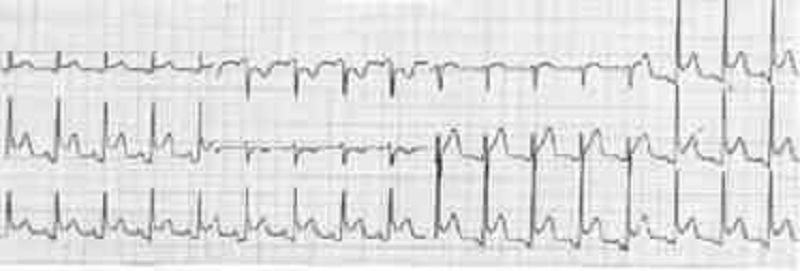
A 31-year-old kindergarten teacher presents to the ED complaining of acute-onset substernal chest pain that is sharp in nature and radiates to her back. The pain is worse when she is lying down on the stretcher and improves when she sits up. She smokes cigarettes occasionally and was told she has borderline diabetes. She denies any recent surgeries or long travel. Her BP is 145/85 mmHg, HR is 99 beats per minute, RR is 18 breaths per minute, and temperature is 100.6°F. Examination of her chest reveals clear lungs and a friction rub. Her abdomen is soft and nontender to palpation. Her legs are not swollen. Chest radiography and echocardiography are unremarkable. Her ECG is shown below. Which of the following is the most appropriate next step in management?
Prescribe a NSAID and discharge the patient
Anticoagulate and CT scan to evaluate for a PE
Aspirin, heparin, clopidogrel, and admit for ACS
Administer thrombolytics if the pain persists
Prescribe antibiotics and discharge the patient
A 51-year-old woman presents to the ED after 5 consecutive days of crushing substernal chest pressure that woke her up from sleep in the morning. The pain resolves spontaneously after 20 to 30 minutes. She is an avid rock climber and jogs 5 miles daily. She has never smoked cigarettes and has no family history of coronary disease. In the ED, she experiences another episode of chest pain. An ECG reveals ST-segment elevations and cardiac biomarkers are negative. The pain is relieved with sublingual nitroglycerin. She is admitted to the hospital and diagnostic testing reveals minimal coronary atherosclerotic disease. Which of the following is the most appropriate medication to treat this patient’s condition?
Calcium channel blocker (CCB)
Aspirin
β-Blocker
H2-Blocker
Antidepressant
While discussing a case presentation with a medical student, a nearby patient who just returned from getting an ankle radiograph done yells out in pain. You walk over to him and ask what is wrong. He states that since returning from the radiology suite, his automatic implantable cardioverter defibrillator (AICD) is discharging. You hook him up to the monitor and note that his rhythm is sinus. You observe a third shock while the patient is in sinus rhythm. Which of the following is the most appropriate next step in management?
Place a magnet over the AICD generator to inactivate it and thereby prevent further shocks
Send the patient back to the radiology suite for another radiograph to desensitize his AICD
Administer pain medication and wait until the device representative arrives at the hospital to power off the AICD
Admit the patient to the telemetry unit to monitor his rhythm and find the cause of his AICD discharge
Make a small incision over his chest wall and remove the AICD generator and leads
A 22-year-old primagravida woman develops hypertension at 28 weeks. She is asymptomatic and the examination is normal except for 1+ pedal edema. Her complete blood count, liver enzymes, and electrolytes are normal. The urinalysis is positive for proteinuria. Which of the following is true for this type of hypertension?
Should be controlled with medications
Improves in the third trimester
Leads to large-birth-weight babies
Spares the placenta
Spares maternal kidney function
A 61-year-old man has a non-ST-elevation MI and is admitted to the coronary care unit. The following day, he develops bradycardia but no symptoms. His blood pressure is 126/84 mmHg, pulse 50/min, and on examination, the heart sounds are normal, with no extra sounds or rubs. His ECG has changed. Which of the following ECG findings is the best indication for this patient to receive a pacemaker?
Left bundle branch block (LBBB) and second-degree AV block Mobitz type II
Persistent bradycardia
Second-degree AV block Mobitz type I
First-degree AV block
New right bundle branch block
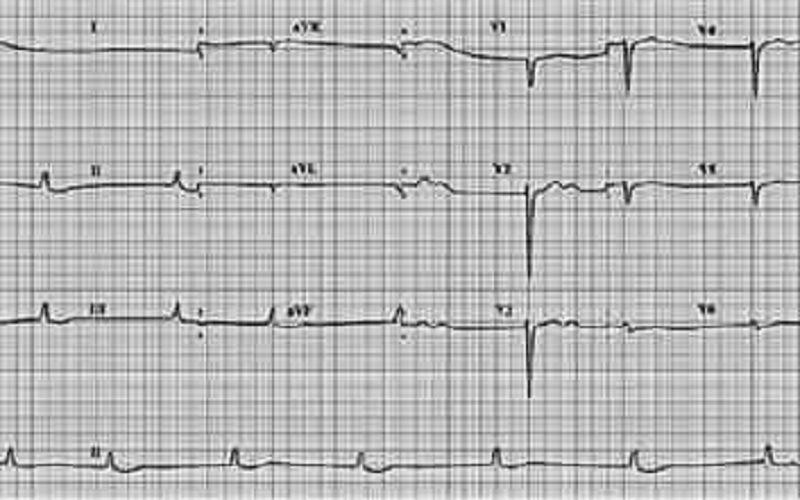
A 63-year-old woman on digitalis for chronic atrial fibrillation experiences fatigue, nausea, and anorexia. Her pulse is regular at 50 beats/min, and the heart sounds, chest, and abdominal examinations are normal. On the ECG, no P waves are visible and the QRS complexes are narrow and regular. Which of the following is the most appropriate management step?
Complete cessation of digitalis
An increase in digitalis dose
Withdrawal of digitalis for one dose
Addition of a beta-blocker
Addition of a calcium channel blocker
A 26-year-old white nonsmoking woman returns for a follow-up appointment with her primary care provider. At a routine health maintenance visit 8 months earlier, her blood pressure was 179/97 mmHg. Since then she has adhered to a low-fat diet and exercises regularly. On repeat measurement 1 month later, her blood pressure was still elevated, despite her compliance with the prescribed hydrochlorothiazide and lisinopril. She has no complaints and denies headaches, chest pain, or mental status changes. On physical examination she is a slender woman in no apparent distress. An abdominal bruit that lateralizes to the left is heard. Her blood pressure is 178/99 mmHg in her left arm and 181/95 mmHg in her right arm. A basic metabolic panel and complete blood count are within normal range. Which of the following is the most appropriate next step in patient care?
Order duplex imaging of the renal arteries and proceed to percutaneous transluminal angioplasty if renal artery stenosis is found
Add a statin to the patient’s current drug regimen to decrease fatty arterial plaques
Admit patient to the hospital and start intravenous nitroprusside
Increase the dosage of her antihypertensive regimen
Order duplex imaging of the renal arteries and proceed to surgical revascularization if renal artery stenosis is found
A 58-year-old man is admitted to the coronary care unit for telemetric monitoring after an episode of bradycardia. While in the unit, he suddenly loses consciousness. His pulse is undetectable and his blood pressure drops to 40 mmHg. His airway is clear and patent, and he is still breathing on his own. An ECG shows electrical activity. Chest compressions are started and he is quickly given a bolus of intravenous sodium bicarbonate and atropine. When his tracing does not improve, the boluses are repeated twice, and finally his tracing returns to normal sinus rhythm. Moments later, when he regains consciousness, he complains of a dry mouth, blurred vision, and feeling flushed. What is the most appropriate next step in the management of this patient?
This patient is experiencing transient adverse effects of atropine and requires only supportive measures
This patient has atropine toxicity and requires urgent administration of a cholinergic agonist
This patient has atropine toxicity and requires urgent administration of a muscarinic agonist
This patient has bicarbonate toxicity and requires urgent administration of calcium citrate
This patient is experiencing transient adverse effects of bicarbonate and requires only supportive measures
A 2-year-old girl is referred to the hospital for evaluation of her inability to gain weight. She is well fed by her parents, but appears to tire during feedings and has been losing weight despite frequent high-calorie meals. There is no family history of developmental delay or short stature. She is well dressed, her hair is brushed, and she is playful but tires quickly. Her temperature is 36.5°C (97.7°F), pulse is 110/min, blood pressure is 90/50 mmHg, and respiratory rate is 24/min. She has a harsh 2/6 holosystolic murmur that is best heard at the left sternal border, which is unchanged and has been present since birth. Which of the following is the most appropriate next step in management?
Refer for evaluation and possible closure of ventricular septal defect
Continue to monitor the patient for increased weight loss and increased shunting
PH probe for gastroesophageal refl ux disease
Skeletal survey
Stool culture
A 31-year-old man who works for a moving company presents to the ED because he thinks he was having a heart attack. He does not smoke, and jogs 3 days a week. His father died of a heart attack in his sixties. He describes a gradual onset of chest pain that is worse with activity and resolves when he is at rest. His HR is 68 beats per minute, BP is 120/70 mmHg, and RR is 14 breaths per minute. On examination, his lungs are clear and there is no cardiac murmur. You palpate tenderness over the left sternal border at the third and fourth ribs. An ECG reveals sinus rhythm at a rate of 65. A chest radiograph shows no infiltrates or pneumothorax. Which of the following is the most appropriate next step in management?
Administer ibuprofen and reassure the patient that he is not having a heart attack
Administer aspirin and send for a troponin
Administer aspirin, clopidogrel, and heparin, and admit for acute coronary syndrome (ACS)
Inject corticosteroid into the costochondral joint to reduce inflammation
Observe the patient for 6 hours
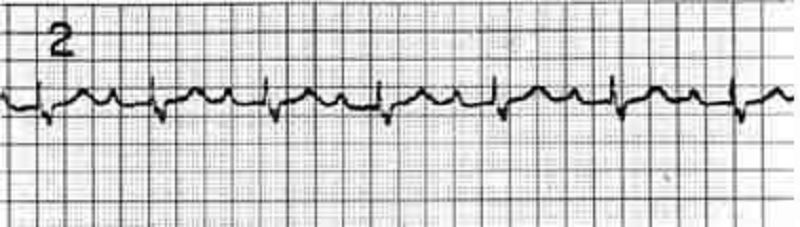
A 27-year-old man who is otherwise healthy presents to the ED with a laceration on his thumb that he sustained while cutting a bagel. You irrigate and repair the wound and are about to discharge the patient when he asks you if he can receive an ECG. It is not busy in the ED so you perform the ECG, as seen below. Which of the following is the most appropriate next step in management?
Discharge the patient home
Admit the patient for placement of a pacemaker
Admit the patient for a 24-hour observation period
Administer aspirin and send cardiac biomarkers
Repeat the ECG because of incorrect lead placement
A 56-year-old woman was recently started on medication for high blood pressure. At her next office visit her hypertension is under good control, but she now complains of “feeling strange” since she started the medication. On further questioning, she reports feeling chest tightness several times over the past 2 weeks, and has also noticed pain in her elbows and knees. Her blood pressure is 124/78 mmHg (146/82 mmHg on last visit), heart rate is 102/min, and respiratory rate is 14/min. Her examination is notable for several erythematous plaques on the malar distribution of the face, arms, and upper torso. What medication was she most likely started on during her last visit?
Hydralazine
Captopril
Metoprolol
Verapamil
Furosemide
A 34-year-old woman presents to your office complaining of several months of chest pain. She says that the pain is left-sided, does not change with deep inspiration, and typically lasts several hours. The pain has no relation to physical activity, but worsens with emotional stress. The patient has no significant family history, and does not use tobacco, alcohol or drugs. She takes no medications and has no drug allergies. On exam, her blood pressure is 110/70 mmHg and her heart rate is 78/min. ECG is normal. Which of the following is the best next step in her management?
Reassurance
Stress ECG testing
Transthoracic echocardiography
Lower extremity venous ultrasonography
Chest X-ray
A 60-year-old male patient is receiving aspirin, an angiotensin-converting enzyme inhibitor, nitrates, and a beta-blocker for chronic stable angina. He presents to the ER with an episode of more severe and long-lasting angina chest pain each day over the past 3 days. His ECG and cardiac enzymes are normal. Which of the following is the best course of action?
Admit the patient and begin low-molecular-weight heparin
Admit the patient and add intravenous digoxin
Admit the patient for thrombolytic therapy
Admit the patient for observation with no change in medication
Increase the doses of current medications and follow closely as an outpatient
A 42-year-old man presents to the clinic for routine evaluation. His medical history is signified cant for gallstones. The patient denies smoking and drinks alcohol occasionally. His mother had a heart attack at the age of 63 years. His blood pressure is 134/77 mmHg. The patient is overweight with well-healed laparoscopic cholecystectomy scars. Fasting laboratory tests show: Aspartate aminotransferase: 37 U/L, Alanine aminotransferase: 28 U/L, Alkaline phosphatase: 88 U/L, Total cholesterol: 268 mg/dL, LDL cholesterol: 183 mg/dL, HDL cholesterol: 46 mg/dL, Triglycerides: 166 mg/dL. What is the most appropriate next step in management?
A trial of lifestyle modification alone (diet, exercise, and weight loss)
A trial of lifestyle modification combined with statin and niacin therapy
A trial of lifestyle modification combined with statin therapy
Niacin therapy
Statin therapy
A 60-year-old man with a history of congestive heart failure presents to his physician. He has a 5-year history of excessive daytime sleepiness and snoring. He also admits to three drinks of alcohol per day. His temperature is 36.6°C (98.0°F), pulse is 85/min, blood pressure is 138/82 mmHg, respiratory rate is 14/min, and oxygen saturation is 99% on room air. His body mass index is 31 kg/m2. Physical examination is significant for macroglossia and a short neck. Polysomnography is performed and is significant for multiple nocturnal episodes of airflow cessation at the nose and mouth, despite evidence of continuing respiratory effort. Which of the following is the most effective management for this patient?
Nasal continuous positive airway pressure
Avoidance of alcohol
Avoidance of supine posture
Uvulopalatopharyngoplasty
Weight reduction
During a screening physical examination for participating in high school sports, a 14-yearold girl is found to have a late apical systolic murmur preceded by a click. The rest of the examination is unremarkable. Echocardiography shows superior displacement of the mitral leaflets of > 2 mm during systole into the left atrium, with a thickness of at least 8 mm. In addition, she states that her father also has some type of heart “murmur,” but she knows nothing else about it. Which of the following is the most appropriate management at this time?
Prophylactic antibiotics for dental procedures
Digoxin
Instruct the patient to avoid all forms of strenuous activity
Metoprolol
Mitral valve replacement
A 27-year-old man complains of chest palpitations and light-headedness for the past hour. He has no past medical history and is not taking any medications. He drinks a beer occasionally on the weekend and does not smoke cigarettes. His HR is 180 beats per minute, BP is 110/65 mmHg, and oxygen saturation is 99% on room air. An ECG reveals an HR of 180 beats per minute with a QRS complex of 90 milliseconds with a regular rhythm. There are no discernable P waves. Which of the following is the most appropriate medication to treat this dysrhythmia?
Adenosine
Digoxin
Lidocaine
Amiodarone
Bretylium
A 70-year-old female has been healthy except for hypertension treated with a thiazide diuretic. She presents with sudden onset of a severe, tearing chest pain, which radiates to the back and is associated with dyspnea and diaphoresis. Blood pressure is 210/94 mmHg. Lung auscultation reveals bilateral basilar rales. A faint murmur of aortic insufficiency is heard. The BNP level is elevated at 550 pg/mL (Normal < 100). ECG shows nonspecific ST-T changes. Chest x-ray suggests a widened mediastinum. Which of the following choices represents the best initial management?
IV beta-blocker to control heart rate, IV nitroprusside to control blood pressure, transesophageal echocardiogram
IV furosemide plus IV loading dose of digoxin
Percutaneous coronary intervention with consideration of angioplasty and/or stenting
Blood cultures and rapid initiation of vancomycin plus gentamicin, followed by echocardiography
IV heparin followed by CT pulmonary angiography
A 67-year-old homeless male presents 24 hours after the onset of substernal chest pain and is diagnosed with an anterior wall myocardial infarction. There is no history of previous chest pain, dyspnea, palpitations, syncope or leg swelling. He has no hypertension or diabetes mellitus. He does acknowledge a 40 pack-year smoking history. Upon discharge, echocardiography shows normal left ventricular size, left ventricular anterior wall hypokinesis and an ejection fraction of 50%. Two years later, the patient is found dead in the street. Autopsy reveals a dilated left ventricle with a globular shape and thinned walls along with a scar on the anterior wall. Which of the following would have most likely prevented this patient's pathologic findings?
Enalapril
Aspirin
Amlodipine
Isosorbide dinitrate
Digoxin
A 55-year-old white male presents to the Emergency Room with a four-hour history of chest pain. The pain is substernal and radiates to the left arm. He has a history of hypertension, diabetes, and hypercholesterolemia. His temperature is 36.7°C (98°F), blood pressure is 110/65 mmHg, pulse is 110/min, and respirations are 18/min. ECG is recorded and reveals ST segment elevation in the anterior leads and several ventricular premature beats (VPBs). What would the administration of lidocaine to such a patient most likely result in?
Increase in the risk of asystole
Increase in the risk of ventricular fibrillation
Improvement in overall prognosis
No change in frequency of VPBs
Increase in the risk of congestive heart failure
56-year-old man presents to your office complaining of progressively worsening fatigue. He also reports difficulty concentrating and increasing forgetfulness over the past several weeks. On review of systems, the patient reports having unintentionally gained 6 pounds over the last three months. His past medical history is significant for hypertension and atrial fibrillation. On physical examination, he has a blood pressure of 140/90 mmHg and a heart rate of 75/min. His lung fields are clear to auscultation. There is no ankle edema. His skin is dry. Which of the following drugs is most likely responsible for this patient's complaints?
Amiodarone
Enalapril
Verapamil
Metoprolol
Hydralazine
An 83-year-old woman is being evaluated for confusion. She was admitted 3 days ago after having an acute MI. Her hospital course has been complicated by narrow-complex ventricular tachycardia, which has finally been stabilized on an antiarrhythmic medication. She was also started on a post-MI protocol and an antidepressant. One day after beginning these medications, she begins to develop confusion and slurred speech. Her temperature is 36.7°C (98.1°F), blood pressure is 138/60 mmHg, pulse is 88/min, and respiratory rate is 14/min. She is alert and oriented to person, but she does not realize she is in the hospital. Additionally, she exhibits difficulty with word articulation, although she speaks fluently, and she demonstrates a mild resting tremor. The remainder of her examination is normal. Which of the following medications is most likely to cause these central nervous system effects?
Lidocaine
Aspirin
Enalapril
Fluoxetine
Metoprolol
A 62-year-old man with a history of benign prostatic hyperplasia and hypertension presents to his primary care provider for a routine health maintenance visit. He reports that he feels “better than ever” and explains that his daughter made him come in for his annual visit. He takes prazosin daily and occasionally some acetaminophen. He has no drug allergies and denies smoking, drinking, or the use of illicit drugs. His physical examination is within normal range except for his rectal examination, which revealed an enlarged prostate. His temperature is 36.8°C (98.2°F), respiratory rate is 13/min, pulse is 82/min, and blood pressure is 138/86 mmHg. Which of the following is the most likely adverse effect of α1-adrenergic blockade in this patient?
Orthostatic hypotension
Decreased urine flow
Increased blood pressure
Increased sexual drive
Irritability
A 59-year-old man presents to the ED with left-sided chest pain and shortness of breath that began 2 hours prior to arrival. He states the pain is pressure-like and radiates down his left arm. He is diaphoretic. His BP is 160/80 mmHg, HR 86 beats per minute, and RR 15 breaths per minute. ECG reveals 2-mm ST-segment elevation in leads I, aVL, and V 3 to V 6. Which of the following is an absolute contraindication to receiving thrombolytic therapy?
Previous hemorrhagic stroke
Systolic BP (SBP) greater than 180 mm Hg
Patient on Coumadin and aspirin
Total hip replacement 3 months ago
Peptic ulcer disease
A 55-year-old man presents to the ED at 2:00 AM with left-sided chest pain that radiates down his left arm. He takes a β-blocker for hypertension, a proton pump inhibitor for gastroesophageal reflux disease, and an antilipid agent for high cholesterol. He also took sildenafil the previous night for erectile dysfunction. His BP is 130/70 mmHg and HR is 77 beats per minute. Which of the following medications is contraindicated in this patient?
Nitroglycerin
Aspirin
Unfractionated heparin
Metoprolol
Morphine sulphate
A 62-year-old woman presents to the ED with general weakness, shortness of breath, and substernal chest pain that radiates to her left shoulder. Her BP is 155/80 mmHg, HR is 92 beats per minute, and RR is 16 breaths per minute. You suspect that she is having an acute MI. Which of the following therapeutic agents has been shown to independently reduce mortality in the setting of an acute MI?
Aspirin
Nitroglycerin
Unfractionated heparin
Lidocaine
Diltiazem
A 62-year-old woman comes to the office for evaluation of a pigmented lesion on her left forearm. The lesion occasionally itches but is otherwise asymptomatic. She admits that she only came because her daughter had persuaded her to do so. On examination, there is a slightly elevated, brown-colored lesion measuring 7 mm in diameter with irregular borders. What is the best next step in management?
Excisional biopsy
Shave biopsy
Dermoscopy
Excision with 1 cm margins
Incisional biopsy
A 17-year-old white male presents to your office because the "spots" on his face "got so much worse recently!" He has several months history of acne. He has not visited a doctor before. Inspection reveals multiple papules with several pustules and nodules. Atrophic scars are seen. What is the best next step in the management of this patient?
Oral isotretinoin
Topical retinoids
Topical antibiotic
Oral antibiotic
Benzyl peroxide
A 47-year-old woman presents to your office complaining of two days of pain and itching over her left chest. Her medical history is significant for breast cancer for which she underwent a left-sided mastectomy six months ago. She has also been receiving chemotherapy and radiation. Physical examination reveals erythema around the mastectomy scar, with excoriations and occasional vesicles. Which of the following is the best treatment for her condition?
Acyclovir
Topical 5-fluorouracil
Topical corticosteroids
Mupirocin
Fluconazole
A 34-year-old Caucasian female presents to the ER with a rash and pruritis. She says that she has had a sore throat for several days, and her friend gave her amoxicillin that turned out to be out dated. The rash developed about 30 minutes after she took the drug. Her blood pressure is 110/70 mmHg and heart rate is 80/min. Physical examination reveals wide spread urticaria and excoriations. Pharyngeal mucosa and tonsils are hyperemic, and tender lymph nodes are palpated in the submandibular area. Lungs are clear on auscultation. Which of the following is the best next step in the management of this patient?
Prescribe antihistamines
Continue amoxicillin therapy with non-outdated drug
Administer adrenalin immediately
Prescribe steroids
Schedule for dialysis
A 35-year-old white male presents with high-grade fever, chills, rigors, malaise, and pain in his right calf for the last 24 hours. His temperature is 39.5°C (103.1°F), pulse is 105/min, blood pressure is 130/80 mmHg, and respirations are 15/min. Physical examination shows generalized swelling of the calf with linear streaks of erythema. The lesion is warm, tender, and not very well-demarcated. No pain is felt in the calf when the ankle is dorsiflexed. Scaling is found in the toe webs on the right side, and KOH preparation of these lesions show hyphae. Blood cultures are obtained. CBC shows a WBC count of 14,000 with 6% bands. What is the most appropriate next step in management?
Intravenous nafcillin
Oral itraconazole
Oral terbinafine
Oral dicloxacillin
Intravenous crystalline penicillin G
A 14-year-old white female presents with "spots" on her face that are "so embarrassing!" Physical examination reveals comedones with minimal inflammation. Her past medical history is insignificant. She does not smoke or consume alcohol. What is the best next step in the management of this patient?
Topical retinoids
Dietary modifications
Cream-based cleansers
Topical erythromycin
Oral doxycycline
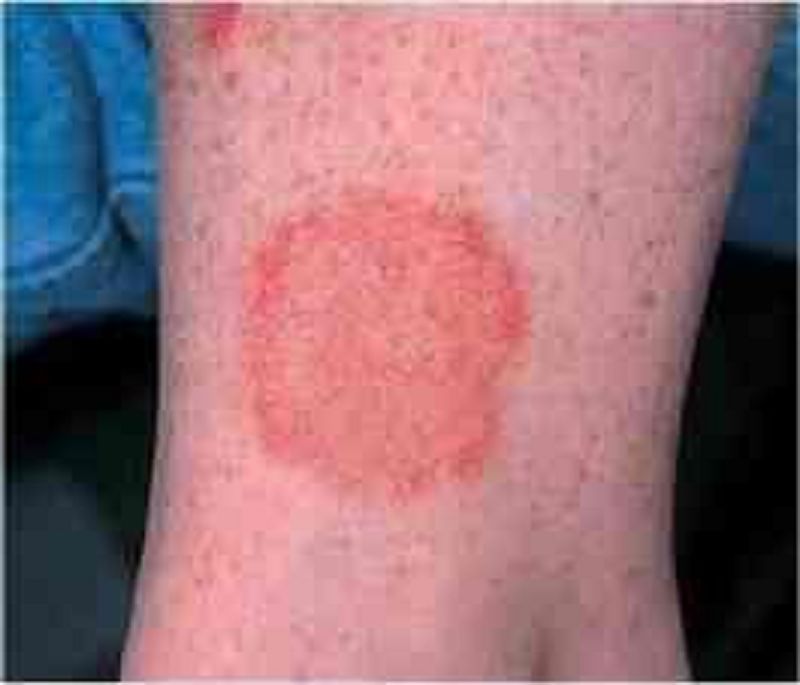
A 12-year-old boy notices a scaly, mildly pruritic rash on his arm (see image below). There is no associated fever, muscle pain, nausea, vomiting, diarrhea, or back pain. He recently started taking swimming classes. The rash is most likely to clear with which of the following therapies?
Terbinafine
Nafcillin
Corticosteroids
Retinoids
Acyclovir
A 10-year-old girl with blue eyes and blonde hair is brought to the office by her mother for a routine check-up. All her immunizations are up to date. Her family history is significant for myocardial infarction in her father and schizophrenia in a maternal uncle. There is no family history of any skin malignancies. Her height is at the 60th percentile, and weight is at the 56th percentile. While you are examining her, the mother says with much concern that she saw a television program that claimed that the incidence of skin cancer is increasing dramatically. She wants to know the best way to prevent skin cancer in her daughter, especially since they live in California. What is the best advice to help prevent malignant melanoma in this child?
Avoid going outdoors
Sun screen lotion with SPF (sun protection factor) 15
Sun screen lotion with SPF 30
Avoid going outdoors
No action needs to be taken, since there is no family history of melanoma
A 50-year-old man comes to the emergency department due to acute onset respiratory difficulty. He also has periorbital, circumoral and facial edema. Two weeks ago, he experienced chest pain, profuse sweating and anxiety, and was subsequently admitted to the cardiac intensive care unit. At that time, his ECG showed ST segment elevation and Q waves in the inferior leads. He was taken to the catheterization lab and had an angioplasty with stent done for 100% occlusion of the right coronary artery. He was discharged with the following medications: aspirin, clopidogrel, metoprolol, enalapril, simvastatin and isosorbide mononitrate. In the ED, his pulse is 102/min, blood pressure is 110/70 mmHg, respirations are 24/min and temperature is 36.8°C (98.4°F). Which of the following is most likely responsible for his present symptoms?
Enalapril
Metoprolol
Lsosorbide
Clopidogrel
Aspirin
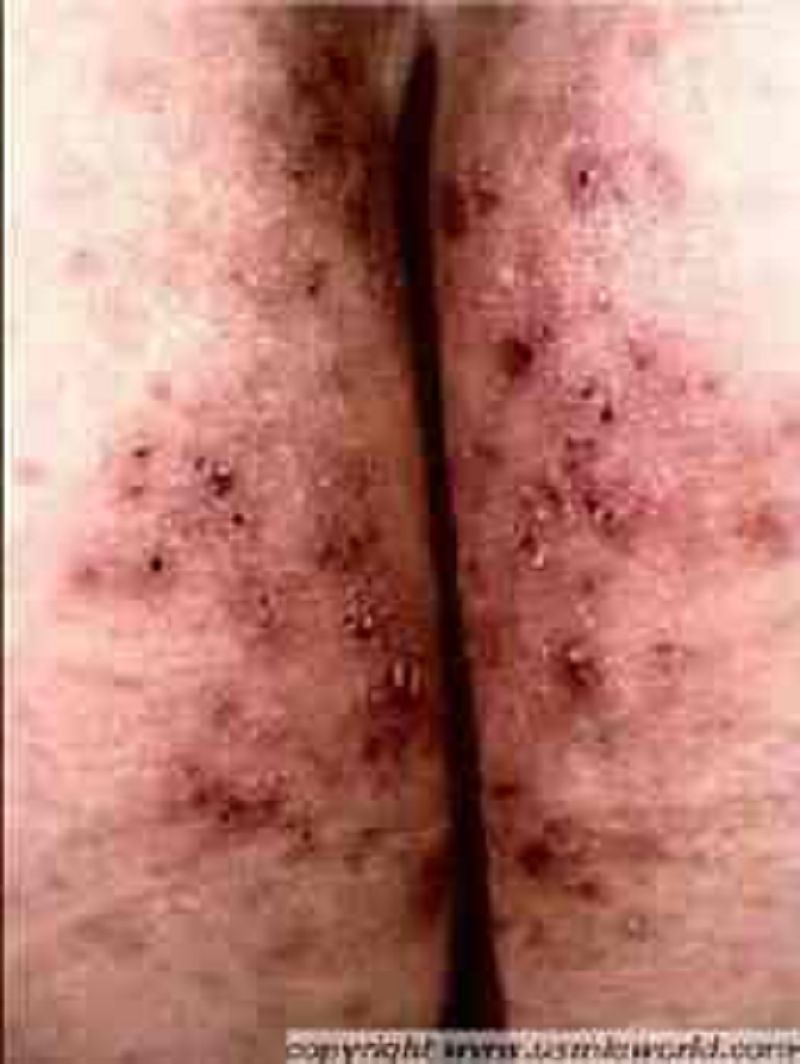
A 25-year-old male presents with skin lesions over his elbows, knees and neck. He complains of intense itching and burning sensation over these lesions for the past 10 days. He was advised to follow a gluten-free diet on his previous visit, but was not compliant. His vital signs are stable. On examination, there are flesh-colored to erythematous vesicles distributed over the extensor aspects of elbows, knees, posterior neck and shoulders. Some of these lesions are shown in the picture below. Which of the following is the drug of choice for his skin condition?
Dapsone
High potency steroids
Low dose acyclovir
1% lindane solution
Azathioprine
A 20-year-old woman complains of skin problems and is noted to have erythematous papules on her face with blackheads (open comedones) and whiteheads (closed comedones). She has also had cystic lesions. She is prescribed topical tretinoin, but without a totally acceptable result. You are considering oral antibiotics, but the patient requests oral isotretinoin, which several of her college classmates have used with benefit. Which of the following statements is correct?
Systemically administered isotretinoin therapy cannot be considered unless concomitant contraceptive therapy is provided
Intralesional triamcinolone should be avoided due to its systemic effects
Antimicrobial therapy is of no value since bacteria are not part of the pathogenesis of the process
The teratogenic effects of isotretinoin are its only clinically important side effects
The patient will not benefit from topical antibiotics since she did not respond to topical retinoids
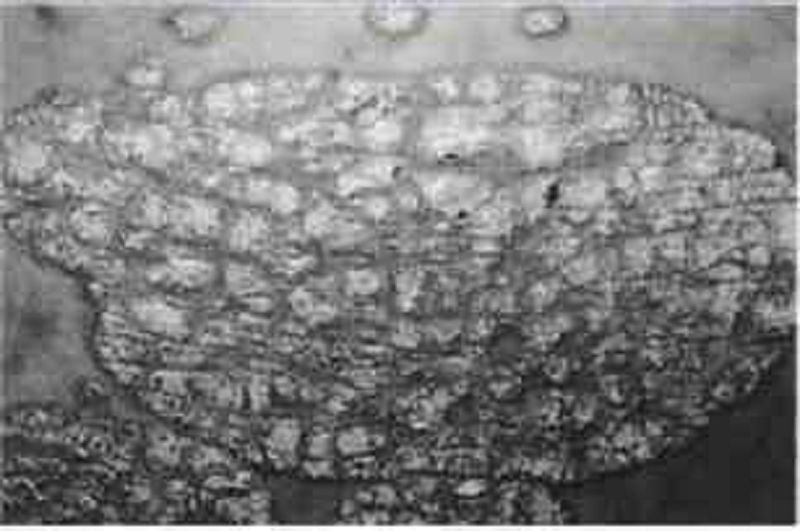
A 22-year-old male presents with a 6-month history of a red, nonpruritic rash over the trunk, scalp, elbows, and knees. These eruptions are more likely to occur during stressful periods and have occurred at sites of skin injury. The patient has tried topical hydrocortisone without benefit. On examination, sharply demarcated plaques are seen with a thick scale. Pitting of the fingernails is present. There is no evidence of synovitis. What is the best first step in the therapy of this patient’s skin disease?
Topical fluticasone
Photochemotherapy (PUVA)
Oral methotrexate
Topical calcipotriene
Oral cyclosporine
A 35-year-old woman develops an itchy rash over her back, legs, and trunk several hours after swimming in a lake. Erythematous, edematous papules and plaques are noted. The wheals vary in size. There are no mucosal lesions and no swelling of the lips. What is the best first step in management of her symptomatic rash?
Oral antihistamines (H1 blockers)
Subcutaneous epinephrine
Intravenous glucocorticoids
Aspirin
Oral doxycycline
A 64-year-old woman presents with diffuse hair loss. She says that her hair is “coming out by the handfuls” after shampooing. She was treated for severe community-acquired pneumonia 2 months ago but has regained her strength and is exercising regularly. She is taking no medications. Examination reveals diffuse hair loss. Several hairs can be removed by gentle tugging. The scalp is normal without scale or erythema. Her general examination is unremarkable; in particular, her vital signs are normal, she has no pallor or inflammatory synovitis, and her reflexes are normal with a normal relaxation phase. What is the best next step in her management?
Reassurance
Measurement of serum testosterone and DHEA-S levels
Topical minoxidil
Topical corticosteroids
CBC and antinuclear antibodies
A 63-year-old retired farmer presents to the clinic complaining of red scaly spots on his head for the past 9 months. Physical examination is remarkable for numerous erythematous hyperkeratotic papules and plaques. The lesions are confined to the head and forehead and have poorly defined borders. Which of the following is the most appropriate next step in management of this patient?
Application of 5-fluorouracil cream to affected areas and follow-up in 4 weeks
Punch biopsy of one of the lesions
Application of hydrocortisone cream to affected areas and follow-up in 4 weeks
Reassurance that this is a benign finding and follow-up in 6 months
Application of fluocinide cream to affected areas and follow-up in 4 weeks
A 21-year-old female presents with an annular pruritic rash on her neck. She explains that the rash has been present for the past 3 weeks and that her roommate had a similar rash not long ago. Physical examination is remarkable for a 20-mm scaling, erythematous plaque with a serpiginous border. Which of the following is the most appropriate initial treatment for this condition?
Topical ketoconazole
Griseofulvin
Oral cephalexin
Topical mupirocin ointment
Hydrocortisone cream
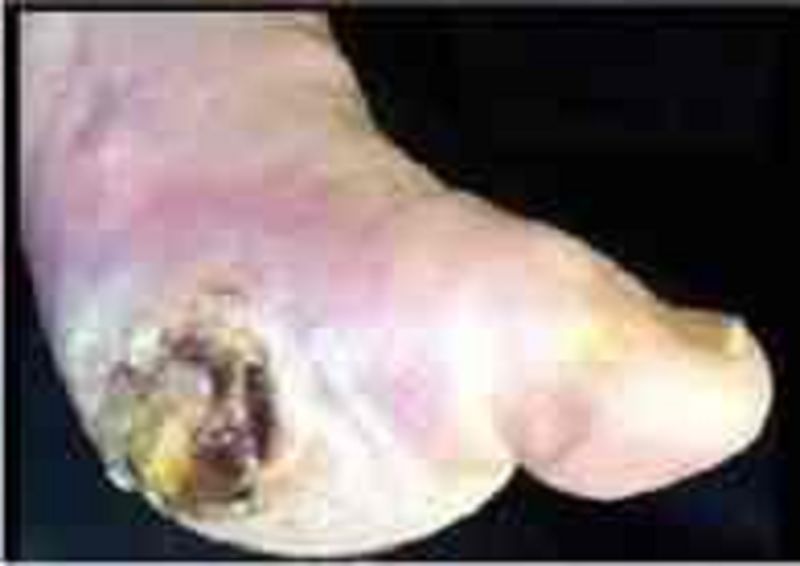
A 50-year-old male comes to the office due to an ulcer in his right foot. He has type 2 diabetes, for which he takes glyburide. Laboratory investigations reveal an HbA1c of 9%, and random blood sugar of 180 mg/dL. X-ray of the leg/foot is normal. A picture of the foot ulcer is shown below. Which of the following is the most appropriate management of this patient's foot ulcer?
Perform thorough debridement of the wound
Start aspirin and atorvastatin
Prescribe tight-fitting shoes
Prescribe oral antibiotics and follow-up as an outpatient
Amputation
A 65-year-old Caucasian male comes to the office because of bilateral foot pain, which is present at rest and worsens at night. He has been having this symptom for the past few months. Other accompanying symptoms are hyperesthesia and paresthesia in both lower limbs. His medical problems include diabetes for the past twenty years. His daily medication is insulin. Physical examination reveals bilateral loss of ankle reflexes, loss of vibratory sensation and altered proprioception below the knees. His HbA1c level is 9%. Urine is positive for microalbuminuria. Which of the following is the most appropriate treatment for his leg pain?
Amitriptyline
Corticosteroids
Oxycodone
Acetaminophen
Ketorolac
A 55-year-old African-American male comes to the office for a routine follow-up visit. His past medical history is significant for type 2 diabetes mellitus (OM), hypertension for the last 5 years, and an acute myocardial infarction 2 years ago. His mother died of a heart attack at the age of 72 years, and his father died in a motor vehicle accident at the age of 42 years. He has no siblings. He is currently on glyburide, captopril and baby aspirin. He is very compliant with his diet and medication. His glycemic control was very good until a few months ago, when he noticed that his blood sugar levels were running high. This morning, his finger stick reading was 200 mg/dL. He weighs 188 lbs and is 5'8" tall. His physical examination is otherwise unremarkable. His blood work done three days ago showed blood urea nitrogen of 14 mg/dL and a creatinine level of 1.0 mg/dL. His HBA1c one month ago was 8.0%. Which of the following is the most appropriate next step in management?
Add metformin to achieve better glycemic control
Discontinue captopril because it is known to produce diabeticogenic state
Discontinue captopril since glyburide efficacy is reduced with simultaneous usage of captopril
Start the patient on human insulin 70/30
Add pioglitazone to achieve better glycemic control
A 60-year-old male comes to the office due to edema of his face and ankles of two weeks duration. He denies any chest pain or breathlessness. He is a known diabetic for the past 15 years. His diabetes is being managed with exercise, dietary modification and glyburide. His glycosylated hemoglobin (HbA1C) level one month ago was 7.5%. His temperature is 37.0°C (98.6°F), pulse is 75/min, blood pressure is 146/87 mmHg, and respirations are 15/min. Examination is unremarkable, except for bilateral pitting edema around the ankles and periorbital edema. Lab results show: Serum sodium 140 mEq/L, Potassium 4.3 mEq/L, Bicarbonate 20 mEq/L, Blood glucose120 mg/dL, Blood urea nitrogen 37 mg/dL, Serum creatinine 24 mg/dL, Total cholesterol 300 mg/dl. EKG is normal. 24 hour urine collection shows 3.7 g protein/day. To alter the course of this patient's diabeticnephropathy, what is the most appropriate next step in management?
Intensive blood pressure control
Intensive glycemic control
Very low protein diet
Aggressive lipid management
Aspirin therapy
A 40-year-old white female presents with complaints of heat intolerance, sweating and palpitations. She also reports menstrual irregularities, increased appetite and diarrhea. She has had these symptoms for the past 4 Months. Her pulse is 102/min and regular, blood pressure is 116/80 mmHg, temperature is 37.2°C (99°F), and respirations are 14/min. Physical examination reveals a non-tender, diffuse swelling in front of her neck; it moves upwards with deglutition. Her TSH level is 0.05 mU/L. Free T4 and T3 levels are increased. Radioactive iodine uptake at 24 hours is significantly increased. Pregnancy test is negative. Which of the following is the most appropriate long-term treatment modality for this patient?
Radioactive iodine therapy
Surgery
Propylthiouracil
Iodinated contrast agents
Propranolol
A 50-year-old Caucasian male comes to the office for the evaluation of polyuria and polydypsia for the last two months. He also complains of weakness and fatigue. He had one episode of transient proximal muscle weakness which lasted 30 minutes. He has a 20-pack year history of smoking. He does not drink alcohol. His past medical and family histories are insignificant. His pulse is 78/min, blood pressure is 150/96 mmHg and temperature is 36.7°C (98°F). The rest of the examination, including the neurological examination, is normal. Labs show: Plasma sodium 150 mEq/L, Potassium 2.6 mEq/L, Serum creatinine 0.8 mg/dL. Which of the following is the most appropriate next step in the management of this patient?
Measurement of plasma renin activity and aldosterone concentration
Measurement of 24 hour urinary potassium excretion
Aldosterone suppression testing
Imaging of adrenals by CT scan
Adrenal vein sampling
A 78-year-old female is being evaluated for recent weight loss and fatigue. Laboratory tests reveal abnormal thyroid function. She begins treatment with a single agent, but soon after is hospitalized with new onset atrial fibrillation and hand tremor. Which of the following treatments had she most likely received?
Radioactive iodine
Propylthiouracil
Lopanoic acid
Propranolol
Prednisone
A 60-year-old female presents with transient loss of consciousness. She appears lethargic and confused. She also complains of hemoptysis and weight loss of 10 lbs (4.5kg) over a period of 2 months. She has smoked one pack of cigarettes daily for the last 40 years. Her temperature is 37.0°C (98.6°F), pulse is 75/min, blood pressure is 110/70 mmHg, and respirations are 16/min. Her mucus membranes are moist. There is no jugular venous distention. Her neurological examination is non-focal, and cardiovascular examination is unrevealing. There is no ankle edema or ascites. Serum studies show: Sodium 115 mEq/L, Potassium 3.7 mEq/L, Bicarbonate 22 mEq/L, Blood glucose 100 mg/dL, BUN 10.0 mg/dL. Serum osmolality is 250 mOsm/Kg, and urine osmolality is 500 mOsm/Kg. Urine sodium concentration is 40 mEq/L. Chest x-ray shows a mass in the right hilar region. What is the most appropriate next step in the management of this patient?
Hypertonic saline
Normal saline
Loop diuretics
Water restriction
Demeclocycline
A 40-year-old African American female comes to the office for a routine medical check-up. She has no complaints. She has twenty pack-year smoking history but she stopped smoking one year ago. Her mother and one maternal uncle have diabetes. Her height is 5'7" inches, and weight is 150 lbs. Her blood pressure is 122/80 mmHg, pulse is 80/min, respirations are 14/min and temperature is 37°C (98°F). She agrees to have diabetes mellitus screening. Her plasma glucose level after an overnight fast is 130 mg/dL. What is the most appropriate next step in the management of this patient?
Repeat fasting blood glucose measurement
Perform 75 g oral glucose tolerance test
Start therapy with oral hypoglycemic agents
Start therapy with insulin
Recommend lifestyle changes
A 22-year-old female presents with complaints of heat intolerance, sweating and palpitations. She also reports menstrual irregularities, increased appetite and diarrhea. Her pulse is 102/min and regular, blood pressure is 116/80 mmHg, temperature is 37.2°C (99°F), and respirations are 14/min. Physical examination reveals a diffusely enlarged, nontender thyroid gland. TSH level is 0.05 mU/L. Free T4 and T3 levels are elevated. Radioactive iodine uptake at 24 hours is 50 percent. Thyroid stimulating immunoglobulins are present. She is started on propylthiouracil 300 mg daily in three divided doses. After two weeks, she returns and complains of a sore throat. Her pulse is 98/min and regular, temperature is 38.6°C (101.5°F), blood pressure is 115/76 mmHg, and respirations are 15/min. The soft palate, pharynx, and tonsils are red and swollen. What is the most appropriate next step in the management of this patient?
Stop propylthiouracil
Add propranolol
Increase propylthiouracil dose
Throat culture
Oral penicillin
A 35-year-old female presents to the emergency department with a 30-minute history of severe headache, palpitations, abdominal pain, nausea, and vomiting. She had similar episodes twice during the last month, but those were not so severe and resolved spontaneously in 30-40 minutes. She visited a doctor recently, and hypertension with elevated urinary vanillylmandelic acid level was diagnosed. She is not taking any medications, and denies substance abuse. Her blood pressure is 200/130 mmHg and heart rate is 130/min. She appears frightened. Physical examination reveals hand tremors and excessive sweating. Slow intravenous infusion of propranolol is started while waiting for the routine labs. What is the most probable reaction to the treatment given to the patient?
Blood pressure will rapidly increase
Blood pressure will slowly decrease
Blood pressure will rapidly decrease
Heart rate will increase
Heart rate will not change
A 65-year-old male comes to the office and complains of nausea and early satiety for the past several months. His other complaints are anorexia and abdominal bloating. He denies any heartburn or epigastric pain. He has diabetes, and has been taking insulin for the last fifteen 15 years. His blood glucose readings using the home blood glucose monitor range between 40 to 400 mg/dL. Most of the low blood glucose readings occur after meals. Which of the following is the most appropriate management of this patient's symptoms?
Metoclopramide
Promethazine
Ondansetron
Ibuprofen
Ranitidine
Four of your patients who came to the office today all have signs and symptoms of hyperthyroidism. After the appropriate evaluation, you decided to treat them with radioactive iodine. Hyperthyroid patients with which of the following disorders are most likely to develop hypothyroidism following radioactive therapy?
Graves' disease
Toxic adenoma
Multinodular goiter
Ectopic production of thyroid hormones
Thyroid Cancer
A 60-year-old Caucasian male presents to the office with erectile dysfunction that progressed slowly over the last several months. He finds it difficult to obtain an erection, and has noted a decrease in nocturnal erections. His past medical history is significant for diabetes mellitus, type 2 and benign prostatic hypertrophy (BPH). His current medications are glyburide and doxazosin. Physical examination is insignificant. HbA1c level measured two weeks ago was 7.5%. He is asking about a prescription for sildenafil. Which of the following is the best statement concerning the treatment of erectile dysfunction in this patient?
Sildenafil and doxazosin should be given with at least a 4-hour interval
Tightening of glycemic control improves erectile dysfunction
Sildenafil is not a drug of choice for diabetics with erectile dysfunction
Prostaglandins (alprostadil) are preferred in this patient
Sildenafil should not be combined with glyburide
A 58-year-old asymptomatic male is found to have elevated levels of serum alkaline phosphate. His serum calcium and phosphate levels are normal. He denies any bone pain or deformity. His liver function tests are normal. The urinary hydroxyproline levels are increased. Nuclear bone scan reveals an increased uptake in the right scapula. Plain radiography confirms Paget's disease. Which of the following is the most appropriate next step in the management of this patient?
No treatment is indicated at this stage
Treatment with bisphosphonates
Treatment with nasal calcitonin
Treatment with calcium and vitamin D
A CT scan of lung

A 25-year-old female comes to the office for a follow-up visit. She was just diagnosed with type 1 diabetes mellitus a few days ago, when she presented at the emergency department with ketoacidosis. After successful management of her diabetic ketoacidosis (DKA), she was sent home on an insulin regimen with the following dosage: Before breakfast 10 units of NPH and 10 units of regular insulin, Before supper 10 units of NPH and 4 units of regular insulin. During this office visit, she shows the record of her fingerstick readings at home. For the last 2 days, her blood glucose levels were (see in pic). What is the most likely explanation for her 7:00 am blood glucose level?
Epinephrine, norepinephrine, & glucagon release
Spikes of growth hormone release
Waning of insulin levels
Destruction of glucagon-secreting cells
Decrease Insulin-secretor
A 46-year-old male comes to your office for a routine health examination. He has no current physical complaints and says he is compliant with his medications. His past medical history is significant for type 2 diabetes diagnosed two years ago that he has been able to control with diet, exercise and metformin. The patient also takes a daily aspirin. On physical examination, he has a temperature of 36.7°C (98°F), a blood pressure of 140/86 mmHg, a pulse of 80/min, and respirations of 14/min. His laboratory studies show: Total cholesterol 170 mg/dl, High density lipoprotein (HDL) 50 mg/dl, Low density lipoprotein (LDL) 65 mg/dl, Triglycerides (TG) 150 mg/dl, HbA1C 7.0. Serum chemistries are with in normal limits. Which of the following is the most appropriate next step in the management of this patient?
Add lisinopril
Add niacin
Add gemfibrozil
Add ezetimibe
Add insulin
A 60-year-old asymptomatic man presents to your office for a routine check-up. He has a 10-year history of type 2 DM, and a 12-year history of hypertension. His current medications include low-dose glyburide and a low-dose thiazide diuretic. His blood pressure is 140/90 mmHg and heart rate is 65/min. Physical examination shows a soft ejection systolic murmur at the base of the heart. Ophthalmoscopic evaluation reveals no abnormalities. ECG recorded 6 months ago showed left ventricular hypertrophy and non-specific ST segment and T-wave abnormalities. His recent fasting glucose level was in the range of 120 to 150 mg/dl, and HbA1c was 7.1 % (normal< 6%). 24-hour urine collection reveals microalbuminuria. Which of the following is the best measure to slow end-organ damage in this patient?
Add ACE inhibitor
Increase the dose of glyburide
Increase the dose of thiazide diuretic
Switch to insulin
Add beta-blocker
A 21-year-old man with type 1 diabetes mellitus presents to the emergency department with complaints of abdominal pain, nausea and vomiting. His temperature is 36.0°C (97.0°F), pulse is 110/min, blood pressure is 102/60 mmHg, and respirations are 26/min. Lungs are clear to auscultation. Abdomen is soft, non-tender and non-distended. Chemistry panel shows: Sodium 130 mEq/L, Potassium 5.2 mEq/L, Chloride 90 mEq/L, Bicarbonate 10 mEq/L, Blood glucose 450 mg/dl. Which of the following is the most appropriate next step in management?
Normal saline and regular insulin
0.45% saline and regular insulin
Normal saline and NPH insulin
5% dextrose and NPH insulin
Sodium bicarbonate
A 40-year-old female patient is brought to the office by her husband due to altered mental status and confusion of recent onset. According to her husband, she has been complaining of intense thirst, craving for ice water, and experiencing increased urination for the past few days. Her only medication is lithium for bipolar depression. Her temperature is 39.0°C (102.5°F), pulse is 102/min, blood pressure is 90/60 mmHg, and respirations are 15/min. Physical examination reveals a disoriented patient with dry skin and mucous membranes. Blood chemistry panel reveals: Sodium 156 mEq/L, Potassium 4.1 mEq/L, Bicarbonate 26 mEq/L, Blood glucose 102 mg/dl, BUN 27 mg/dl. Serum osmolality is 328 mOsm/kg, and urine osmolality is 180mOsm/Kg. What is the most appropriate next step in the management of this patient?
IV infusion of normal saline
Water deprivation test
Plain water drinking
IV infusion of 045% saline
IV infusion of 5% dextrose
A 40-year-old asymptomatic male comes to the office for a routine physical examination. His serum chemistry panel shows: Sodium 140 mEq/L, Potassium 4.0 mEq/L, Bicarbonate 25 mEq/L, Chloride 101 mEq/L, Calcium 11.8 mg/dL, Albumin 4.0 g/dL, Phosphorus 2.2 mg/dL. 24-hour urine collection reveals a calcium level of 200 mg, and creatinine level of 1.7 g. Serum PTH level is increased. Bone mineral density by dual energy X-ray absorptiometry (DEXA) shows normal bone mineral density. Neck examination reveals no masses. What is the most appropriate next step in the management of this patient?
Surgical exploration of the neck
Bisphosphonate therapy
Medical surveillance
Loop diuretics
Thiazide diuretics
A 38-year-old woman presents with several months of decreased libido and a 4.5-kg (10-lb) weight gain. She has not had her menstrual period for the past 3 months. Physical examination is unremarkable except that a small amount of white discharge is manually expressed from the nipples bilaterally. The serum prolactin level is 300 ng/mL. Which of the following is the most appropriate first-line treatment?
Bromocriptine
Cortisol
Methyldopa
Metoclopramide
Octreotide
A 72-year-old woman presents to her physician complaining of fatigue, malaise, weight loss, and salt cravings. The patient has chronic obstructive pulmonary disease and is intermittently treated with corticosteroids but is not using home oxygen. Her oxygen saturation is 97% on room air with a blood pressure of 115/65 mmHg, which is significantly lower than her baseline of 125/78 mmHg. On auscultation she has good breath sounds bilaterally without wheeze, although the expiratory phase is slightly prolonged. Five weeks ago she received a corticosteroid treatment for an acute chronic obstructive pulmonary disease exacerbation, for which she was hospitalized and given 3 L of oxygen via nasal cannula. However, she admits that after discharge she was having continued difficulty breathing and did not follow the taper of the corticosteroids. The patient has smoked one pack of cigarettes per day for the past 51 years. Which of the following is the appropriate first step in the management of this patient?
Restart corticosteroids and follow a strict taper
3 L of oxygen via nasal cannula
CT scan of the chest
Intravenous fluids
X-ray of the chest
An obese patient with a long-standing history of type 2 DM presents to his primary care physician. On examination he has decreased sensation in both lower extremities. Upon questioning of his compliance with his prescribed medications, he reports that he has stopped taking one medication because it gave him flatulence and abdominal pain. Which of the following did this man most likely stop taking?
An α-glucosidase inhibitor
Meglitinide
Metformin
Sulfonylurea
Thiazolidinedione
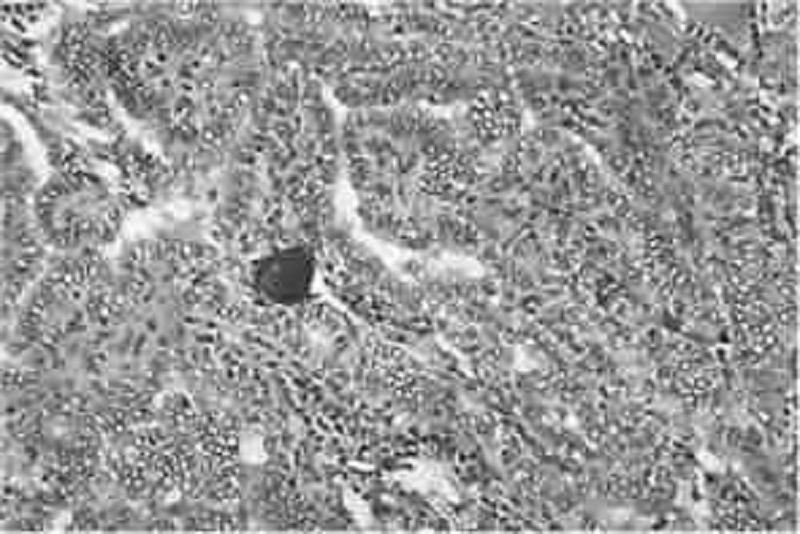
A 19-year-old G1P0 woman at 32 weeks gestation presents for scheduled prenatal appointment. The pregnancy has been uncomplicated to date. However, she mentions that she recently noticed a hard lump on her neck. She denies pain or difficulty swallowing, speaking, or breathing. Physical examination reveals a firm, nontender, immobile, solitary nodule on the left hemithyroid. Ultrasound reveals a solid 2-cm mass. There is no cervical lymphadenopathy. Thyroid function tests reveal a thyroid-stimulating hormone level of 1.2 μU/mL and free thyroxine level of 0.9 ng/dL. Results of fine-needle aspiration biopsy are shown in the image. Which of the following is the best next step in management?
Monitor until after delivery
Left hemithyroidectomy
Radioablation therapy
Start methimazole
Start propylthiouracil
A 49-year-old man presents to the clinic for a health maintenance visit. He has a family history of type 2 DM. His medical history is significant for gastroesophageal reflux disease, for which he takes omeprazole and over-the-counter antacids. He smokes one pack of cigarettes per day and drinks an average of two beers per night. The patient’s body mass index is 32 kg/m². Which of the following most greatly reduce(s) the patient’s risk of future coronary artery disease, renal failure, and retinopathy?
Weight loss and exercise
Alcohol avoidance
Daily multivitamin
Diet rich in fruit and vegetables
Smoking cessation
A 37-year-old white female presents with galactorrhea and amenorrhea for the past 7 months. She denies any headaches, visual problems, vaginal dryness or dyspareunia. She is married, has two children, and remarks that her family is "complete." She does not use tobacco, alcohol or drugs. Her blood pressure is 120/80 mmHg, pulse is 72/min, temperature is 36.7°C (98.6°F) and respirations are 14/min. Visual field testing is within normal limits. Pregnancy test is negative. Her serum prolactin level is 150ng/ml. Pituitary MRI shows a 6mm pituitary adenoma. Which of the following is the most appropriate next step in the management of this patient?
Treatment with cabergoline
Surgery
Treatment with estrogens
Radiotherapy
Monitoring by serum prolactin and MRI
A 32-year-old man presents to his primary care physician complaining of diffuse muscle weakness, dry and puffy skin, and patchy areas of hair loss on his scalp. He also notes numbness around his mouth and a tingling sensation in his hands and feet. He has a history of seizure disorder, and has been taking carbamazepine for the past 5 years. On physical examination he has dry skin and coarse, brittle hair with patchy alopecia. Tapping his right cheek causes contraction of the muscles at the corner of his mouth, nose, and eye on the right side. Which of the following could best have prevented the development of the patient’s current problem?
Vitamin D supplementation
Magnesium supplementation
Parathyroidectomy
Thyroid hormone
Vitamin C supplementation
A 30-year-old Caucasian female comes to the physician's office because of polyuria and polydipsia of recent onset. She has no other medical problems. She does not use tobacco, alcohol or drugs. She has no known drug allergies. Her mother has diabetes. Her temperature is 36.7°C (98°F), pulse is 75/min, blood pressure is 110/70 mmHg, and respirations are 15/min. The initial lab results are: Hb 12.7 g/dl, WBC 5,000 /cmm, Platelets 380,000/cmm, Blood glucose 90 mg/dl, Serum sodium 142 mEq/L, Serum potassium 4.0 mEq/L, Bicarbonate 26 mEq/L, BUN 15 mg/dl, Serum creatinine 0.9 mg/dl, Serum uric acid 9 mg/dl, Serum osmolality 295 mOsm/kg, Urine osmolality 160 mOsm/kg. After 12 hours of water deprivation, lab testing reveals:Serum sodium 151 mEq/L, Serum potassium 4.2 mEq/L, Bicarbonate 26 mEq/L, Serum osmolality 300 mOsm/kg, Urine osmolality 186 mOsm/kg. One hour after the subcutaneous administration of arginine vasopressin, the urine osmolality is 400mosm/kg. Which of the following is the most appropriate treatment for this patient?
Intranasal desmopressin acetate
Psychotherapy
Indomethacin
Hydrochlorothiazide
Demeclocycline
{"name":"Part 4 (765-865) (765-1019) NR 6", "url":"https://www.quiz-maker.com/QPREVIEW","txt":"A 65-year -old Hispanic male is brought to the emergency room with severe substernal chest pain and diaphoresis that began suddenly 1 hour ago. He reports that his pain started while he was at rest and radiates to his left shoulder. The patient notes having vomited twice when the pain first began. Despite administration of 2 baby aspirins and 3 tablets of sublingual nitroglycerin, the pain persists. His initial EKG is shown below. On physical examination, the patient's temperature is 36.9°C (98.4°F), blood pressure is 110\/80 mmHg, pulse is 60\/min, and respirations are 18\/min. S1 and S2 are normal, and an S4 is heard. The lungs are clear to auscultation. There is no jugular venous distension or pedal edema. Interventions to achieve which of the following goals would most improve this patient's long-term prognosis?, A 64-year -old male with a history of hypertension presents with general malaise and a 'funny' heart rhythm for the past 2 weeks. He had an echocardiogram done last year, which revealed mild left atrial dilatation and left ventricular hypertrophy. He has been taking hydrochlorothiazide for hypertension. His blood pressure at today's visit is 180\/98 mmHg. An EKG is obtained and is shown below. Which of the following is the most appropriate treatment for this patient?, A 53-year-old Caucasian male is admitted to the hospital with a 2-week history of fatigue and decreased exercise tolerance. He says he can hardly climb two flights of stairs without getting dyspneic. He denies palpitations or chest pain. His past medical history is insignificant, and a routine check-up 6 months ago was normal. He admits two episodes of binge drinking during the last month, but says that he 'got it under control'. He is currently not taking any medications. His blood pressure is 150\/90 mmHg and heart rate is 130\/min, irregular. Lungs are clear on auscultation. ECG does not reveal P waves. Echocardiography shows significant left ventricular dilation with an ejection fraction of 35% and mitral regurgitation (1+). Which of the following intervention will most likely improve the left ventricular function in this patient?","img":"https://cdn.poll-maker.com/10-472664/1.jpg?sz=1200"}
More Quizzes
Hack Free Fire Gems 2020
100
Find your aesthetic
231233
100
Which grandparent are you from 'The Maples'?
630
Free Industrial Safety Knowledge
201021031
Master Airfield Driving: Test Your Flightline Safety Skills
201023063
Topics in Film and History
15822223
Ultimate Foods of the World: Can You Name Them All?
201042371
La Casa de Bernarda: Bernarda Perra Trivia Challenge
201063672
Free Chapter 3 Review Test & Health
201024800
What Avatar Element Are You? Free Fun Personality
201023063
Is a Rhombus Always a Rectangle? Square & Rhombus
201063672