P 427 p 444 *No 1 to 50 *
1) A 74-year-old man presents to your office for a routine. He has no present complaint. His medical history is significant for right knee osteoarthritis. He takes naproxen occasionally, to relieve knee pain. He does not smoke or consume alcohol. His BP is 165/75 mmHg and PR is 70/min. The physical examination showed a mild systolic ejection type murmur at the base of the heat to the right. An E-KG revealed left ventricular hypertrophy and secondary ST segment and T wave change. Moderate left ventricular hypertrophy, without any flow abnormalities, was demonstrated on echocardiography. The ejection fraction was 60%. What is the most probable cause of hypertension in this patient?
. Rigidity of the arterial wall
. Elevated plasma renin activity
. Aortic insufficiency
. Increased cardiac output
. Increased intravascular volume
.2) A 47-year-old woman loses consciousness for 2 minutes while shopping in a supermarket. In the emergency room, she recounts feeling nausea and warmth spreading over her body immediately before passing out. She has never had a similar episode before. She has not seen a doctor for several years and does not take any medications, nor does she use tobacco, alcohol or drug. Her family history is unremarkable. Which of the following most likely caused this episode?
. Cardiac arrythmia
. Seizure
. Neurocardiogenic syncope
. Heat valve disease
. Orthostatic hypotension
.3) A 25-year-old woman experiences sudden-onset palpitations and generalized weakness. During this episode, her blood pressure is 100/60 mmHg and her heat rate is 160/min and regular. She has no significant past medical history and does not take any medications. She reports having a few similar episodes in the past which she has self-treated by immersing her face in cold water. Generally, she says, cold water immersion relieves her symptoms within several minutes. This cold water therapy works by affecting which of the following?
. Vascular tone
. Sinoatrial node automatism
. Atrioventricular node conductivity
. Purkinje fiber conduction
. Ventricular myocardium contractility
.4) A 67-year-old man is evaluated for hypertension. He complains of occasional morning headaches. His past medical history is also significant for type 2 diabetes mellitus, coronary artery disease, and a stroke with residual left-sided weakness. He underwent coronary artery bypass surgery seven years ago and carotid endarterectomy five years ago. His current medication list includes lisinopril hydrochlorothiazide, amlodipine, metoprolol, aspirin, metformin and glyburide. His blood pressure is 190/120 mmHg on the right arm and 170/110 mmHg on the left arm. His heat rate is 65/min Physical examination reveals a periumbilical systolic-diastolic bruit. The latter finding is best explained by which of the following?
. Abdominal aortic aneurysm
. Aortic dissection
. Aortic coarctation
. Renal artery stenosis
. Aorto-enteric fistula
.5) A 67-year-old male is brought to the emergency department after a syncopal episode. He lost consciousness while shopping in the mall. He denies any nausea, diaphoresis, chest pain, or shortness of breath. He has had two episodes of lightheadedness over the last month but has not seen a doctor. His past medical history is significant for long-standing hypertension, which is being treated with enalapril. His blood pressure is 135/90 mmHg while supine, and 130/85 mmHg while standing. His heat rate is 64/min. ECG shows a sinus rhythm with high voltage, prolonged PR interval, prolonged QRS interval, normal QT interval and occasional premature ventricular contractions (PVC). Echocardiography reveals left ventricular hypertrophy and an ejection fraction (EF) of 55%. Which of the following is the most likely cause of this patient's syncope?
. Bradyarrhythmia
. Decreased myocardial contractility
. Torsades de pointes
. Autonomic dysfunction
. Ventricular premature beats
.6) A 47-year-old male presents to your office with a two-month history of lethargy and decreased libido. His medical records reveal that he has been treated for joint pain and swelling over the last six months and was diagnosed with diabetes mellitus one year ago. Physical examination reveals hepatomegaly and testicular atrophy. Which of the following cardiac abnormalities is most likely to also be present in this patient?
. Atrial septal defect
. Aortic stenosis
. Hypertrophic cardiomyopathy
. Cardiac conduction block
. Endocardial fibroelastosis
.7) A 50-year-old woman presents to your office complaining of lower extremity edema that stated several weeks ago, and slowly progressed thereafter. Her past medical history is significant for hypertension, treated with metoprolol for 2 years. Amlodipine was added recently because of inadequate control of BP with metoprolol alone. She does not smoke or consume alcohol. She has no known drug allergies. Her blood pressure is 130/80mmHg and her heart rate is 64/min. The physical examination reveals bilateral symmetric 3+ pitting edema of both lower extremities, without any skin changes or varicosities. Her neck vein pulsation is normal. Other physical findings are within normal limits. Her laboratory studies reveal the following: Serum albumin 4.5 g/dL, Total serum bilirubin 0.8 mg/dL, Serum sodium 140 mEq/L, Serum potassium 4.0 mEq/L, Serum creatinine 0.8 mg/dL. Urinalysis is within normal limite. What is the most likely cause of the edema in this patient?
. Heart failure
. Liver disease
. Renal disease
. Venous insufficiency
. Side effect of her medications
.8) A 63-year-old man presents to the ER with substernal chest pain and diaphoresis. The pain stated one hour ago and did not remit with antacids. He has a past medical history of asthma for which he uses inhaled fluticasone and peptic ulcer disease for which he takes omeprazole. His family history is significant for prostate cancer in his father and breast cancer in his mother. Physical examination reveals a blood pressure of 160/100 mmHg and a heat rate of 90/min. A bruit is heard over the right carotid artery and a mild systolic murmur is present at the cardiac apex. Sublingual nitroglycerin and aspirin are administered in the. Within minutes, the patient reports decreased pain. Which of the following most likely accounts for this improvement in his symptoms?
. Increased left ventricular compliance
. Decreased left ventricular volume
. Decreased left ventricular contractility
. Increased systemic afterload
. Increased cardiac preload
.9) A 38-year-old female comes to your office complaining of occasional palpitations. She describes feeling a fast and irregular heartbeat. Over the past two months, she has had three such episodes, each lasting about two hours. She denies any associated chest pain, shortness of breath cough or ankle swelling. She drinks alcohol on social occasions and does not smoke cigarettes. She has no other medical problems and is not taking any medications. On physical examination, her temperature is 37.1°C (98.9°F), pulse is 80/min, blood pressure is 130/70mmHg, and respirations are 14/min. On auscultation of her heat the apical impulse is displaced and there is an S3. You also hear a pansystolic murmur, which is loudest at the apex and radiates to the axilla. Which of the following is the most likely cause of her symptoms?
. Mitral valve prolapse
. Myocardial ischemia
. Rheumatic heat disease
. Mitral annular calcification
. Infective endocarditis
.10) A 42-year-old woman is evaluated for depression, mood swings and poor. She also complains of mild headaches and muscle weakness. She has had two ER visits for kidney stones over the past year. She denies any illicit drug use. Her blood pressure is 160/105 mmHg and her heat rate is 85/min. Her laboratory findings are shown below: Sodium 140mEq/L, Potassium 3.6 mEq/L, Chloride 101 mEq/L, Bicarbonate 24 mEq/L, BUN 13 mEq/L, Creatinine 0.9 mEq/L, Glucose 98 mEq/L, Calcium 11.7 mg/dL. Which of the following is the most likely cause of this patient's hypertension?
Renal parenchymal disease
. Renal vascular stenosis
. Aortic dissection
. Hypothyroidism
. Parathyroid gland disease
.11) A 14-year-old African American male is referred to your office after his older brother experienced sudden cardiac arrest during hiking trip. He has no current complaints. He denies any illicit drug use. His blood pressure is 110/60 mmHg and his heat rate is 75/min. Neck is supple, no jugular venous distention is appreciated. Carotid pulse seems to have dual upstroke. Lungs are clear. There is strong apical impulse and a systolic ejection type murmur along the left sternal border. Which of the following is most likely to increase the murmur intensity in this patient?
. Squatting
. Valsalva maneuver
. Sustained handgrip
. Recumbency
. Leg raising
.12) A 60-year-old male is brought to ER by his son because he had an episode of syncope. He was watching TV in an arm-chair when suddenly lost his consciousness without any warning sign. He had several clonic jerks while unconscious. He never had such an episode before. His past medical history is significant for acute myocardial infarction six months ago and well-controlled hypertension. His current medications include captopril metoprolol hydrochlorothiazide, clopidogrel and aspirin. His blood pressure is 130/85 mmHg and heat rate is 80/min with frequent ectopic beat. Physical examination revealed mild holosystolic apical murmur radiating to the axilla. Which of the following is the most probable pathophysiologic mechanism for his syncopal episode?
. Vasovagal reaction
. Arrhythmia
. Autonomic dysfunction
. Seizure
. Postural hypotension
.13) A 54 year-old male comes to the physician because of abdominal distention. He thinks his big belly is making it hard for him to breathe. He received radiation therapy for Hodgkin lymphoma several years ago and was told that he is cured. He drinks alcohol on a regular basis. His temperature is 36.7°C (98°F), blood pressure is 120/76 mm Hg, pulse is 80/min and respirations are 20/min. Examination shows a jugular venous pressure 7 cm above the sternal angle. Dullness to percussion and decreased breath sounds are noted in the right lung base. The abdomen is quite distended with an obvious fluid wave. Mild hepatomegaly is present. Extremities have 2+ lower extremity edema. Initial laboratory studies are shown below: Serum creatinine 08 mg/dL, Alburnin 4.0 mg/dL, Total bihrubin 1.0 mg/dl, Prothrombin time 11 sec. Urinalysis is within normal limits. Which of the following is the most likely cause of his condition?
. Urinary protein loss
. Portal vein thrombosis
. Portal vein compression
. Inelastic pericardium
. Thoracic duct obstruction
.14) A 32-year-old woman presents with progressively worsening dyspnea on exertion one month after returning from a vacation in Texas. She says that her symptoms have progressed to the point that she now wakes during the night with a choking sensation that improves only with sitting up. Recently her shortness of breath has required her to significantly limit her physical activity. She denies having associated chest pain, skin rash or joint pain. She has no significant past medical history. Family history is significant for thyroid cancer in her aunt and lung cancer in her father, a heavy smoker. On physical examination, her temperature is 37.2°C (99°F), pulse is 96/min, blood pressure is 110/70 mmHg, and respirations are 14/min. Bilateral pitting ankle edema is present. Her liver is enlarged 2 cm below the right costal marginal. Lung auscultation reveals decreased breath sounds at the bilateral bases. Cardiac exam reveals the presence of a third heat sound. Chest x ray shows an enlarged cardiac silhouette and small bilateral pleural effusion. EKG is unremarkable. Which of the following is the most likely cause of her symptoms?
. Atherosclerosis
. Viral infection
. Lyme disease
. Coccidioidomycosis
. Autoimmune disease
.15) An 88-year-old female nursing home resident is brought to the hospital with a one-week history of moaning, decreased oral intake and decreased ambulation. Physical examination reveals a very thin female who is moaning and appears to be in pain. She opens her eyes spontaneously but does not respond to questions. Her blood pressure is 75/43 mmHg, pulse is 105/min, temperature is 35.5°C (96°F), and respirations are 22/min. Oxygen saturation (pulse oximetry) is 97% on room air. Her skin and oral mucosa are dry and her neck veins are flat. There is no lymphadenopathy. On chest auscultation, there are crackles in the right upper lung lobe. Abdomen is soft and non-distended. There is 2+ pitting presacral and lower extremity edema, and a deep pressure ulcer in the sacral area. Laboratory analysis reveals the following: Sodium 155mEq/L, Potassium 5.3 mEq/L, Glucose 88mg/dL, Bicarbonate 14mEq/L, BUN 151mg/dL, Creatinine 3.1mg/dl. Which of the following is the most likely cause of her lower extremity edema?
. Increased plasma hydrostatic pressure
. Decreased plasma oncotic pressure
. Renal water and sodium retention
. Increased interstitial oncotic pressure
. Decreased lymphatic drainage
.16) A 64-year-old man complains of palpitations and progressive shortness of breath over the past several hours. He says that he also develops a choking sensation every time he tries to lie down. His medical history is significant for hypertension for the past 20 years and medication non-compliance. He also has a 35-year smoking history. He reports that his father died of a heart attack at age 70 and his mother suffered from asthma. On physical examination, his blood pressure is 170/100 mmHg and his heat rate is 130/min and irregularly irregular. Lung exam reveals bibasilar crackles. There is 2+ pitting edema of the lower extremities. Bedside echocardiography shows a left ventricular ejection fraction of 55%. Which of the following is most likely responsible for his symptoms?
. Cardiogenic shock
. Diastolic dysfunction
. High-output heat failure
. Small airway bronchoconstriction
. Increased lung compliance
.17) A 55-year-old Caucasian male presents to your office with muscle pain of recent onset. His past medical history is significant for hypertension and an acute myocardial infarction experienced 2 months ago. His current medications include metoprolol captopril, aspirin and simvastatin. His blood pressure is 130/80 mmHg and heat rate is 60/min. Liver function tests are slightly abnormal. Serum creatine kinase level is elevated. You suspect a drug-induced reaction. Which of the following is the most possible mechanism of drug-induced reaction in this patient?
. Immune-mediated reaction
. Cell surface receptor blockage
. Extracellular enzyme blockage
. Synthetic reaction inhibition
. Damage of membrane-bound lipids
.18) A 70-year-old man is brought to the Emergency Room because he lost his consciousness while working in the garden. He says that he had several episodes of near-syncope on exertion recently. His past medical history is insignificant. He is not taking any medications. His blood pressure is 110/85 mmHg and heat rate is 80/min. Point of maximal impulse is increased in intensity. Cardiac auscultation reveals ejection type systolic murmur at the base of the heat with radiation to the carotid arteries. ECG demonstrates left ventricular hypertrophy, and secondary ST segment and T wave change. What is the most probable cause of this patient's condition?
. Rheumatic endocarditis
. Bacterial endocarditis
. Hypertension
. Congenital anomaly
. Age-related sclerocalcific changes
.19) A 32-year-old male complains of progressive weakness and exertional dyspnea. His past medical history is significant for a knife injury to the right thigh two months ago. He has been arrested several times for robbery. He consumes alcohol regularly, and smokes crack occasionally. His younger brother died of cystic fibrosis. His blood pressure is 160/60 mmHg, and heart rate is 100/min. His extremities are warm and flushed. Carotid upstroke is brisk. The point of maximal impulse is displaced to the left, and a soft, holosystolic murmur is heard over the cardiac apex. The murmur does not change with the Valsalva maneuver. Which of the following is the most likely cause of this patient's symptoms?
. Decreased cardiac output
. Hypertrophic cardiomyopathy
. Increased cardiac preload
. Papillary muscle dysfunction
. Pulmonary hypertension
.20) A 22-year-old college student went to the health clinic complaining of a fever over the last 5 days, fatigue, myalgias, and a bout of vomiting and diarrhea. The clinic doctor diagnosed him with acute gastroenteritis and told him to drink more fluids. Three days later, the student presents to the ED complaining of substernal chest pain that is constant. He also feels short of breath. His temperature is 100.9°F, HR is 119 beats per minute, BP is 120/75 mmHg, and RR is 18 breaths per minute. An ECG is performed revealing sinus tachycardia. A chest radiograph is unremarkable. Laboratory tests are normal except for slightly elevated WBCs. Which of the following is the most common cause of this patient’s diagnosis?
. Streptococcus viridans
. Influenza A
. Coxsackie B virus
. Atherosclerotic disease
. Cocaine abuse
.21) A 60-year-old man is brought to the ER by his wife because he lost consciousness in the bathroom at night. He says that he woke up, went to the bathroom to urinate, and fainted there. He rapidly recovered his consciousness without any indication of disorientation. He has never had such an episode before. He admits' problems with urination,' including difficulty with initiating urination and frequent awakening to void at night. He does not take any medication. His past medical history is insignificant. He smokes 2 packs of cigarettes per day and does not consume alcohol. His blood pressure is 130/80 mmHg while supine, and 132/80 mmHg while standing. His heart rate is 70/min. His physical examination is within normal limits. The ECG is normal. What is the most probable cause of the syncopal episode in this patient?
. Arrhythmia
. Postural hypotension
. Situational syncope
. Seizure
. Transient ischemic attack (TIA)
.22) A 73-year-old man presents to the ED after a syncopal episode. He had been resting in bed for approximately one week after injuring his right knee. This morning, his knee felt better and he attempted to get up from bed. However, upon attempting to stand, he sustained a brief loss of consciousness. He had no symptoms or medical history prior to the knee injury. Medications include acetaminophen and ibuprofen for knee pain. On exam, his pulse is 73/min, respirations are 14/min, and blood pressure is 136/83 mmHg. Which of the following is the most likely cause of this patient's syncope?
. Cardiac arrhythmia
. Valvular obstruction
. Orthostatic hypotension
. Vagal nerve hyperactivity
. Hyperventilation
.23) A 46-year-old woman is hospitalized for agitation, restlessness and poor sleep. She has been complaining of headaches recently and has gained 14 pounds over the past three months. She denies any illicit drug use. Her blood pressure is 160/110 mmHg and her heart rate is 90/min. Her laboratory findings are shown below: Sodium 142 mEq/L, Potassium 3.2 mEq/L, Chloride 98 mEq/L, Bicarbonate 26 mEq/L, BUN 12 mg/dl, Creatinine 0.9 mg/dl, Glucose 205 mg/dl, Calcium 94 mg/dl. Which of the following is the most likely cause of this patient's hypertension?
. Renal parenchymal disease
. Adrenal medullary disease
. Adrenal cortical disease
. Hypothyroidism
. Parathyroid gland disease
.24) A 53-year-old man presents to the emergency room with squeezing chest pain that started two hours ago. He also complains of shortness of breath that is worse when lying down. He has never had pain like this before. He has no significant past medical history and he takes no medications. A routine health maintenance visit two weeks ago was normal. On physical examination in the ER, his blood pressure is 140/90 mmHg and his heart rate is 100/min. Chest auscultation reveals a grade II/VI blowing systolic murmur at the cardiac apex and bibasilar crackles in the lungs. ECG shows ST segment elevations in leads I, aVL, and v1-v3. Which of the following is most likely increased in this patient?
. Left atrial pressure
. Left atrial size
. Left ventricular compliance
. Left ventricular ejection fraction
. Right ventricular preload
.25) A 35-year-old woman who has recently emigrated from Asia presents to the emergency room with acute onset of dyspnea. She denies any cough, chest pain, or fever. She has a history of rheumatic heart disease as a teen. On examination, she has an irregular pulse of 97/min, blood pressure of 125/75 mmHg and temperature of 37.2°C (98.9°F). The first heart sound is loud and a mid-diastolic rumble is heard at the apex. Crackles are present in both lung fields. ECG shows an irregularly, irregular heart rhythm and the absence of 'P' waves. Which of the following is the most likely cause of this patient's abnormal heart rhythm?
. Left atrial dilatation
. Right atrial dilatation
. Left ventricular dilatation
. Left ventricular hypertrophy
. Pulmonary hypertension
.26) An 82-year-old male presents for evaluation of chronic back pain. On physical examination, he is found to have a blood pressure of 160/85 mmHg while supine and 135/70 mmHg while standing. He is otherwise healthy; his only medicine is occasional ibuprofen for back pain. Which of the following age-related changes best explains the observed finding?
. Increased left ventricular wall stiffness
. Decreased left ventricular contractility
. Decreased baroreceptor responsiveness
. Decreased stress-mediated catecholamine release
. Decreased glomerular filtration rate
.27) A 70-year-old Caucasian man comes to the emergency department because of the sudden onset of nausea, vomiting, diaphoresis, and chest pain. His other medical problems include hypertension, diabetes mellitus-type 2, and aortic stenosis. He has smoked one-and-a-half packs of cigarettes daily for 30 years and drinks 4 ounces of alcohol daily. His temperature is 37.2°C (99°F), blood pressure is 100/60 mmHg, pulse is 60/min, and respirations are 18/min. The patient's pulse oximetry showed 98% at room air. Examination shows normal first and second he sounds. Lungs are clear to auscultation. His EKG is shown below. Which of the following is the most likely mechanism of this patient's condition?
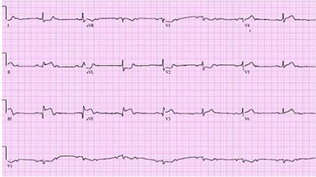
Share

. Occlusion of the right coronary artery
. Occlusion of the left circumflex artery
. Occlusion of the left anterior descending artery
. Inflammation of the pericardium
. Vasospasm of the left circumflex artery
.28) A 24-year-old male experiences syncope while shovelling snow. He regained consciousness within one minute. He has been having some shortness of breath and chest pains recently, mostly related to exercise. He denies any illicit drug use. His temperature is 37.2°C (98.9°F), and blood pressure is 126/76 mmHg, pulse is 76/min and respirations are 14/min. Physical examination shows a well-built male in no apparent distress. Lungs are clear. A crescendo-decrescendo systolic murmur is heard along the left sternal border without carotid radiation. Chest X-ray is normal. Which of the following is the most likely cause of his syncopal episode?
. Atrioventricular conduction delay
. Left ventricular hypertrophy
. Aortic dissection
. Coronary atherosclerosis
. Mitral valve degeneration
.29) A 33-year-old woman is undergoing an elective, open cholecystectomy after 2 episodes of acute calculous cholecystitis. She suddenly becomes hypotensive, and a generalized rash is noted. Her past medical history is significant for a hypotensive episode 8 weeks ago while having protected sex with her new partner. Which of the following is the most probable cause of this patient's condition?
. Acute blood loss
. Coagulation abnormality
. Allergic reaction
. Septic shock
. Pulmonary embolism
.30) A 72-year-old male comes to the office with intermittent symptoms of dyspnea on exertion, palpitations, and cough occasionally productive of blood. On cardiac auscultation, a low-pitched diastolic rumbling murmur is faintly heard at the apex. What is the most likely cause of the murmur?
. Rheumatic fever as a youth
. Long-standing hypertension
. A silent MI within the past year
. A congenital anomaly
. Anemia from chronic blood loss
.31) A 53-year-old male presents to your office with a two-day history of right calf pain and swelling. He describes the pain as constant and states that it is exacerbated by knee flexion. He has a history of past IV drug abuse, endocarditis, and stroke. He is currently wheelchair-bound secondary to stroke-related left-sided hemiparesis. On physical examination, his blood pressure is 140/90 mmHg and his heart rate is 100/min. There is no jugular venous distention or hepato-jugular reflux. His chest is clear to auscultation but his abdomen is enlarged with shifting dullness and a fluid wave, suggestive of ascites. His liver is palpable 3 cm below the right costal margin. His spleen is also palpable. On examination of his lower extremities, you note right-sided calf swelling and tenderness. Which of the following is the most likely cause of this patient's ascites?
. Right-sided heart failure
. Pulmonary embolism
. Protein C deficiency
. Chronic liver disease
. Paradoxical embolism
.32) A 60-year-old white man comes into the Emergency Room with intensive retrosternal pain that began ten minutes ago. He has never had such pain before. His past medical history is significant for diabetes mellitus, type 2, controlled with diet. His blood pressure is 150/95 mmHg and HR is 80/min. You give him one chewable tablet of aspirin and two sublingual tablets of nitroglycerin with a 5-minute interval. After the second tablet of nitroglycerin, the pain is greatly relieved. What is the most important mechanism responsible for pain relief in this patient?
. Increase in coronary blood flow
. Increased cardiac contractility
. Dilation of resistance vessels
. Dilation of capacitance vessels
. Change in the activity of baroreceptors
.33) A 34-year-old male who recently immigrated from Brazil presents with a 5-month history of exertional dyspnea without associated chest pain, palpitations, dizziness, or syncope. His past medical history is significant for an episode of megacolon, which was treated 2 years ago. On physical examination, there is 1+ pedal edema and mild jugular venous distention. Cardiac exam is significant for the presence of an S3, but no murmurs are heard. Chest x-ray reveals prominent cardiomegaly. Based on these findings, which of the following is most likely causing his symptoms?
. Diphtheric myocarditis
. Coronary artery disease
. Protozoal disease
. Giant cell myocarditis
. Rickettsial myocarditis
.34) A 12-year-old African American male is found to have a murmur during a routine sports physical. He has a family history of sudden death at a young age. It is a harsh crescendo-decrescendo murmur that begins after S1 and is best heard at the left lower sternal border. Valsalva maneuver intensifies the murmur. Which of the following is the most likely mitral valve abnormality in this patient?
. Dilated mitral valve annulus
. Rupture of chordae tendinae
. Abnormal mitral leaflet motion
. Mitral annulus calcifications
. Prolapse of the mitral valve
.35) A 63-year-old woman with a long history of hypertension faints after experiencing the sudden onset of severe chest pain that radiates to her back. She is rushed to the emergency room. Upon arrival she is agitated and demands quick pain relief. Her heart rate is 110/min and blood pressure is 90/50 mmHg. Jugular veins are distended. An intra-arterial catheter shows significant variation of systolic blood pressure related to the respiratory cycle. Chest x-ray reveals widening of the mediastinum. Which of the following is the most likely cause of this patient's syncope?
. Papillary muscle dysfunction
. Intravascular volume loss
. Pericardial fluid accumulation
. Vagal hyperactivity
. Cardiac tachyarrhythmia
.36) A 47-year-old male was brought to the emergency room with chest pain of acute onset. The pain was associated with nausea, vomiting, and diaphoresis. He has a history of diabetes, hypertension, and hyperlipidemia. ECG reveals ST segment elevation in the anterolateral leads and ventricular premature beats (VPBs). The patient dies within the first hour after the arrival to emergency room. What is the most likely pathophysiologic mechanism responsible for this patient's death?
. Electro-mechanic dissociation
. Reentry
. Full conduction block
. Increased automaticity
. Asystole
.37) A 57-year-old male presents to your office with a two week history of fever, chills, and generalized weakness. His medical history is significant for a hospitalization for pyelonephritis requiring IV antibiotics six months ago. He also recently underwent cystoscopy for evaluation of persistent dysuria. His past medical history is also significant for an episode of rheumatic fever as a child and Hodgkin's lymphoma treated with chemotherapy 10 years ago. On examination, his temperature is 37.8°C (100°F), blood pressure is 150/86 mmHg, pulse is 98/min and regular, and respirations are 16/min. The patient appears slightly diaphoretic. You note a new II/VI systolic murmur and tender erythematous lesions affecting several fingertips. The remainder of the physical examination is unremarkable. Which of the following bacteria is most likely responsible for his present illness?
. Streptococcus pyogenes
. Staphylococcus epidermidis
. Enterococci
. Viridans streptococci
. Coxiella burnetii
.38) A 65-year-old man complains of lower leg swelling, fatigue and poor appetite. His past medical history is significant for recurrent chest infections, wheezing, cough, recent pyelonephritis, and arterial hypertension. He smokes 1 pack of cigarettes a day but denies alcohol or intravenous drug use. His physical examination reveals a barrel-shaped chest with bilateral scattered wheezes. His abdomen is distended and his liver edge is palpated 4 cm below the right costal margin. You note pitting edema and dilated, tortuous, superficial veins over the bilateral lower extremities. Manual pressure on the abdomen causes persistent distention of the jugular veins. The patient's serum sodium level is 135 mEq/L and his creatinine concentration is 1.2 mg/dl. An abnormality of which of the following is most likely to explain his edema?
. Serum albumin level
. Pulmonary artery systolic pressure
. Pulmonary capillary wedge pressure
. Portal venous resistance
. Urinary protein excretion
.39) A 60-year-old male presents to the emergency room with the chief complaint of progressive exertional dyspnea and fatigue. He denies any chest pain, syncope, cough, or edema. He suffered an acute anterior wall myocardial infarction one month ago. Chest auscultation reveals bilateral crackles in his lower chest. Cardiac auscultation reveals a pansystolic murmur at the apex with radiation to the axilla. ECG shows previously present unchanged Q waves and a persistent ST segment elevation in the anterior leads. Based on these findings, what is the most likely underlying cause of his symptoms?
. Interventricular wall rupture
. Ventricular free wall rupture
. Ventricular aneurysm
. Recurrent ischemia
. Right ventricular infarction
.40) A 68-year-old white female presents to the ER complaining of sudden onset chest pain associated with two episodes of vomiting. She has hypertension for which she takes atenolol and hydrochlorothiazide. Her pulse is 60/min, blood pressure is 80/50 mmHg and respirations are 14/min. Examination shows elevated jugular venous pressure and a positive Kussmaul's sign. Her lungs are clear to auscultation. Her EKG shows 2 mm ST segment elevation in leads II, III and aVF and 1 mm ST segment depression in leads I and aVL. Which of the following is the most likely cause of this patient's hypotension?
. Pulmonary thromboembolism
. Right ventricular infarction
. Interventricular septum rupture
. Variant angina
. Intravascular volume depletion
.41) A 53-year-old man presents to your office complaining of weakness and exertional dyspnea over the last week. He denies chest pain and palpitations. He has no other past medical history. His father died of a myocardial infarction at age 55. On exam, his heart rate is 100/min and blood pressure is 90/60 mmHg. Internal jugular venous pulsation is observed 7 cm above the sternal angle. Lungs are clear to auscultation. Heart sounds are muffled. Which of the following is the most likely cause of this patient's complaints?
. Decreased cardiac contractility
. Left ventricular outflow obstruction
. Decreased left ventricular preload
. Pulmonary hypertension
. Increased right ventricular compliance
.42) A 34-year-old man rushes into the ER complaining of severe substernal chest pain that began abruptly 30 minutes ago. He says that he also feels as though his heart 'is racing,' but denies any shortness of breath, cough or fever. He has never experienced pain like this before. His past medical history is significant for an appendectomy one year ago. The patient reports that his father died at age 64 due to "some heart problem" and his mother died of ovarian cancer. On physical examination, the patient is agitated and sweating profusely. His pulse is 110/min, blood pressure is160/100 mmHg, and respirations are 14/min. Physical examination is normal except for dilated pupils and a small amount of blood at the external nares. EKG shows ST elevations in leads v1-v4. What is the most likely explanation for his symptoms?
. Atherosclerotic vascular disease
. Acute pericarditis
. Pleurodynia
. Drug-induced vasospasm
. Aortic dissection
.43) A 50-year-old white male comes into your office for a routine check-up. He has no present complaints. His past medical history is significant for hypertension controlled with a low-dose thiazide diuretic. His family history reveals non-fatal myocardial infarction in his father at the age of 47. The patient does not smoke or consume alcohol. His blood pressure is 130/75 mmHg and his heart rate is 70/min. His previous records show that his HDL level is persistently low in spite of acceptable total cholesterol and LDL levels. You prescribe niacin to raise HDL level. The patient returns in a week complaining of intensive generalized pruritis and flushing. What is the most probable cause of the patient's complaint?
. Hypersensitivity reaction
. Prostaglandin-related reaction
. Drug interaction
. Drug-induced vasoconstriction
. Psychogenic reaction
.44) A 63-year-old male is admitted for sudden onset severe chest pain. His ECG reveals ST elevation in leads V2-V6. He is treated with thrombolytic therapy, heparin, aspirin, metoprolol, morphine, and nitrates. A coronary angiogram performed after thrombolytic therapy reveals 50% obstruction of the left anterior descending artery. On the third day of hospitalization, the patient suddenly develops severe shortness of breath at rest and hypotension. Examination reveals a soft S1, an apical pansystolic murmur radiating to the axilla, and bibasilar crackles. His temperature is 37.8°C (100°F), blood pressure is 92/58 mmHg, heart rate is 102/min, and respirations are 31/min. An echocardiogram performed on the second hospital day reveals an akinetic region of the anterior wall. What is the most likely explanation for this patient's deterioration?
. Pericardia! tamponade
. Pulmonary embolism
. Rupture of ventricular septum
. Papillary muscle dysfunction
. Acute aortic dissection
.45) A 34-year-old female presents to your office complaining of pressure-like, substernal chest pain that has been affecting her recently when she plays active sports. Resting consistently alleviates the pain. She denies any associated nausea, vomiting, diaphoresis, dyspnea, palpitations or syncope. Family history is non-contributory. On physical examination, her pulse is 79/min and blood pressure is 130/70 mmHg. Cardiac auscultation reveals a high-pitched 3/6 systolic murmur best heard at the second right intercostal space. The lungs are clear to auscultation. Chest x-ray shows a normal sized heart and clear lung fields. What is the most likely cause of this patient's chest pain?
. Anomalous origin of the right coronary artery
. Atherosclerotic narrowing of the coronaries
. Increased myocardial oxygen demand
. Increased myocardial oxygen extraction
. Stretching of the papillary muscles
.46) A 48-year-old Caucasian male presents to your office complaining of progressive exertional dyspnea. It has become especially bothersome over the past two months. Presently, he becomes short of breath after climbing one flight of stairs. He denies any significant problems in the past. He is not taking any medications and he denies smoking or drinking alcohol. His temperature is 37.2°C (98.9°F), pulse is 78/min, blood pressure is 130/75 mmHg and respirations are 14/min. Chest examination reveals a harsh systolic murmur that is best heard at the right second intercostal space with radiation along the carotid arteries. An S4 is heard at the apex. Based on these findings, what is the most likely cause of this patient's symptoms?
. Hypertrophic cardiomyopathy
. Myxomatous valve degeneration
. Rheumatic heart disease
. Bicuspid aortic valve
. Senile calcific aortic stenosis
.47) A 45-year-old man presents to the emergency department because of dyspnea, fatigue, poor appetite and weight gain over the past several weeks. He says that about four weeks ago he began to develop worsening shortness of breath with exertion and more recently has been waking at night with breathlessness. He also notes that it is sometimes difficult for him to open his eyes in the morning due to facial edema. He has no significant past medical history and he takes no medications. On physical examination, his blood pressure is 200/120 mmHg and his heart rate is 100/min. You note generalized bodily edema and distention of his jugular veins while he is sitting upright. On lung auscultation you hear bibasilar rales. Urinalysis shows trace protein, no nitrites, trace leukocyte esterase, 50+ red blood cells and occasional neutrophils. Which of the following is the most likely cause of this patient's edema?
. Renal hypoperfusion
. Hypoalbuminemia
. Extensive glomerular damage
. Portal hypertension
. Hypothyroidism
.48) A 14-year-old African American male collapses and dies while playing basketball at a school tournament. He has no known past medical history. Which of the following is the most likely underlying disease in this patient?
. Hypertrophic cardiomyopathy
. Coronary atherosclerosis
. Aortic aneurysm rupture
. Ventricular septal defect
. Bicuspid aorta
.49) A 46-year-old man complains of exertional dyspnea and dry cough. He also describes occasional episodes of a suffocating night-time cough that is relieved only when he stands up. His medical history is significant for a myocardial infarction six months ago. His current medications are metoprolol, aspirin and simvastatin. He does not use tobacco but drinks alcohol on social occasions. His father died of a stroke and his mother suffers from diabetes mellitus. His blood pressure is 150/100 mmHg and his heart rate is 60/min. Chest examination reveals bibasilar rales. His cardiac apex is palpated in the sixth intercostal space. The liver span is 12 cm. Bilateral pitting leg edema is also present. Which of the following most likely contributes to his edema?
. Constriction of the renal arterioles
. High sodium delivery to the distal tubule
. Increased renal blood flow
. Increased renal potassium loss
. High portal venous resistance
.50) A 54-year-old man with a 20-year history of chronic obstructive lung disease has a heave that is palpable at the lower left sternal border at the third, fourth, and fifth intercostal spaces. Which of the following best explains the etiology of the heave?
. It is probably a displaced point of maximum impulse (PMI)
. It means the patient has congestive heart failure
. It means that the patient has aortic stenosis
. It means the patient has right ventricular hypertrophy
. It means the patient has a pericardial effusion
{"name":"P 427 p 444 *No 1 to 50 *", "url":"https://www.quiz-maker.com/QPREVIEW","txt":"1) A 74-year-old man presents to your office for a routine. He has no present complaint. His medical history is significant for right knee osteoarthritis. He takes naproxen occasionally, to relieve knee pain. He does not smoke or consume alcohol. His BP is 165\/75 mmHg and PR is 70\/min. The physical examination showed a mild systolic ejection type murmur at the base of the heat to the right. An E-KG revealed left ventricular hypertrophy and secondary ST segment and T wave change. Moderate left ventricular hypertrophy, without any flow abnormalities, was demonstrated on echocardiography. The ejection fraction was 60%. What is the most probable cause of hypertension in this patient?, .2) A 47-year-old woman loses consciousness for 2 minutes while shopping in a supermarket. In the emergency room, she recounts feeling nausea and warmth spreading over her body immediately before passing out. She has never had a similar episode before. She has not seen a doctor for several years and does not take any medications, nor does she use tobacco, alcohol or drug. Her family history is unremarkable. Which of the following most likely caused this episode?, .3) A 25-year-old woman experiences sudden-onset palpitations and generalized weakness. During this episode, her blood pressure is 100\/60 mmHg and her heat rate is 160\/min and regular. She has no significant past medical history and does not take any medications. She reports having a few similar episodes in the past which she has self-treated by immersing her face in cold water. Generally, she says, cold water immersion relieves her symptoms within several minutes. This cold water therapy works by affecting which of the following?","img":"https://www.quiz-maker.com/3012/images/ogquiz.png"}
More Quizzes
Riddles
15810
EMOJI QUIZ: Can you name these Derby winners?
1050
Do you have any recommendations in new papers today?
100
C-12
50250
What Must Occur for Bacterial Conjugation? Challenge
201084848
Ultimate Computer Network Online Test - Challenge Yourself!
201024191
Free French Comprehension Practice
201028088
What TV Series Should I Watch on Netflix? Take the
201032237
Think You Know the Philadelphia Flyers? Ultimate NHL Trivia
201035427
Free Language Identification: Test Recognition Skills
201022871
ACES Transfer Orientation
15823414
Technology Strategy
15825036